Secondary & Adult Cleft Lip Repair Before & After Photos
Secondary Cleft Lip Repair Before & After 1
However, if nasal obstruction and symptoms are severe, nasal reconstruction before jaw surgery is sometimes done, knowing that a second surgery may be needed after the maxilla is moved forward.
Here, septal deviation and airway collapse led to nasal obstruction, sleep apnea, and difficulty with daily activities.
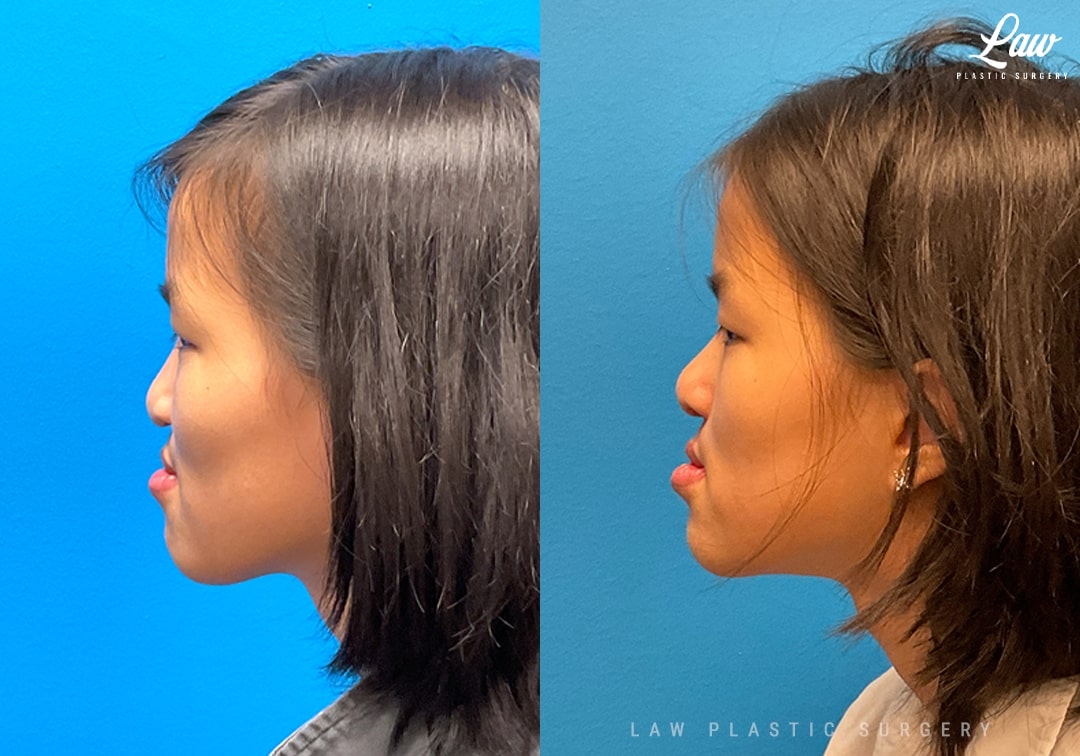
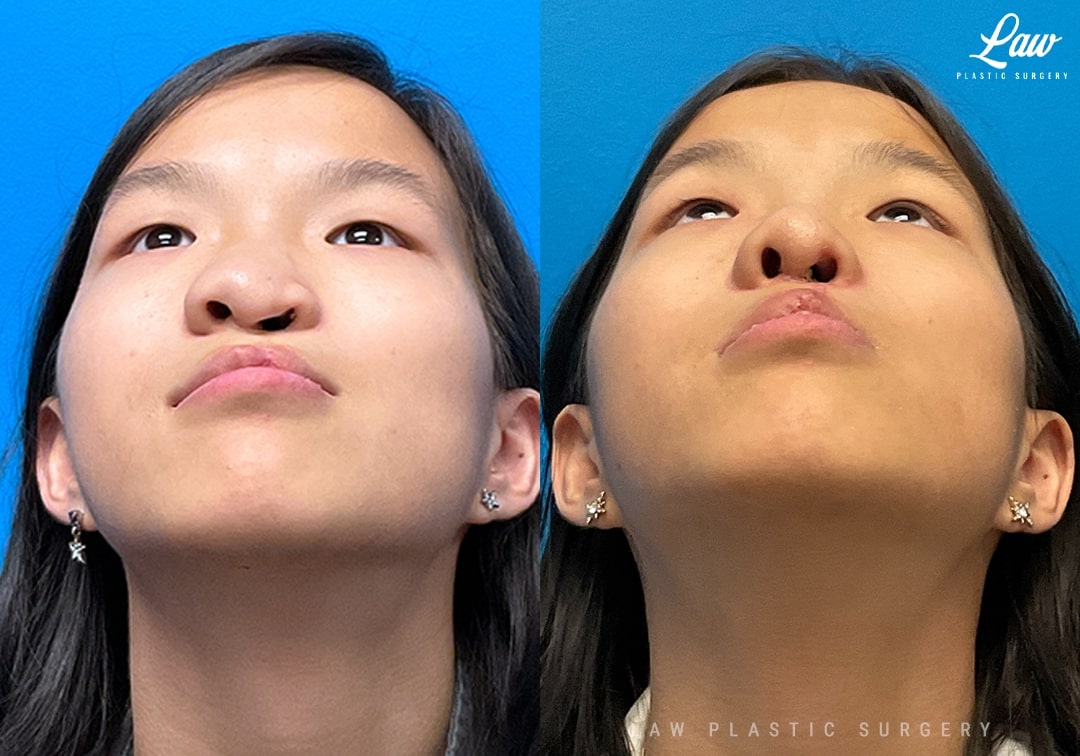
Also, her upper lip balance had room for improvement of the skin height, white roll continuity, muscle continuity for playing a