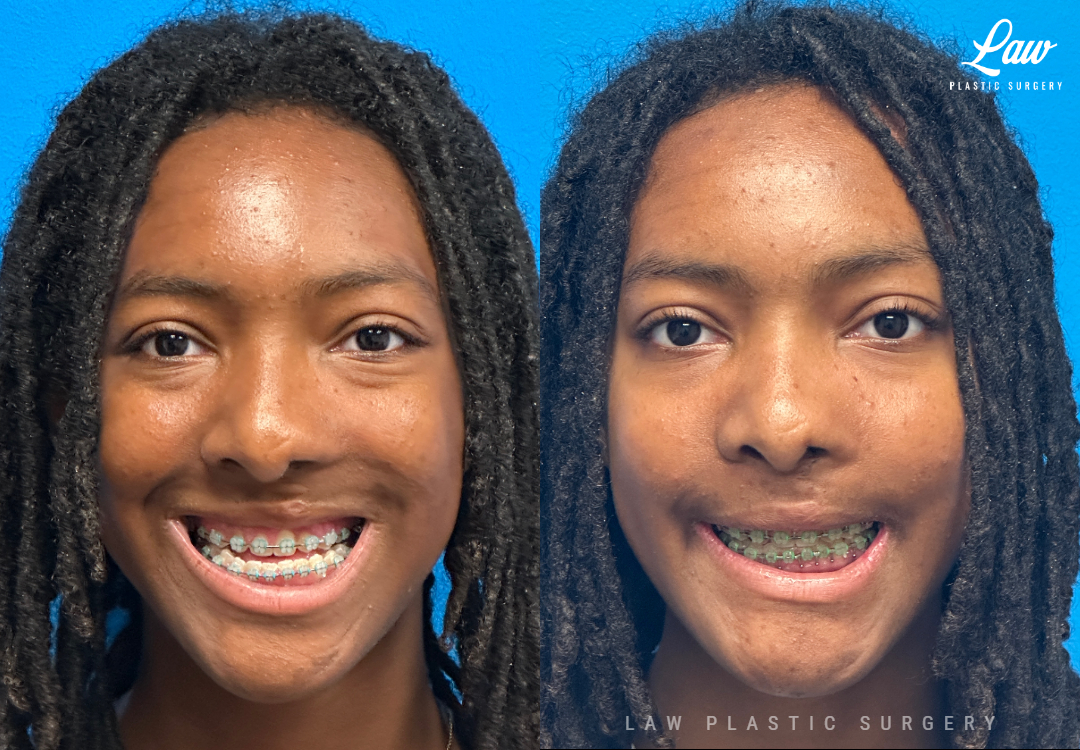Jaw Surgery Before & After Photos
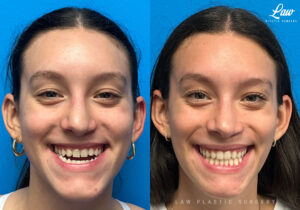
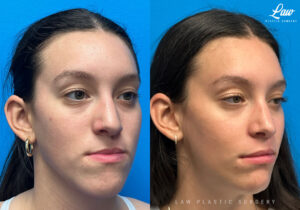
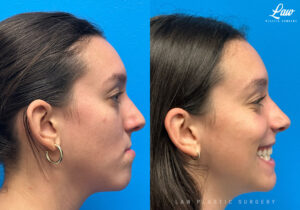
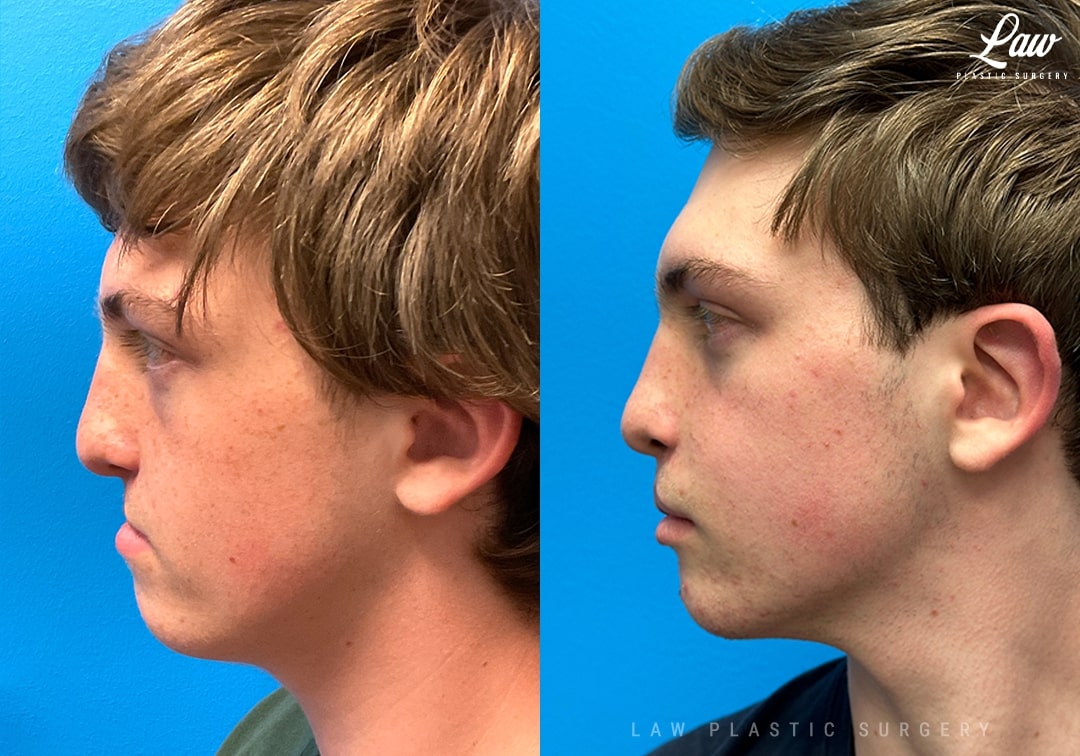
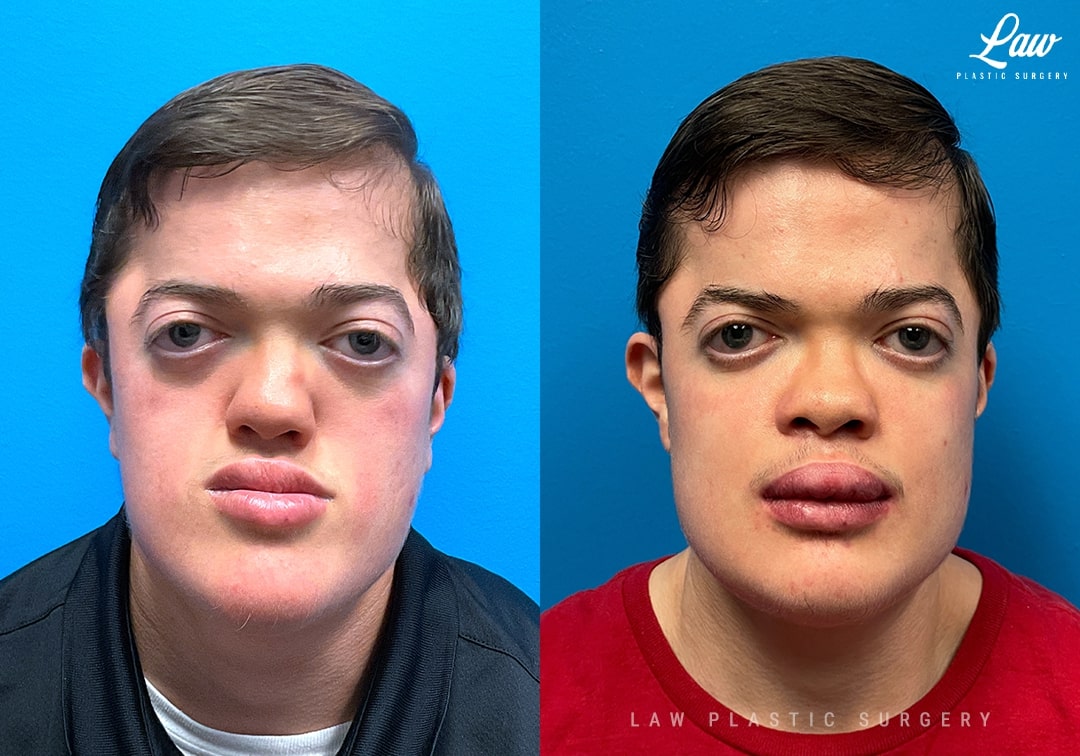
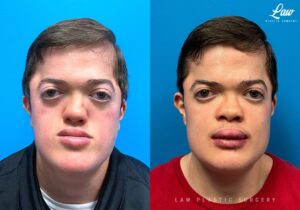
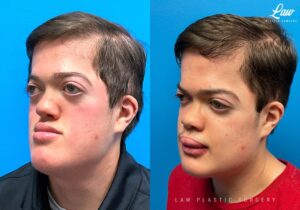
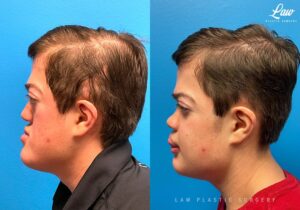
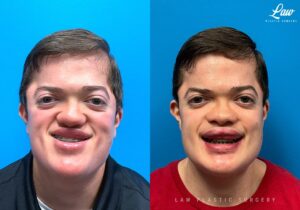
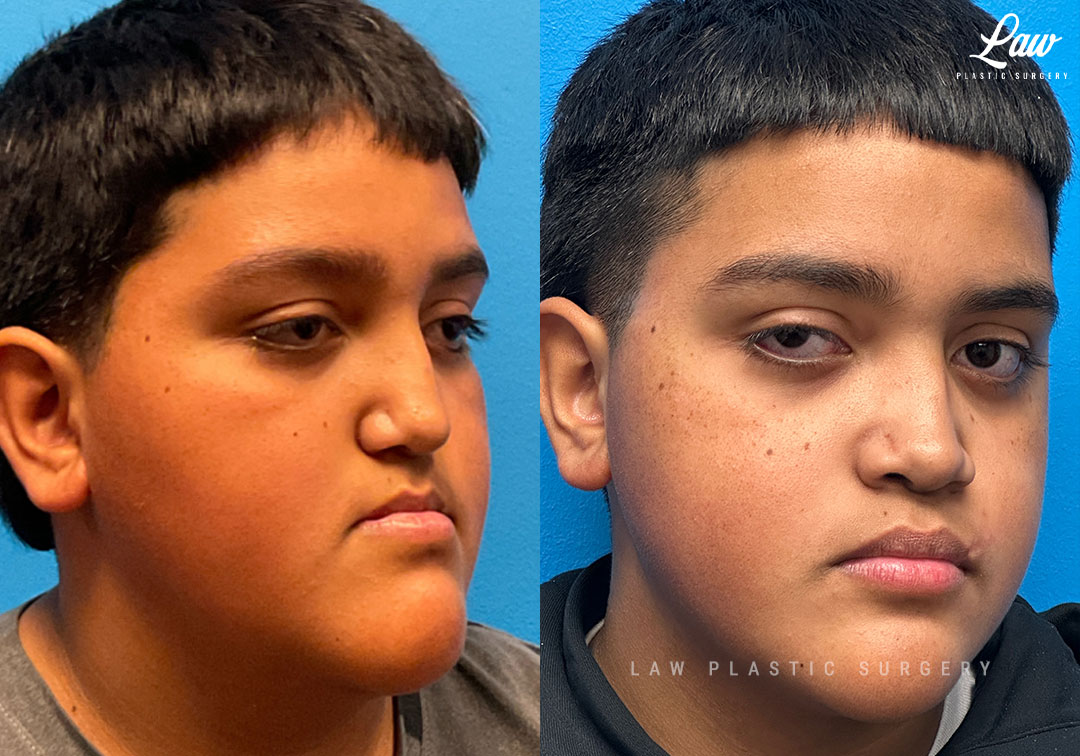