brass instrument, and rolling in of the exposed wet mucosa (which otherwise cracks, bleeds, and is painful if chronically exposed).
The lip was fully taken down and re-repaired similar to a primary cleft lip repair.
Her nose reconstruction included septoplasty (reset, and resection of cartilage and bone), spreader grafts, columellar strut, tip and alar grafts, and dermal-fat graft.
She has made tremendous progress after 5 weeks, breathing well and excited to return to playing her instrument!

Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Secondary Cleft Lip Repair Before & After 2
This beautiful woman loves her boost of confidence after a cleft rhinoplasty and revision of her lip scar.
She is seen here early in her recovery, and can already breathe much more easily.
She also said we “gave her back her smile!” after revising the notch in her cleft lip.

Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Secondary Cleft Lip Repair Before & After 3
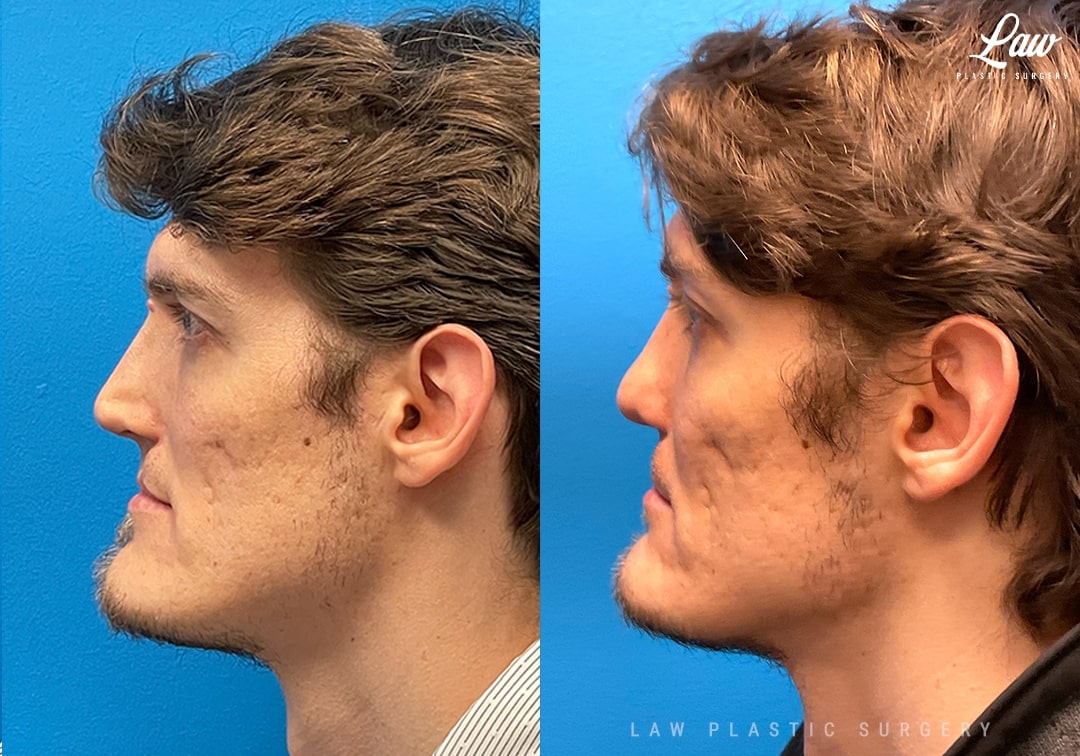
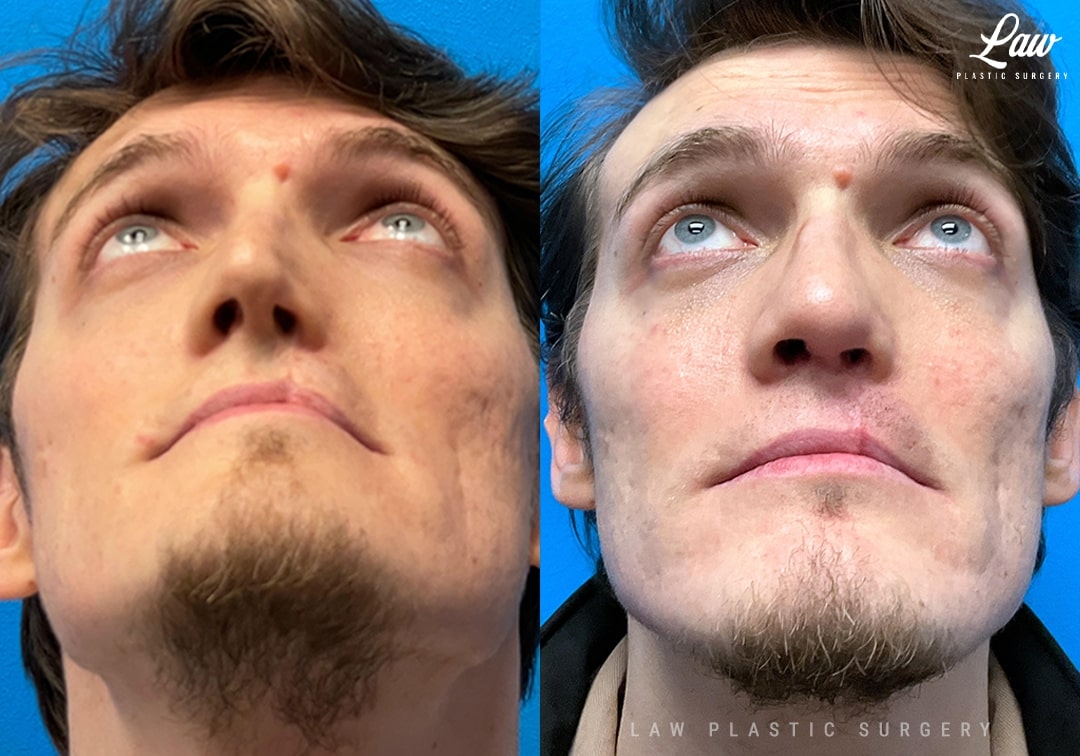
This handsome man had severe nasal obstruction and nasal asymmetry, with collapse and less growth of the left side of his nose. He also had a notch of his upper lip with some irregular scar texture.