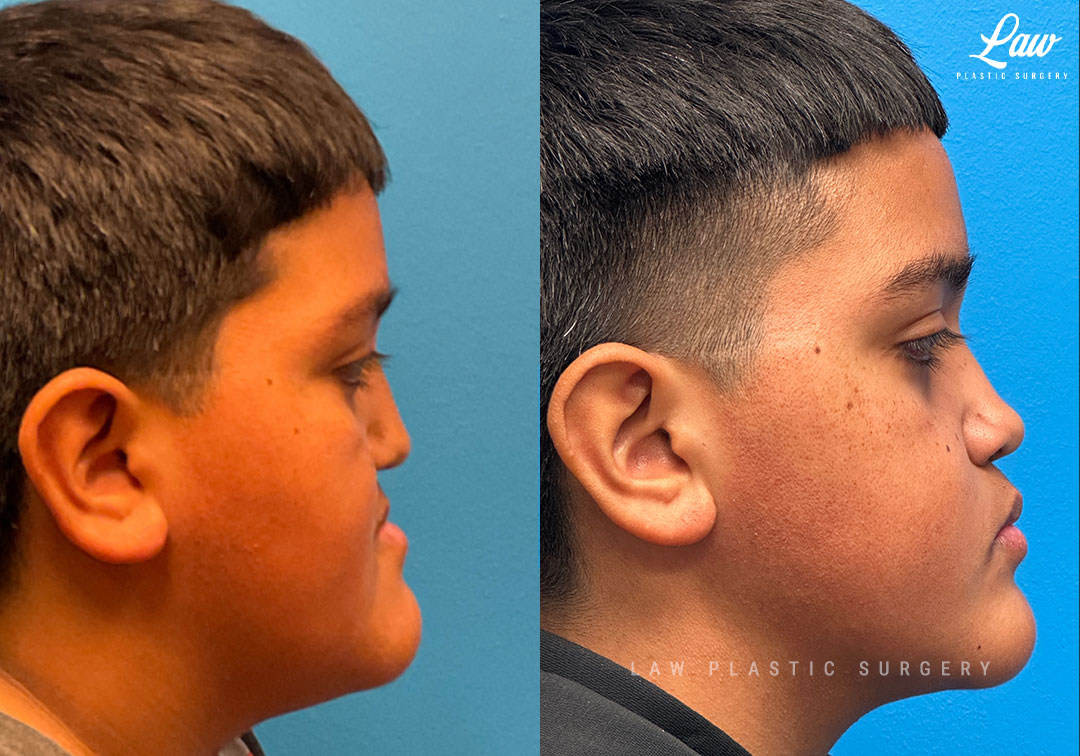
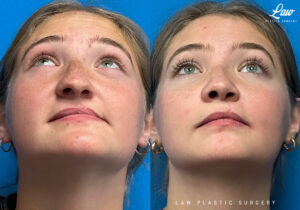
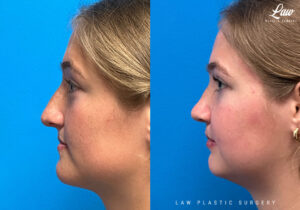
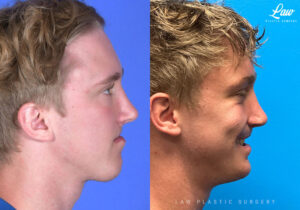
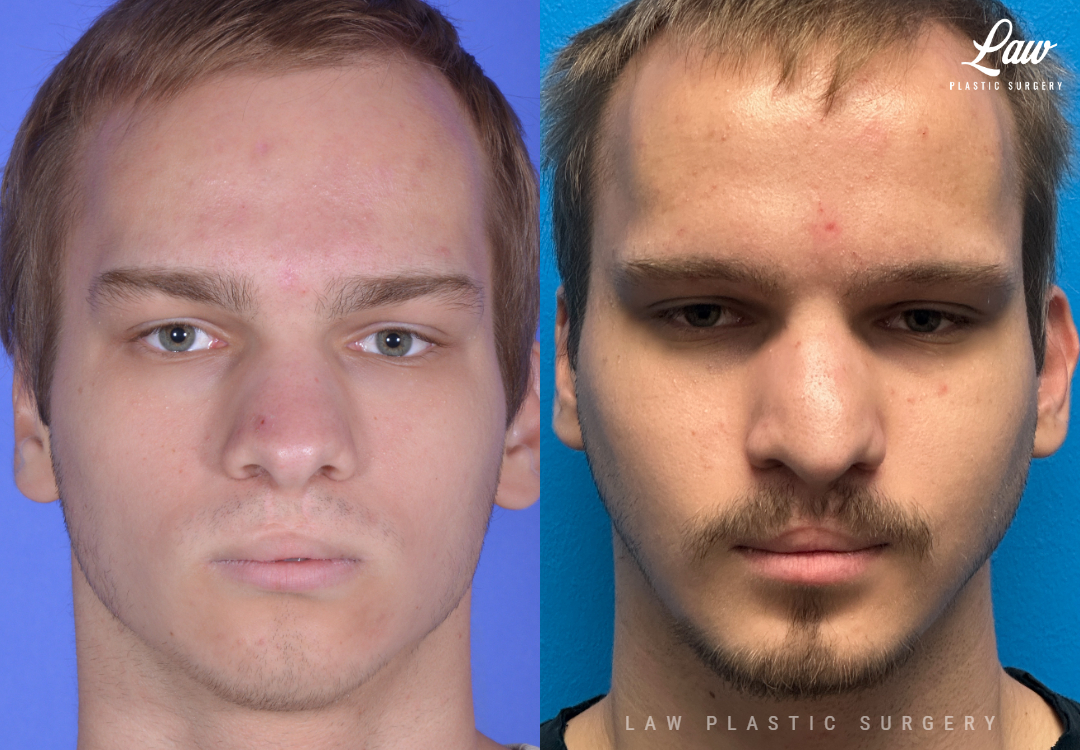
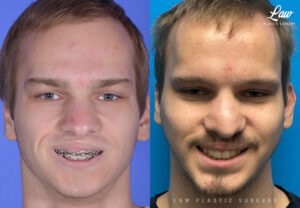
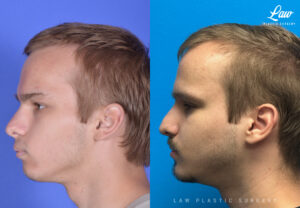
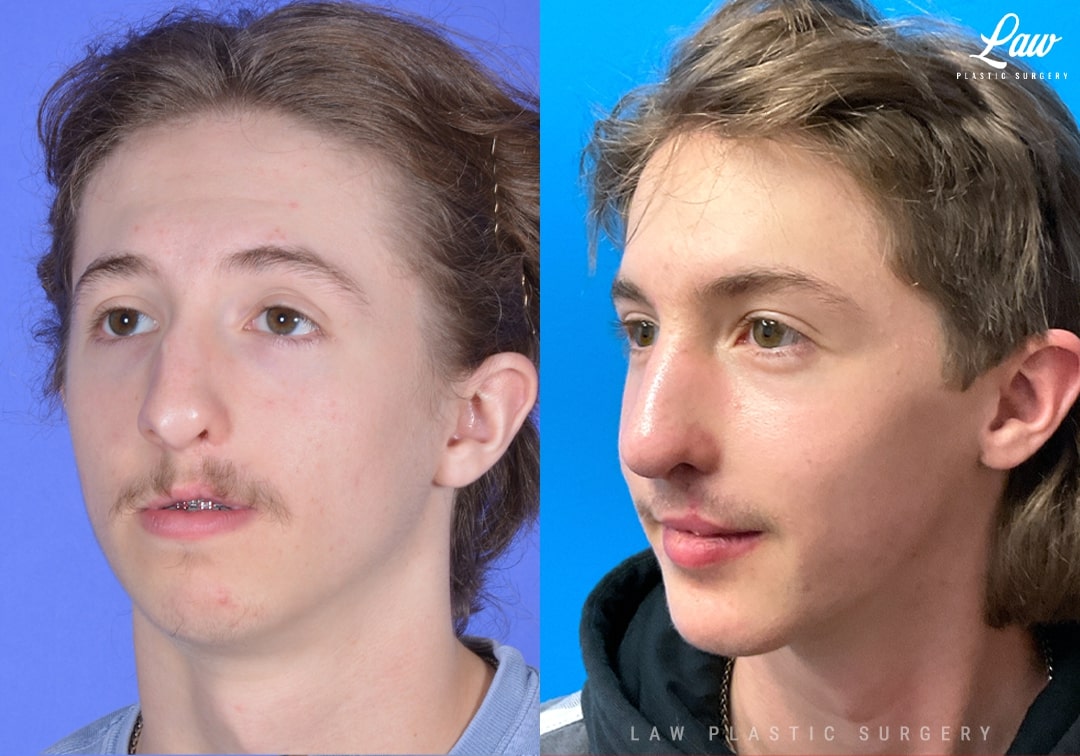
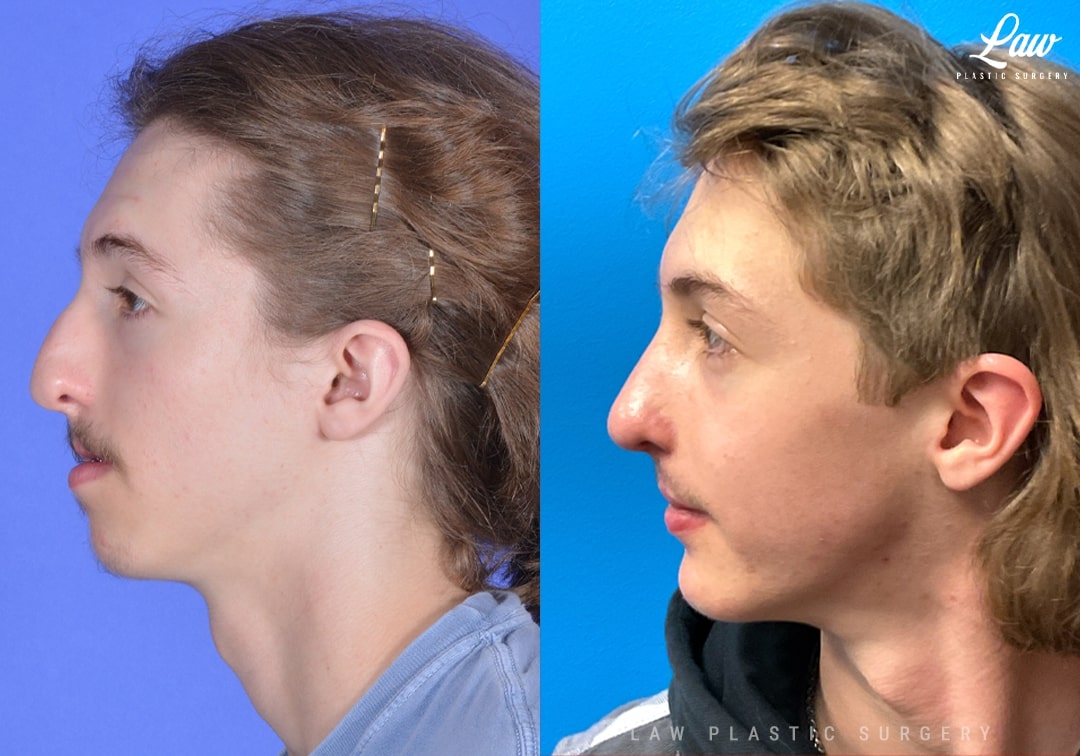
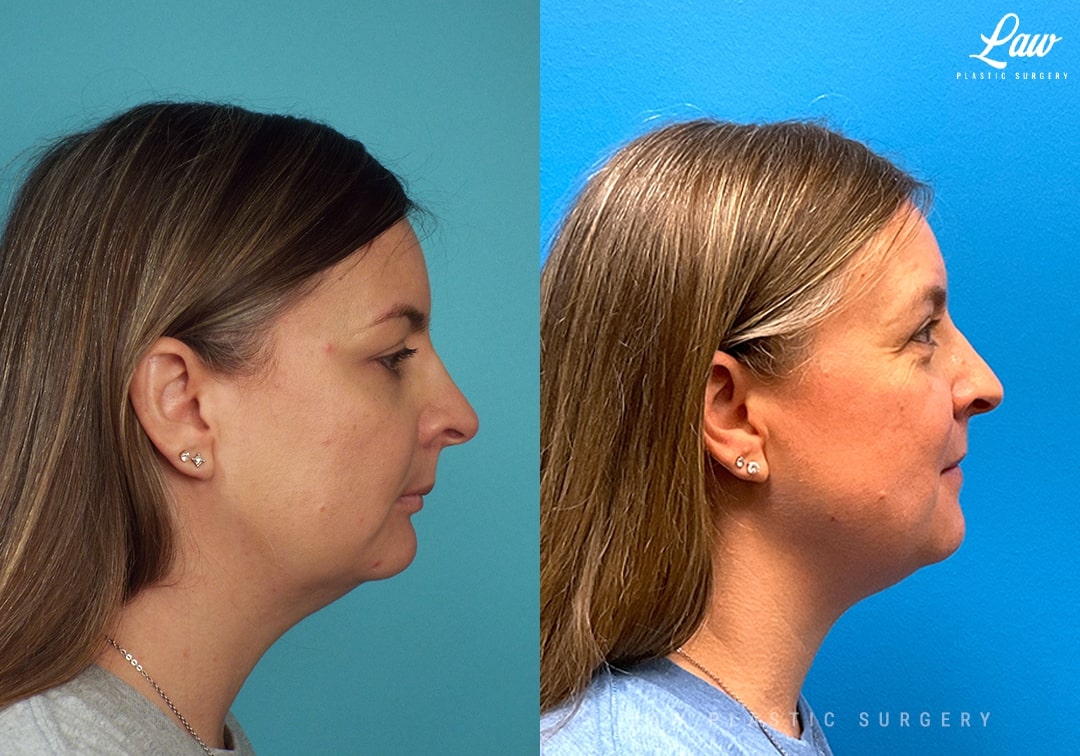
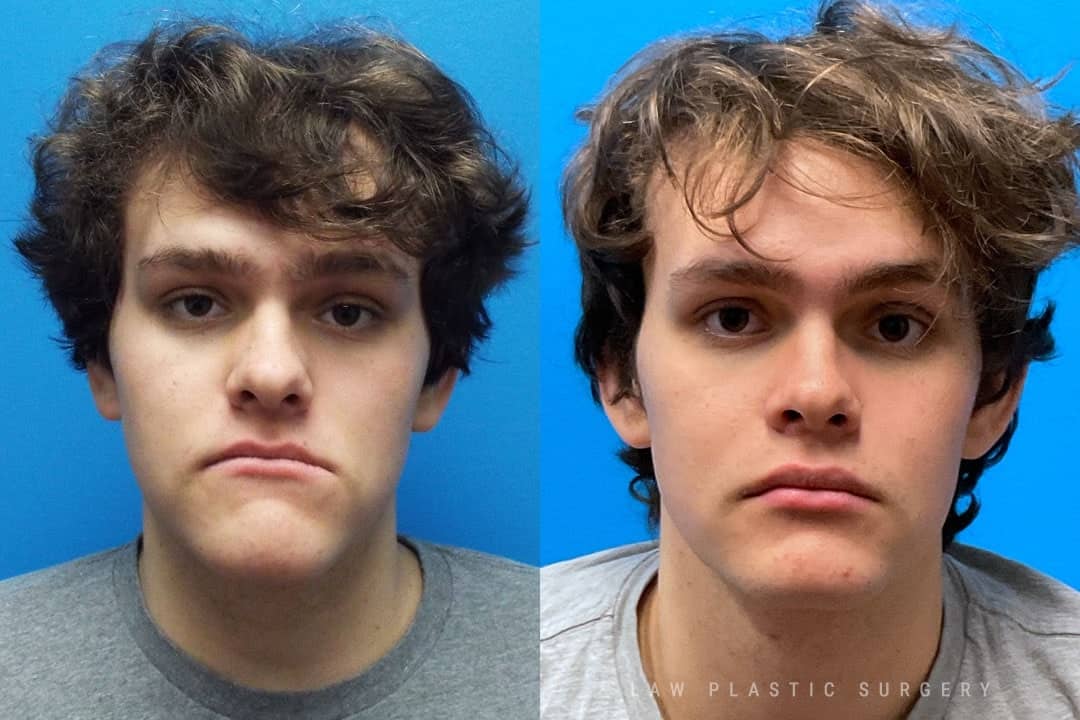
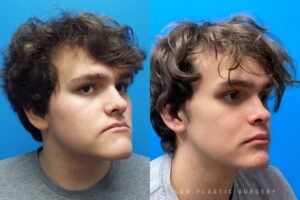
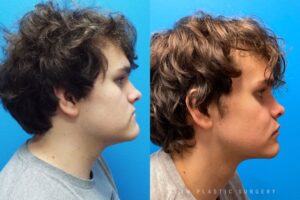
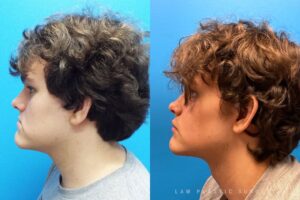
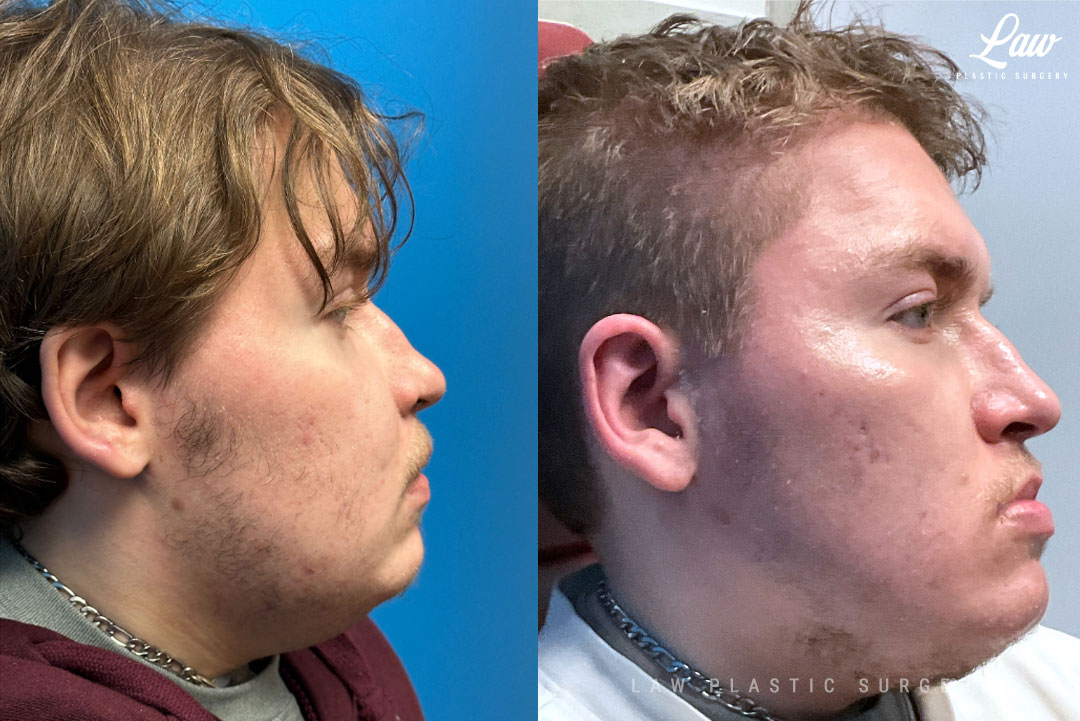
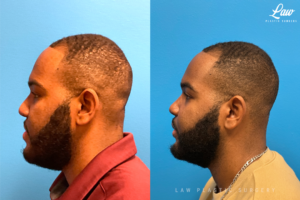
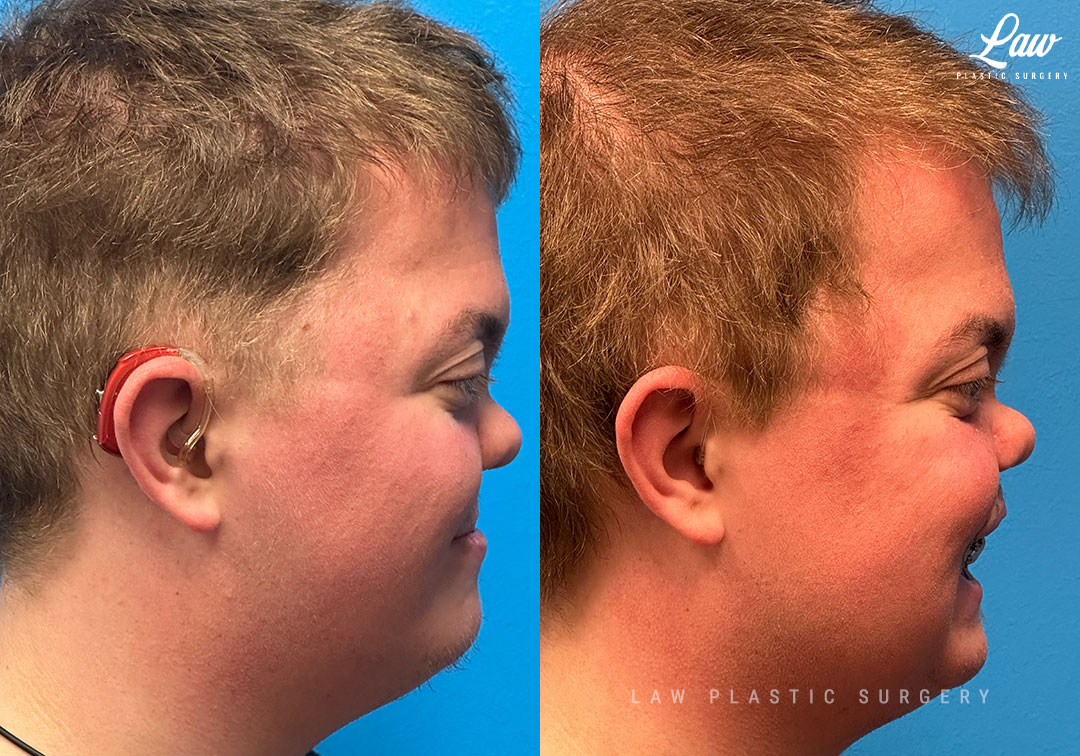
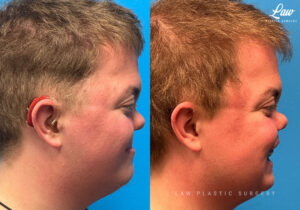
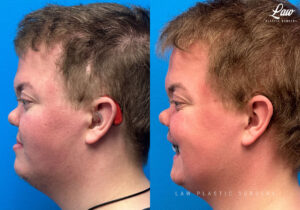
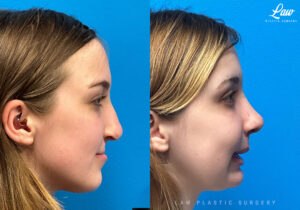
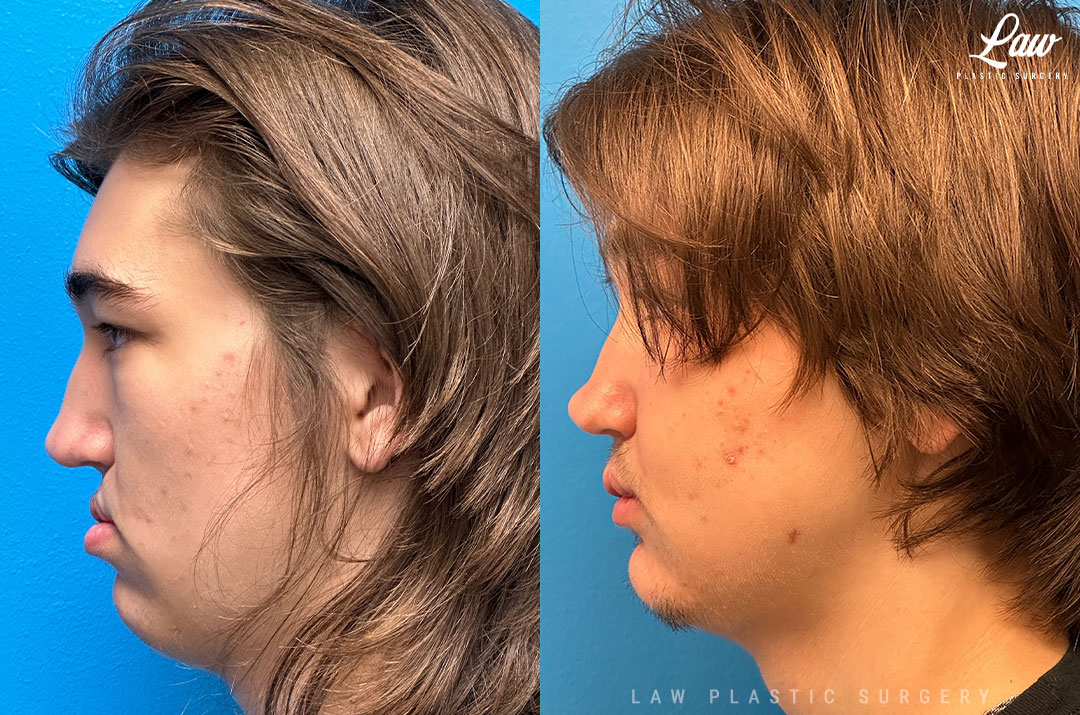
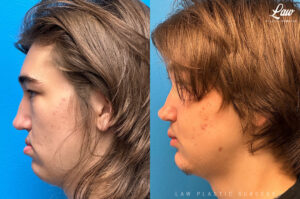
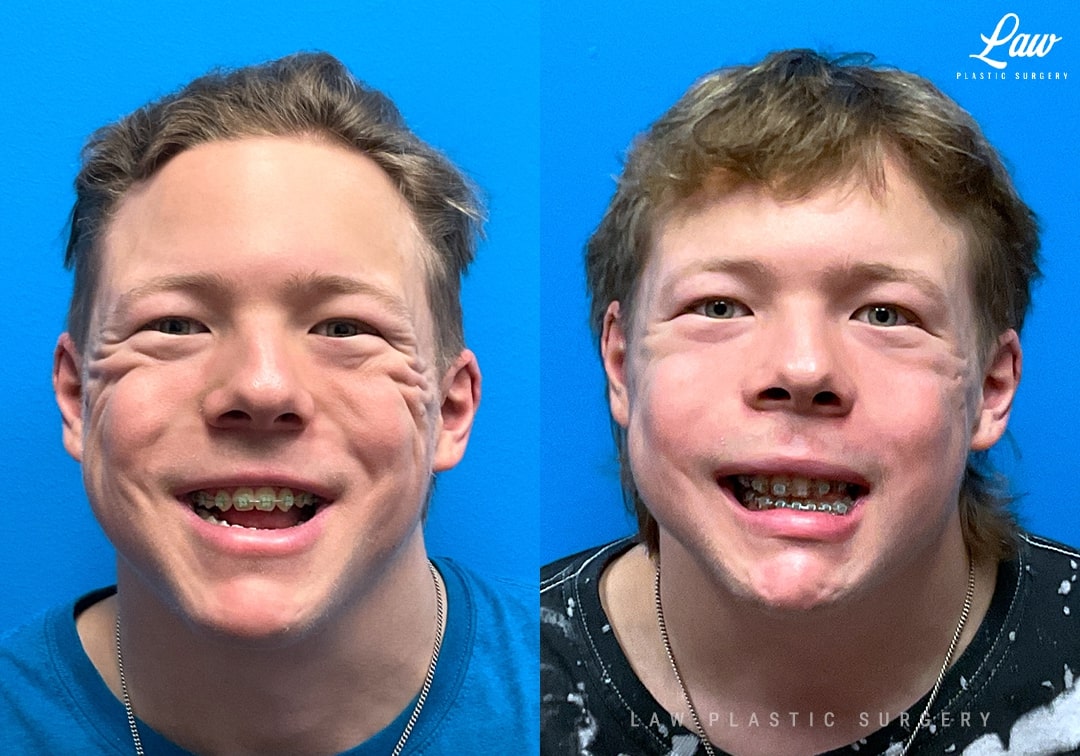
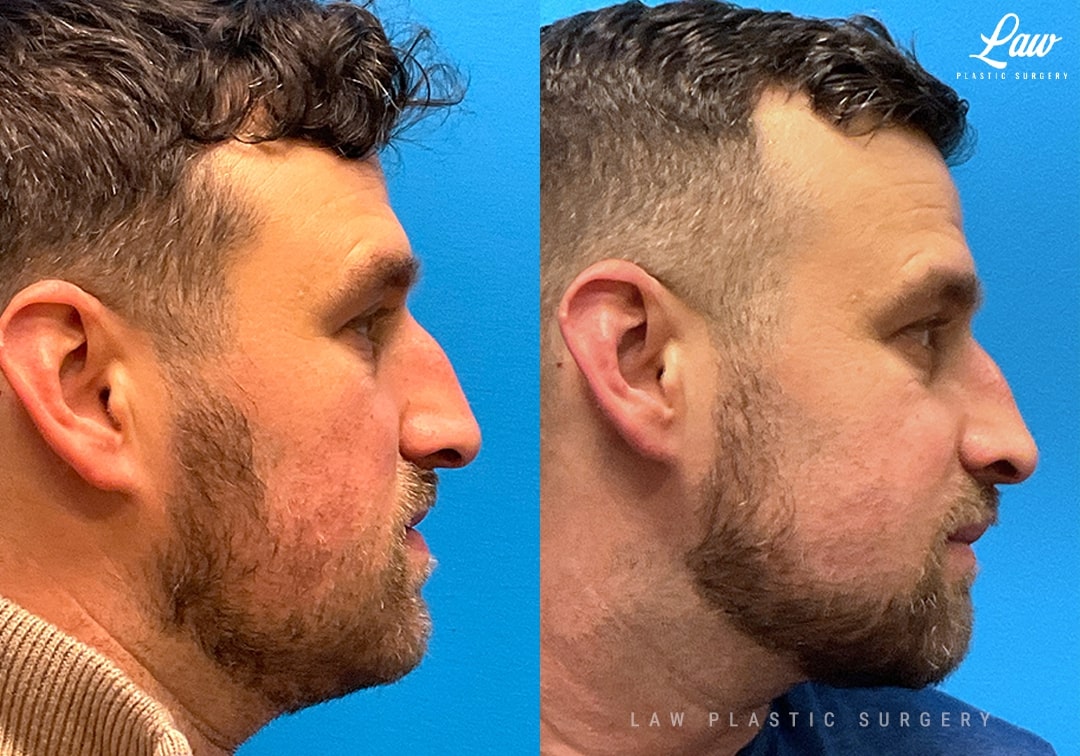