Open rhinoplasty was performed, with release of the old scar tissue, and multiple cartilage grafts from his septum used to support his collapsed nasal passages, and to fill in the deep depression at the left alar groove.
Removing the crooked septal cartilage also helped open up his nasal airway.
The lip was re-repaired, with removal of the irregular scar tissue and improved balance of the height and width of the skin, dry mucosa, and wet mucosa, along with the underlying muscle.
Each of these components must be addressed individually, as well as all together kept in balance.
His swelling will continue to improve for at least 9-12 months, though some patients report improvement even at 18-24 months. He is seen here at 4 months.

Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Secondary Cleft Lip Repair Before & After 4
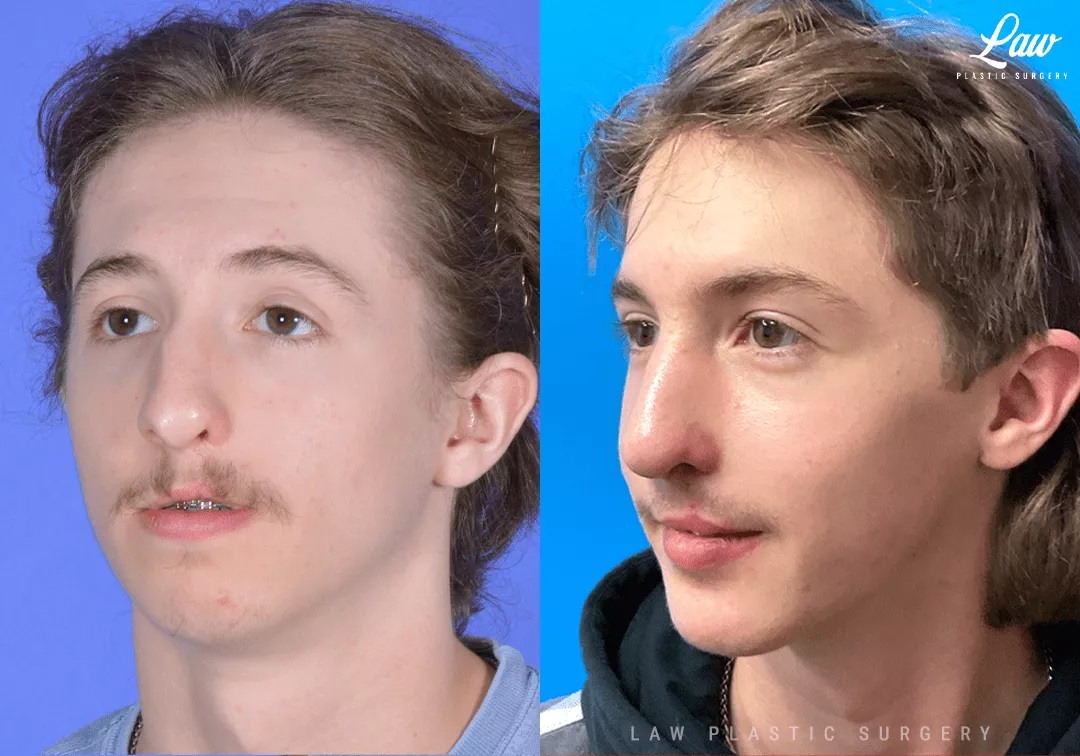
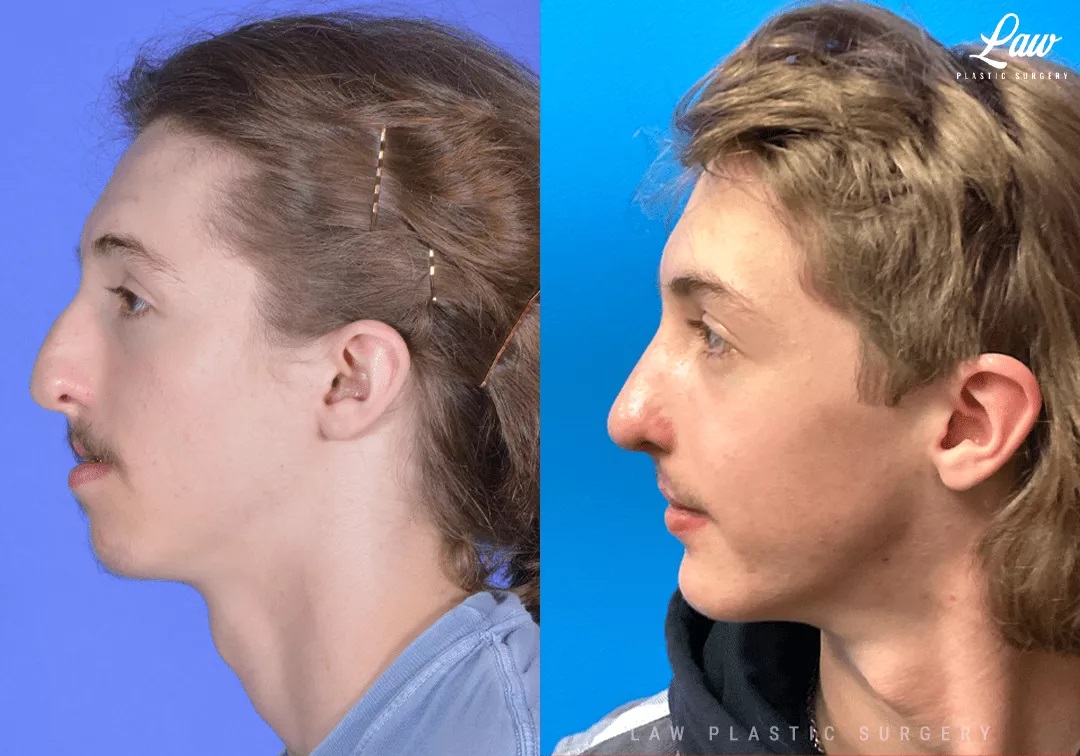
This handsome young man has a history of a unilateral cleft lip and palate.
He is seen here 7 months after jaw surgery (maxillary advancement, mandibular setback, and chin advancement), and 1 month after rhinoplasty.
His occlusion (or how his teeth fit together) is now centered and leveled, with the teeth now able to chew optimally. This will help with TMJ and dental health long-term.
The bony work also helped to balance his facial profile, giving his upper lip and chin more support.
The rhinoplasty improved his breathing by straightening the septum and supporting his nasal passages, like having a Breathe-Right strip on the inside of his nose.
His lip scar will also continue to improve after a re-repair and re-orientation of the muscle of his lip.

Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Secondary Cleft Lip Repair Before & After 5
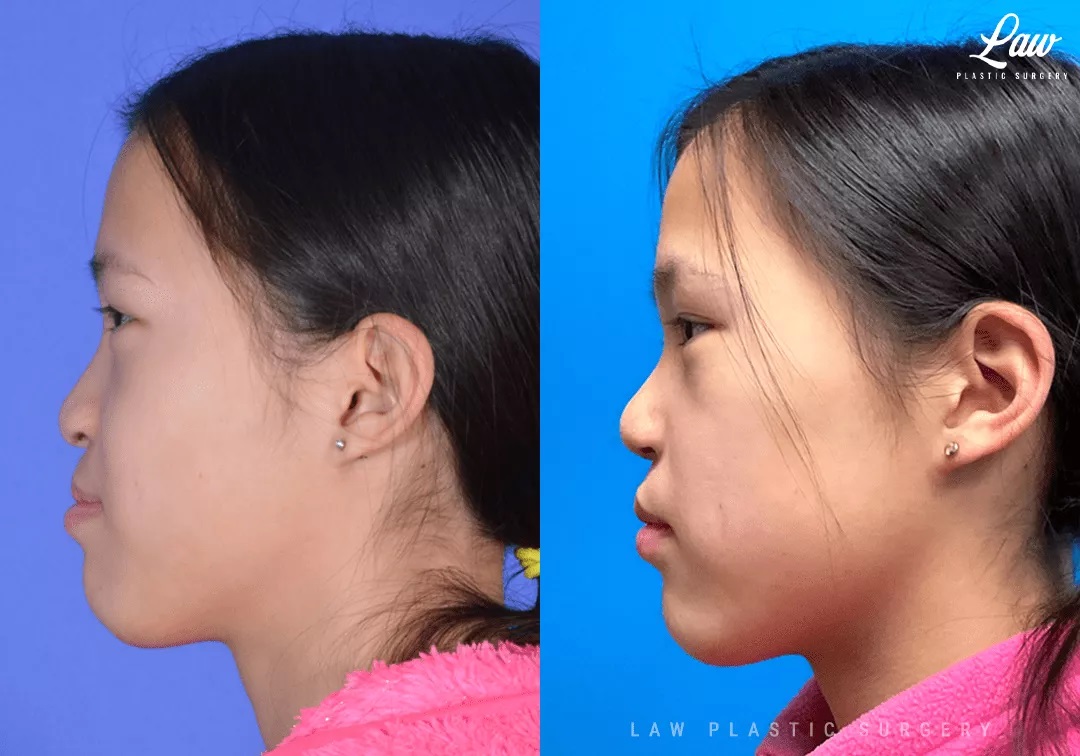
She also had some imbalance of her lip, with the height of the skin several millimeters shorter on the cleft side. This can be seen with very small imbalances magnified over years as a child grows. The scar tissue also usually does not grow as well as the surrounding skin, so even slight over-lengthening can still leave that side shorter over time.
Here, a cleft rhinoplasty and revision of the lip scar opened up her breathing tremendously. Her symmetry of the tip and wings of the nose is improved, with some upward rotation and tip support added.
Her lip was also revised, with a strong focus on not just the skin, but rebalancing the muscle height and direction of the muscle fibers.
As always, the scars will fade and flatten with time and care. She is seen here at 3 weeks after surgery.

Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Secondary Cleft Lip Repair Before & After 6
There must also be enough strength to keep the walls from collapsing in.
Here, the biggest problems were blockage by a deviated septum, and scar tissue from a lifetime of previous cleft surgeries.
The scar tissue can be thick, tighten like a lasso, and even create bands that go across from the septum in the middle to the side.
Here, these scar bands were released and reconstructed with local rearrangement (Z-plasty, V-Y advancement) for the soft tissue.
The deviated septum was straightened and resected, with special attention paid to the bone that sits further back. This bone is the most common place I find continued blockage after someone has had a previous surgery, and this area was not treated.
Support was given by rib graft to the dorsum, ear cartilage grafts to the tip, and some cartilage and soft tissue along the rim to support the external nasal valve.
The central part of the lip in the dry vermilion was also re-repaired to add some bulk here and push some of the mucosa that wants to be inside the mouth, back inside. Otherwise, this mucosa can become dry, cracked, and bleed.

Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Secondary Cleft Lip Repair Before & After 7
Often, this will improve with scar care, massage, and time.
Rarely, the scar is causing enough problems that it is worth revising it at a later time.
Sometimes, this is at the time of palate repair or bone grafting to the gum line.
Other times, a revision is done at time of rhinoplasty, or as its own procedure if severe or symptomatic like with dry, cracked mucosa.
Look for our poster on secondary lip repairs coming at the American Cleft Palate Association meeting in Denver this year!
And then on to a publication near you, later this year. Stay tuned!

Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Secondary Cleft Lip Repair Before & After 8
This made some speech articulations and graceful eating a challenge.
Anatomically, the muscle fibers here in the middle needed some reorientation across side-to-side rather than upwards in the middle.
There was also a straight band of scar tissue that made her attempts at filling unsuccessful, as the filler flowed to the softer areas on either side, making the notch even more visible.
A revision of the lip scar and muscle improved that center gap classically described as a “whistle deformity”. She is seen here at 1 month post-op.

Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Cleft Lip Repair, Secondary and Adult Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Secondary Cleft Lip Repair Before & After 9
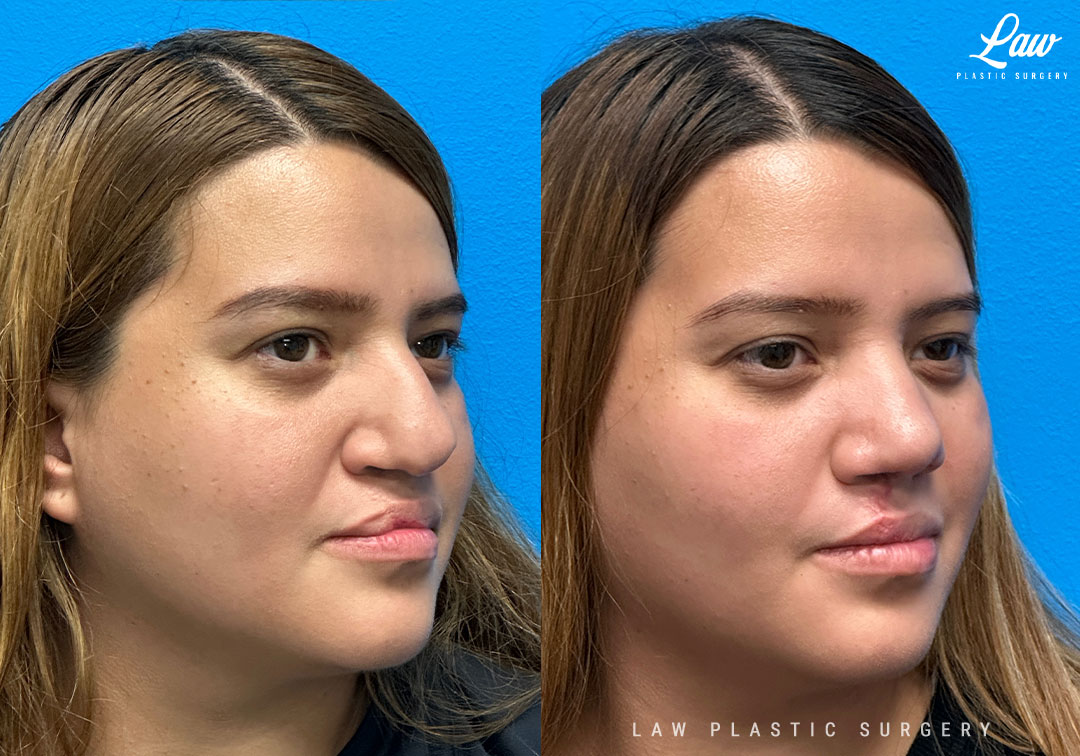
Yes, the surgery is routinely covered by insurance companies.
Any nasal obstruction that is symptomatic – cleft or no cleft – is typically covered after failing conservative treatments like nasal sprays and over the counter allergy medicines.
Similarly, the dry, chapped mucosa at the cleft lip margin may be treated under insurance to reduce exposure and symptoms, and to reduce the gap at that notch.