Jaw Surgery Before & After 1
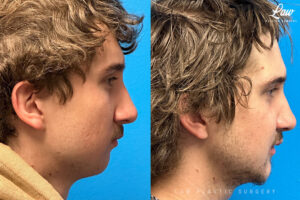
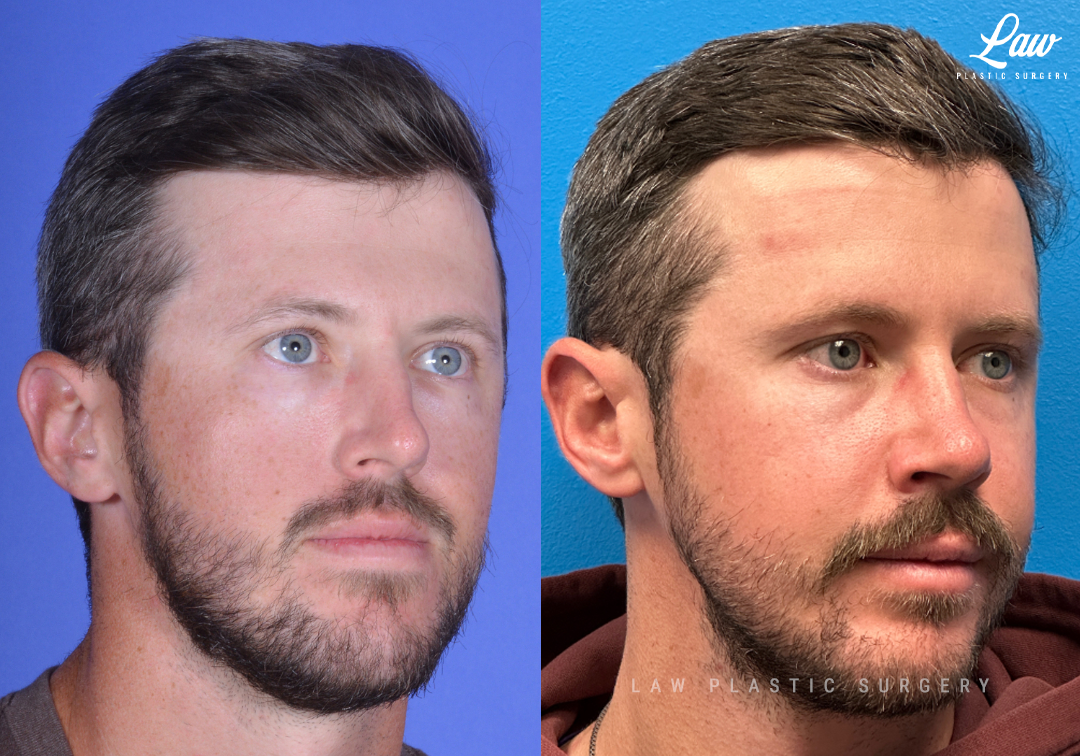
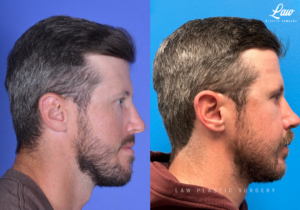
He has Gnathodiaphyseal dysplasia (distinct from osteogenesis imperfecta), a condition that caused >10 different fractures after minimal or no known trauma.
We offered jaw surgery after a thorough discussion of the risks and recovery process.
The surgery, thankfully, was a success. It included a multi-piece Lefort 1 advancement and BSSO setback.
For many years we have been using VSP (Virtual Surgical Planning) and custom 3D guides and plates. The improved consistency, accuracy, and efficiency are worth the planning time and process.
Best of all is the positive effect we can have on patients’ lives. Improved breathing, eating, speaking, and long-term dental and TMJ health, all make the surgery and recovery worthwhile when the surgery is needed.
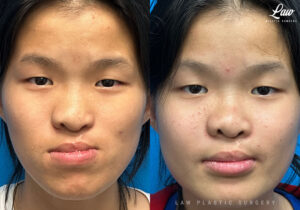
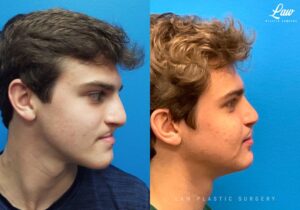
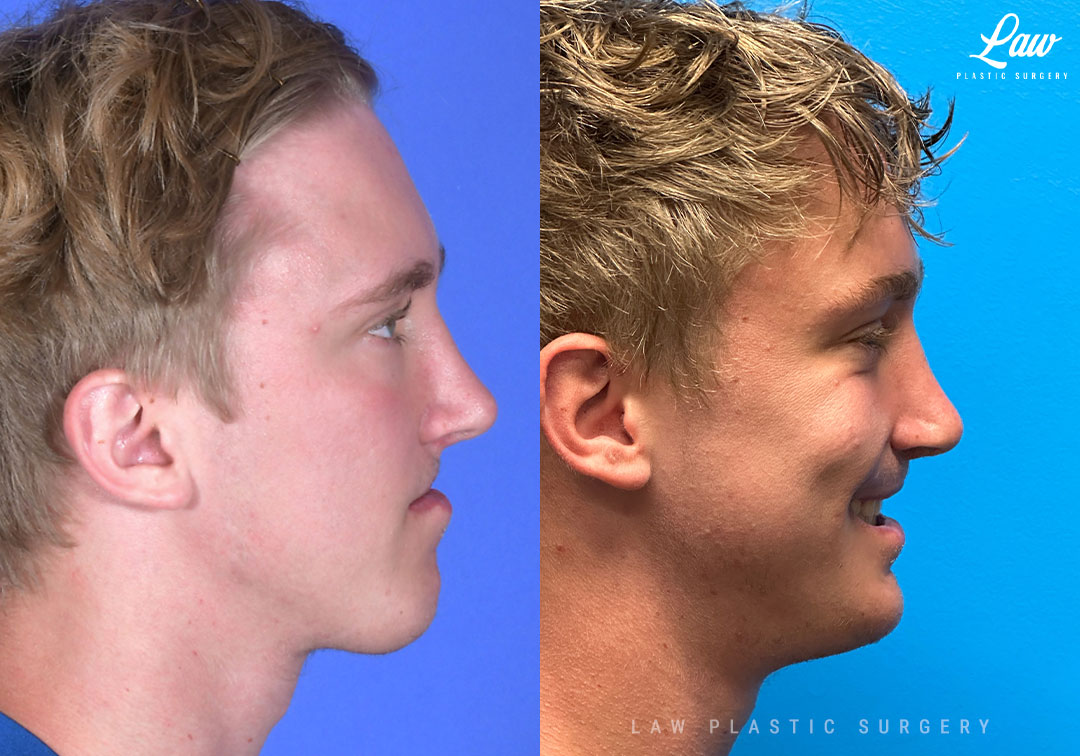
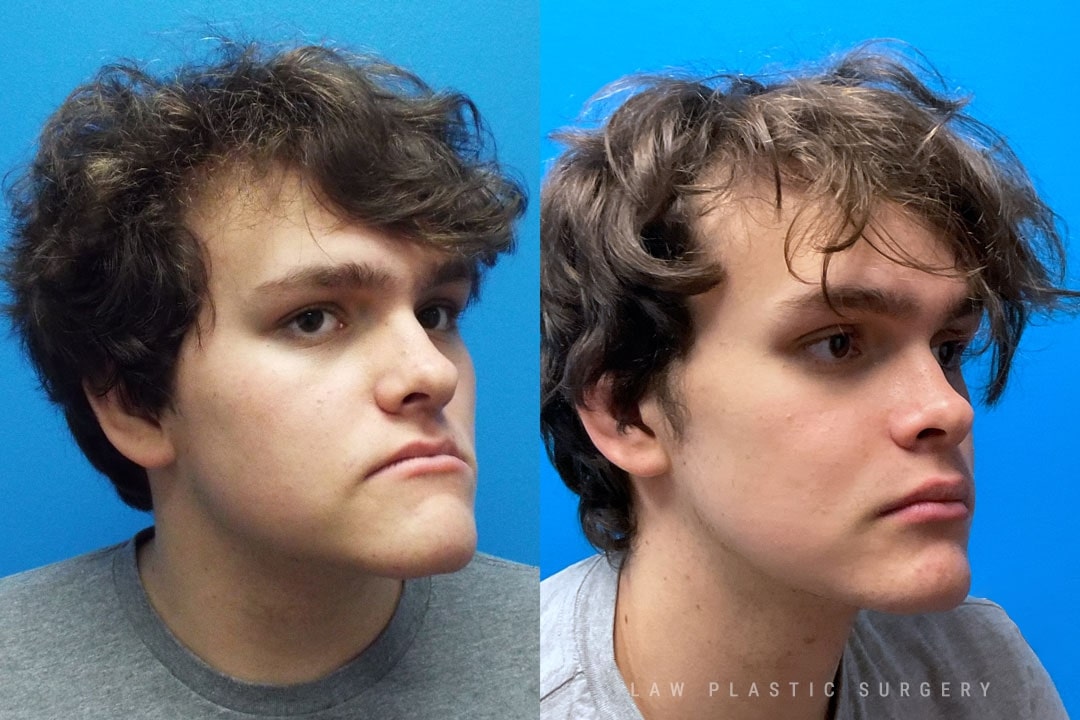
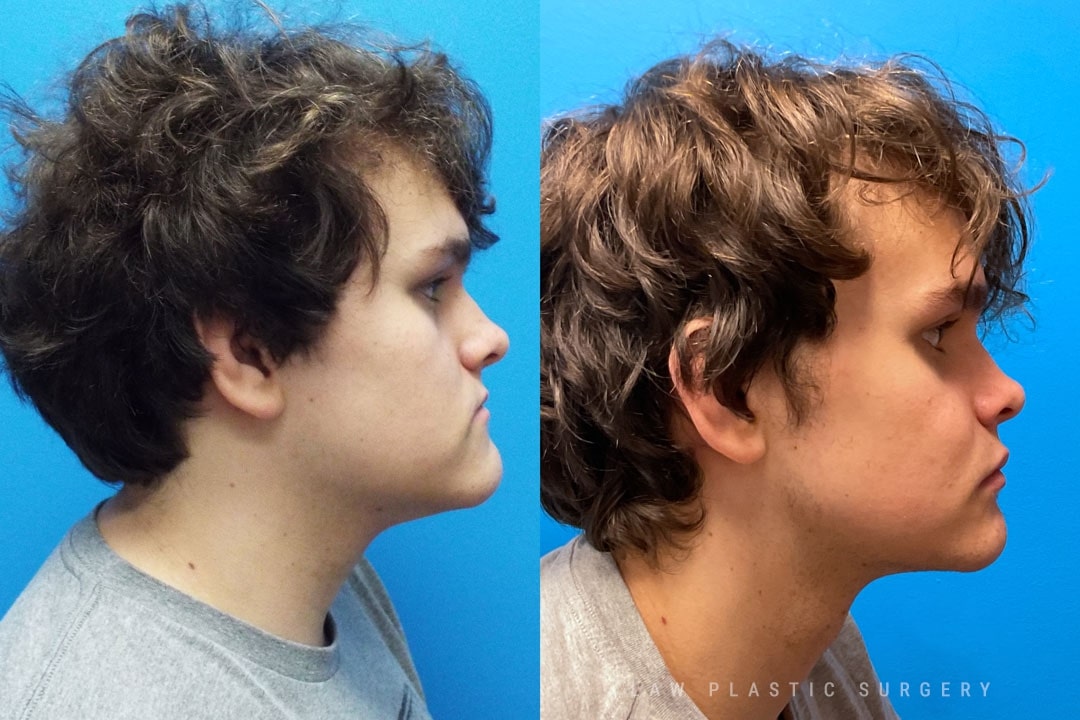
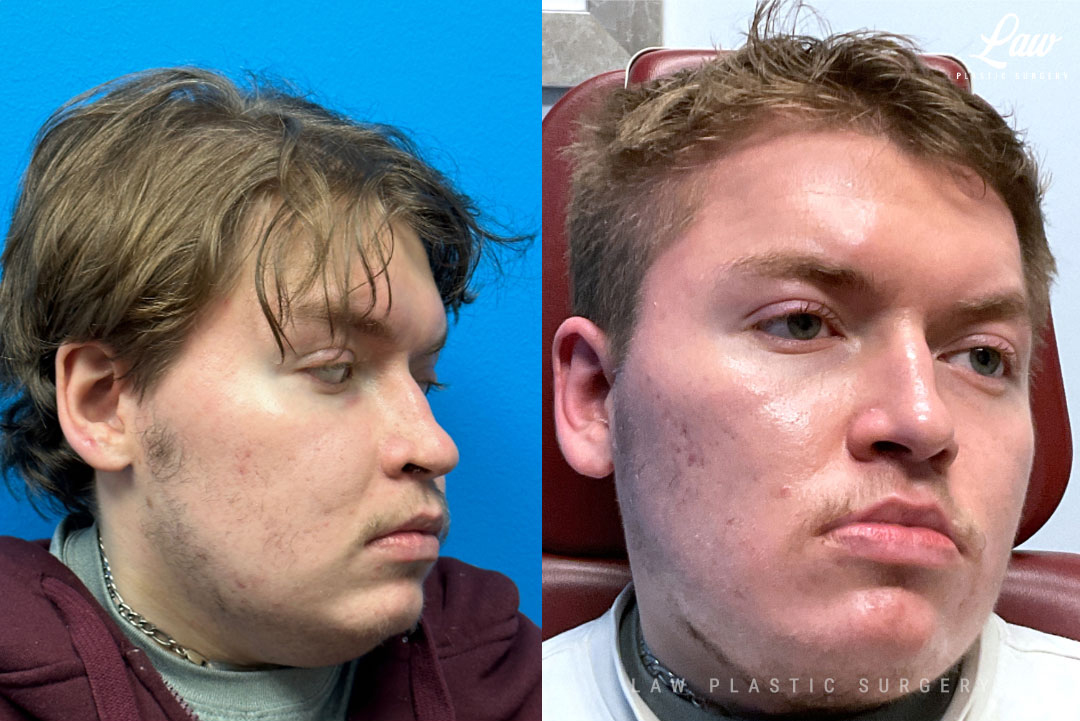
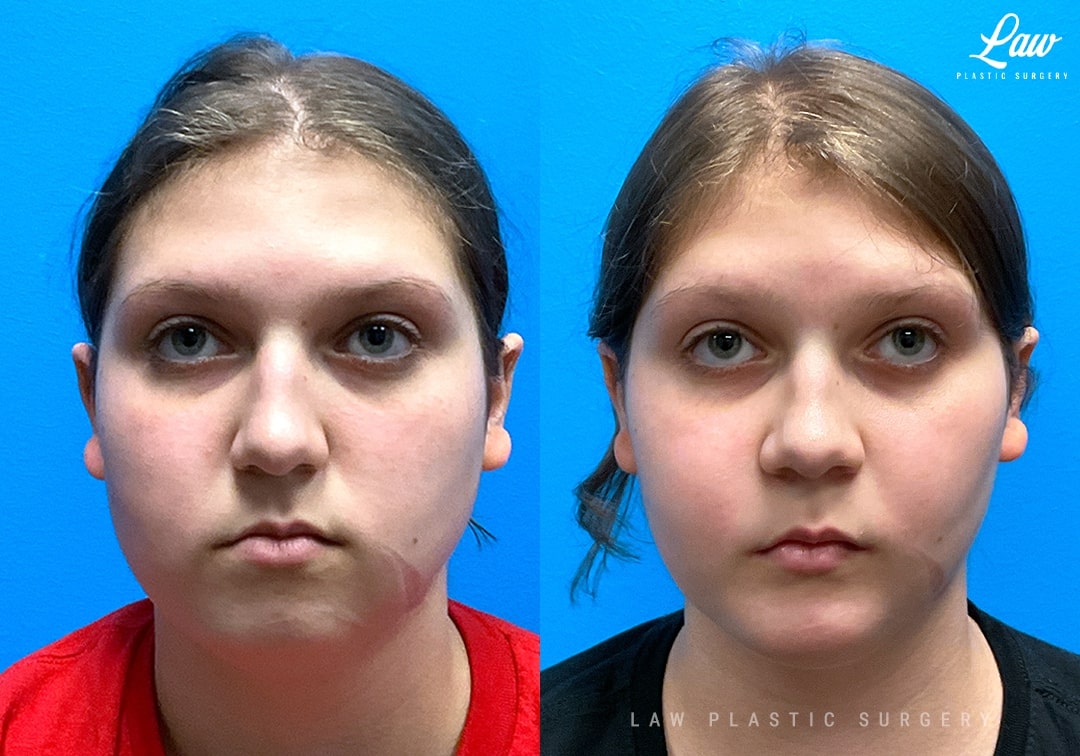
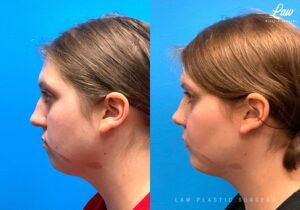
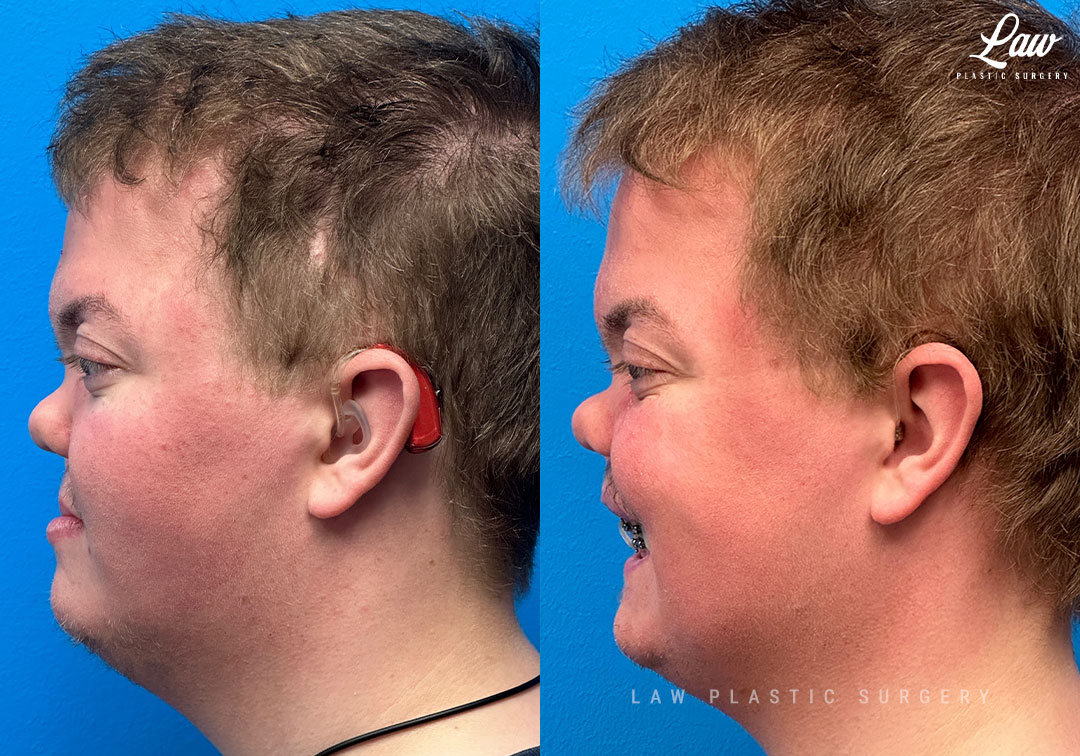
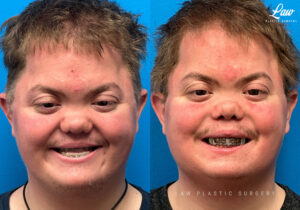
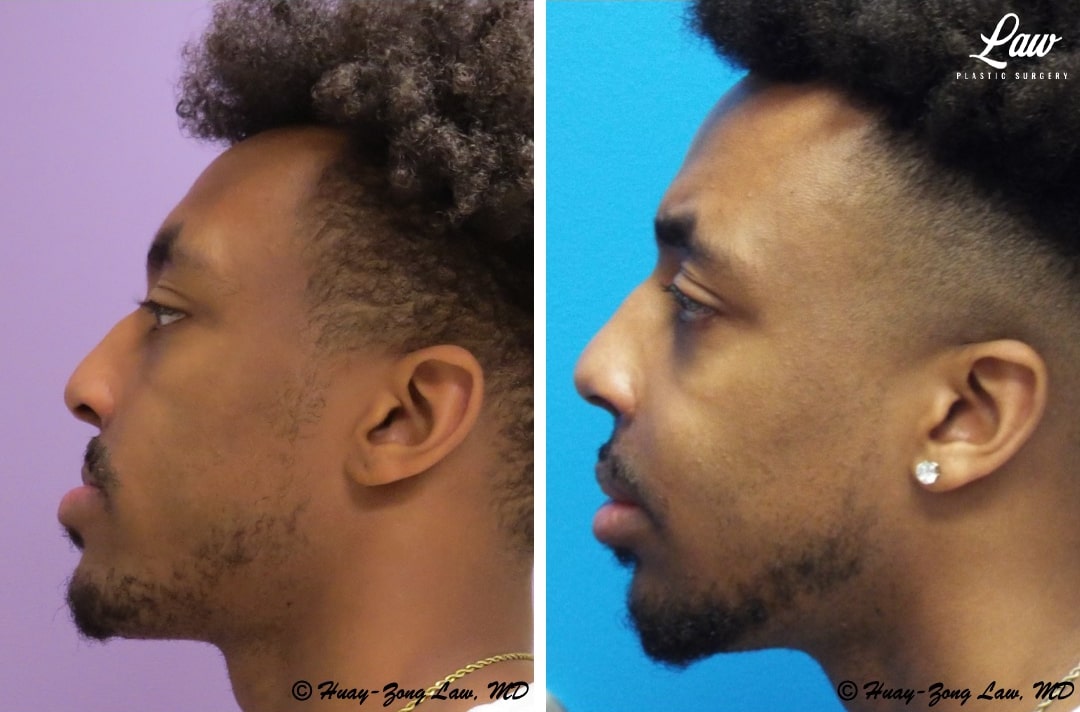
Jaw Surgery Before & After 2
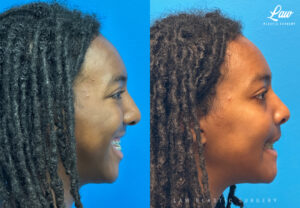
Swelling is still ~50%, but already the chin is more centered, and the jaw line more symmetric.