Cleft Rhinoplasty (Cleft Nose Surgery) Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Cleft Rhinoplasty (Cleft Nose Surgery) Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
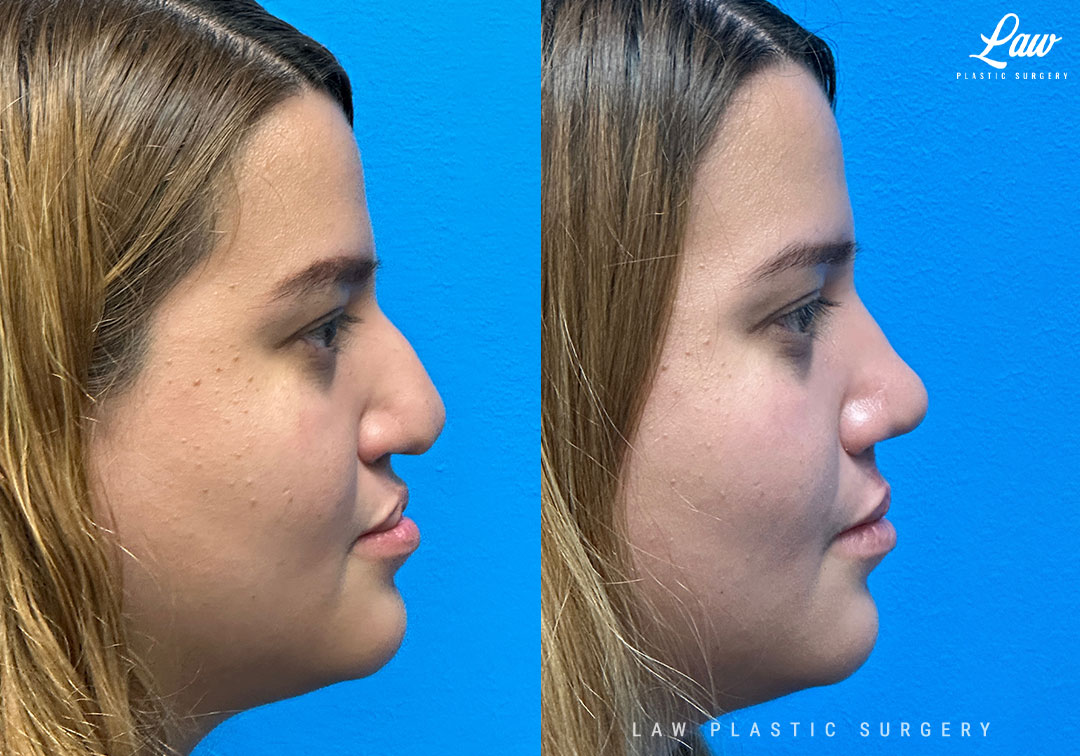
Cleft Rhinoplasty (Cleft Nose Surgery) Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Secondary Cleft Lip Repair Before & After 10
As long as the nasal passages are functional enough to allow for recovery after the jaw surgery, we will do the jaw surgery first, and let the foundation settle before working on the nose.
The goals for the nose are very individualized for each person. Some patients focus mainly on the airway, without any concern for the outward appearance.
That said, giving the nasal framework stronger and more symmetric support can be an essential part of making breathing easier.
Making the lip more symmetric with better balance between the upper and lower lip can help with speech and confidence.
Filler (usually a hyaluronic acid) can be used for a temporary boost without surgery, while fat grafting gives more long-term results, but requires harvesting someone’s fat (usually with a little bit of liposuction).
Surgery may be recommended with – or instead of – filler, depending on each person’s goals and their anatomy, including the amount of scarring, and each component of the lip (skin, muscle, and mucosa).
Swelling and scar maturation can take months to fully return to normal. Like with any surgery, most people are perhaps 85-90% back to baseline at 6-12 weeks. With prior surgeries, and the extent of some of these surgeries, that timeline can run twice as long.

Cleft Rhinoplasty (Cleft Nose Surgery) Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Cleft Rhinoplasty (Cleft Nose Surgery) Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Cleft Rhinoplasty (Cleft Nose Surgery) Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Cleft Rhinoplasty (Cleft Nose Surgery) Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