Key goals:
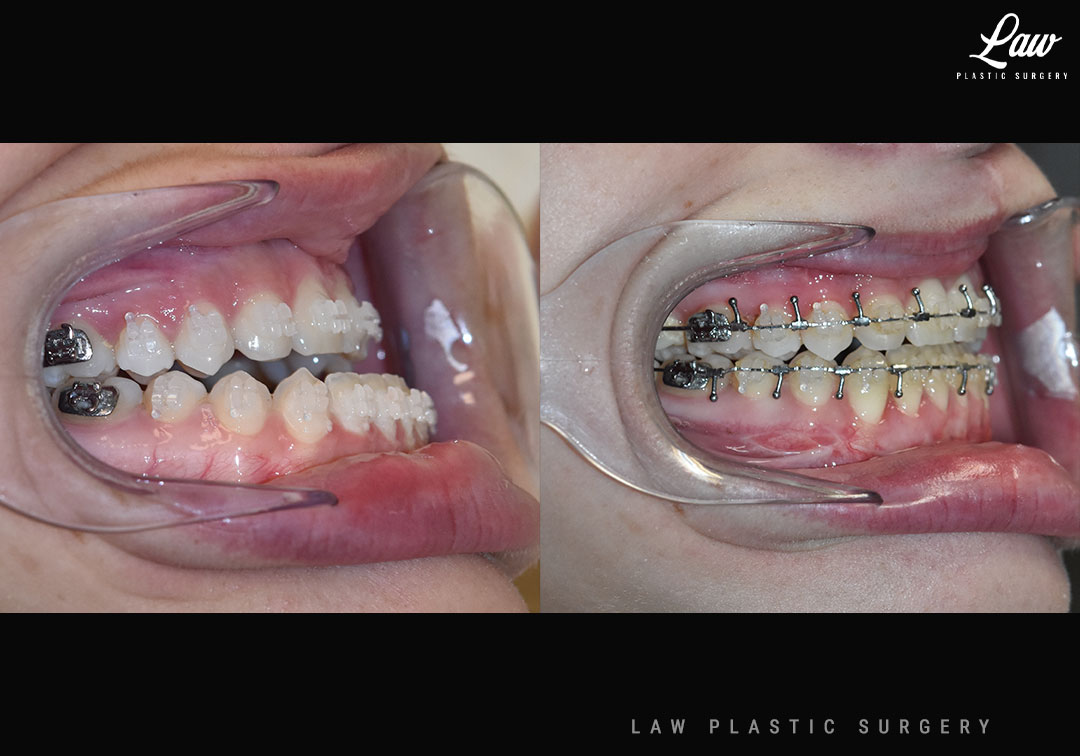
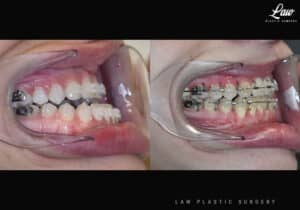
✅ Level, class I occlusion
✅ Bony foundation more symmetric
✅ Protect tooth roots and nerves
🚀 Confidence to the moon
We’re looking forward to his swelling coming down and braces coming off to better see his big smile! Stay tuned for updates!
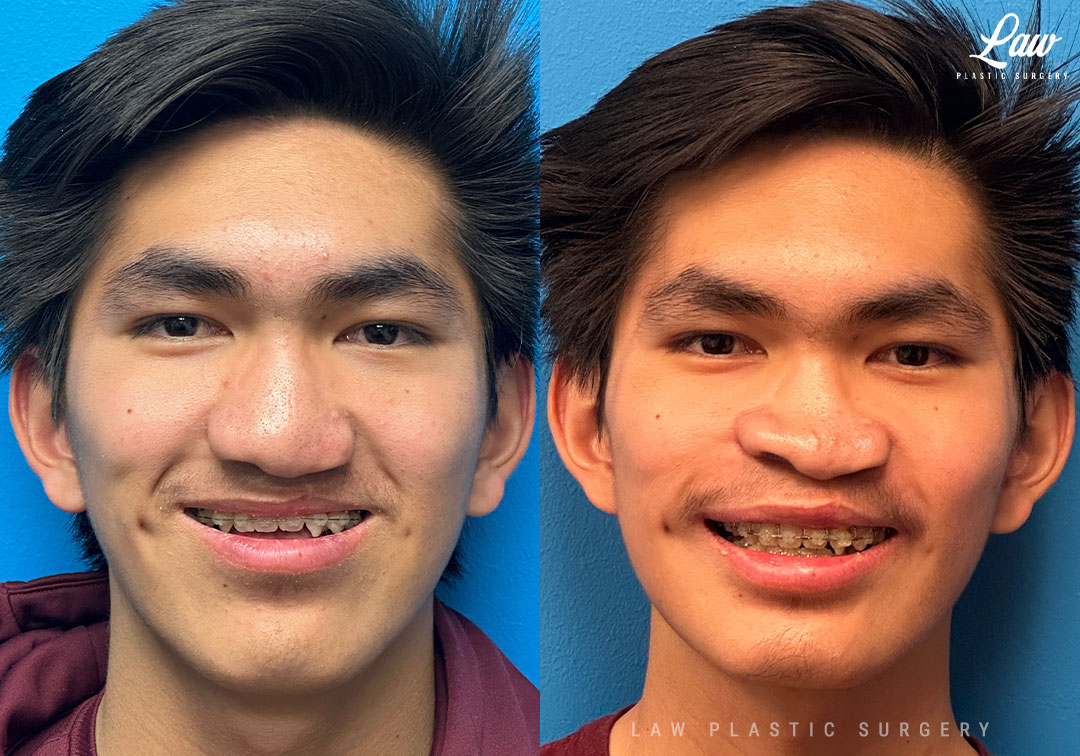
Jaw Surgery Before & After 3
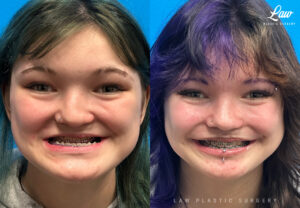
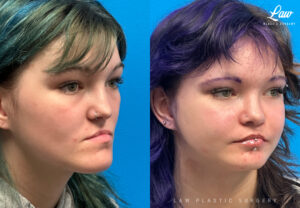
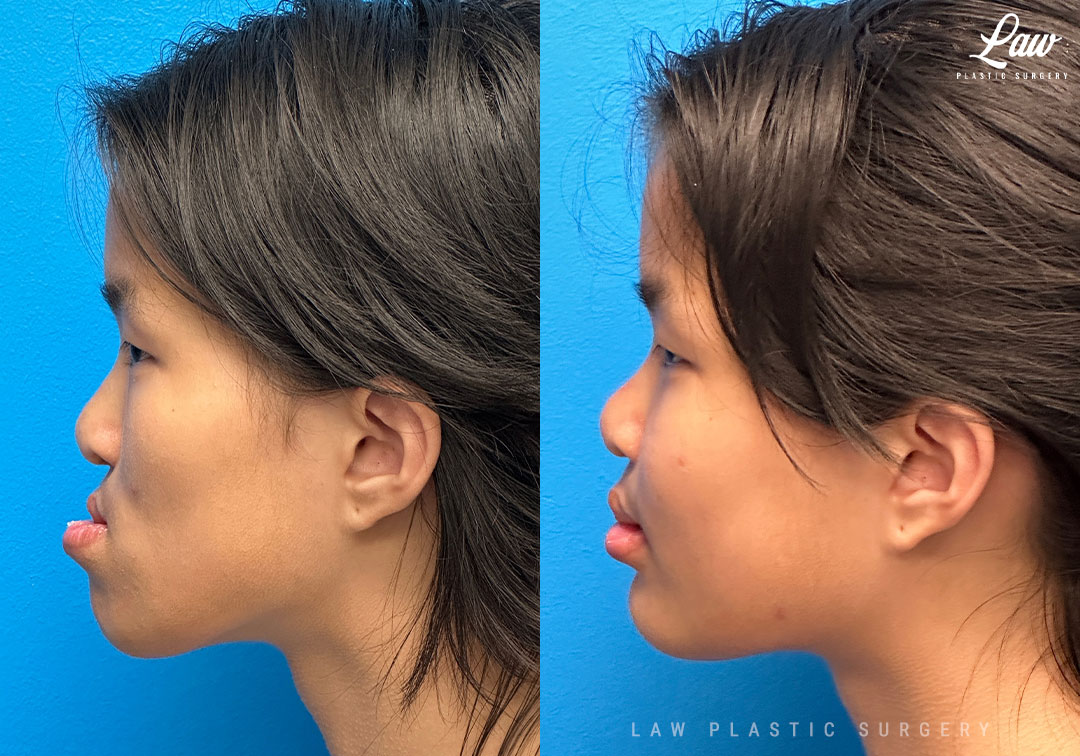
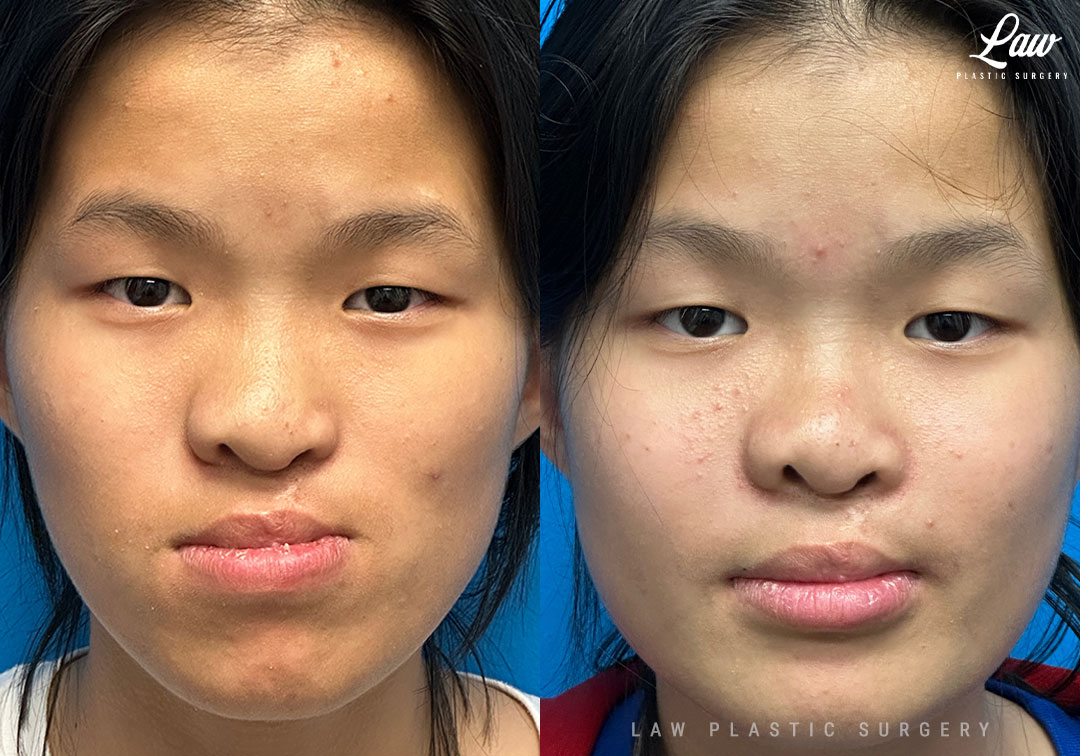
When your jaws do not line up well enough, no amount of speech therapy nor braces can fully address essential functions like:
– chewing food completely,
– speaking clearly, and
– smiling and socializing confidently.
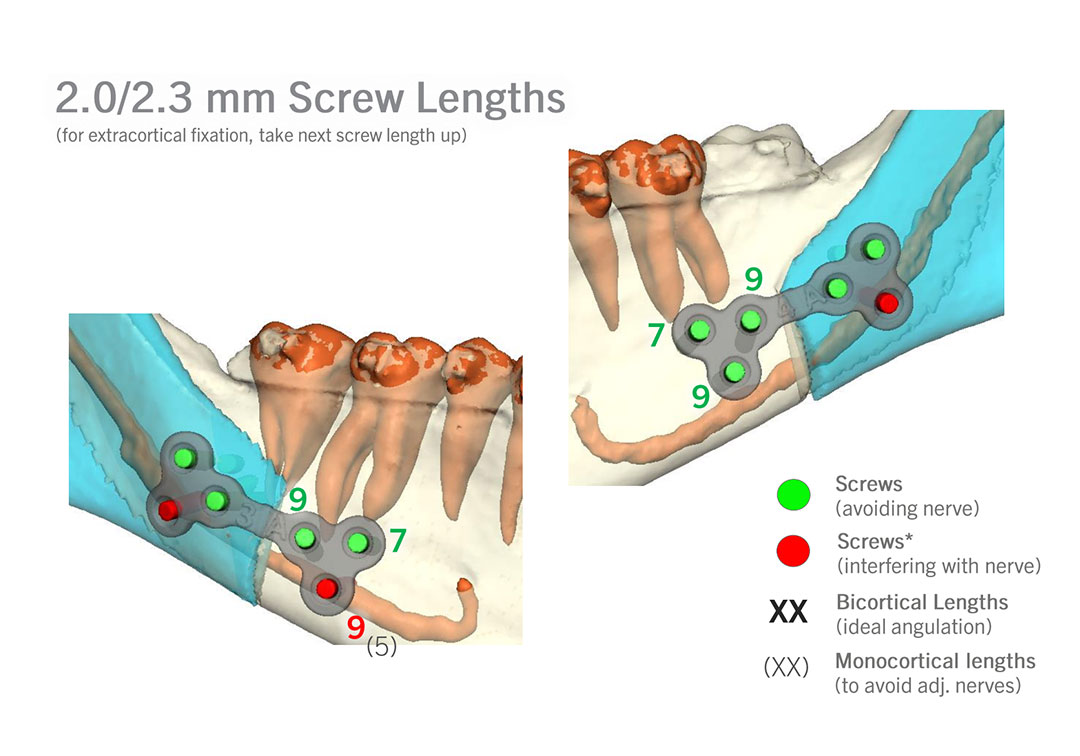
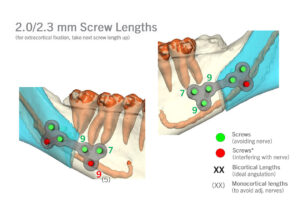
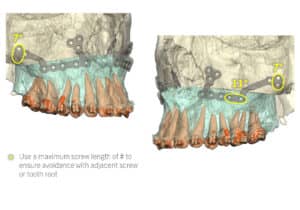
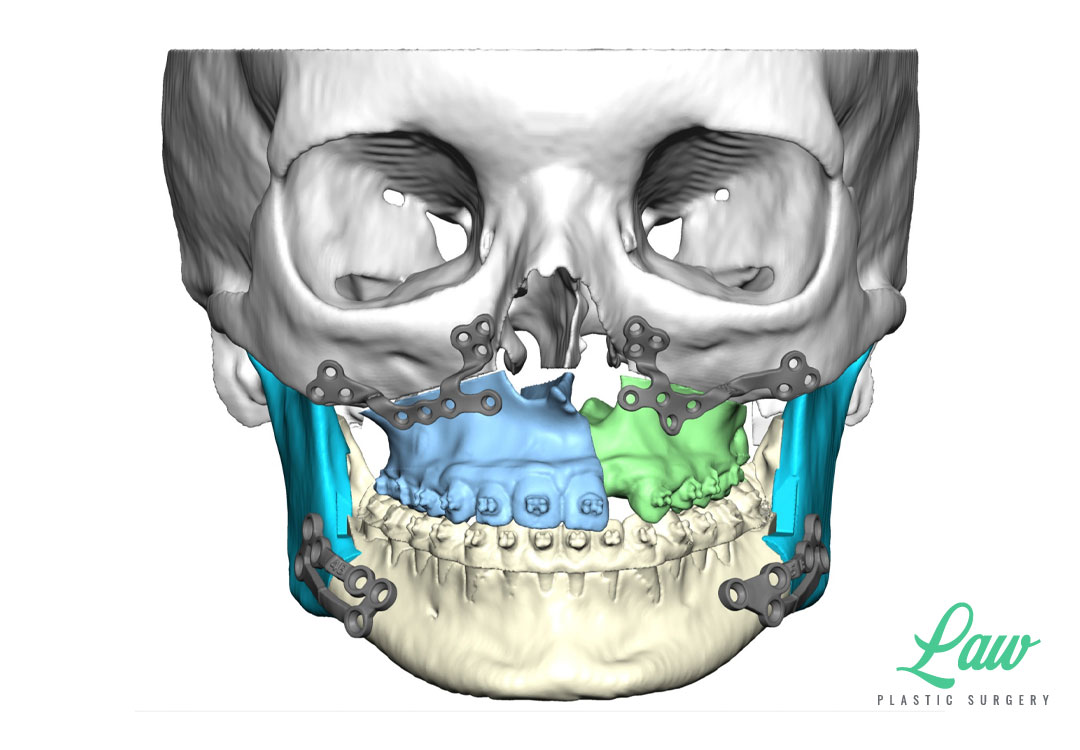
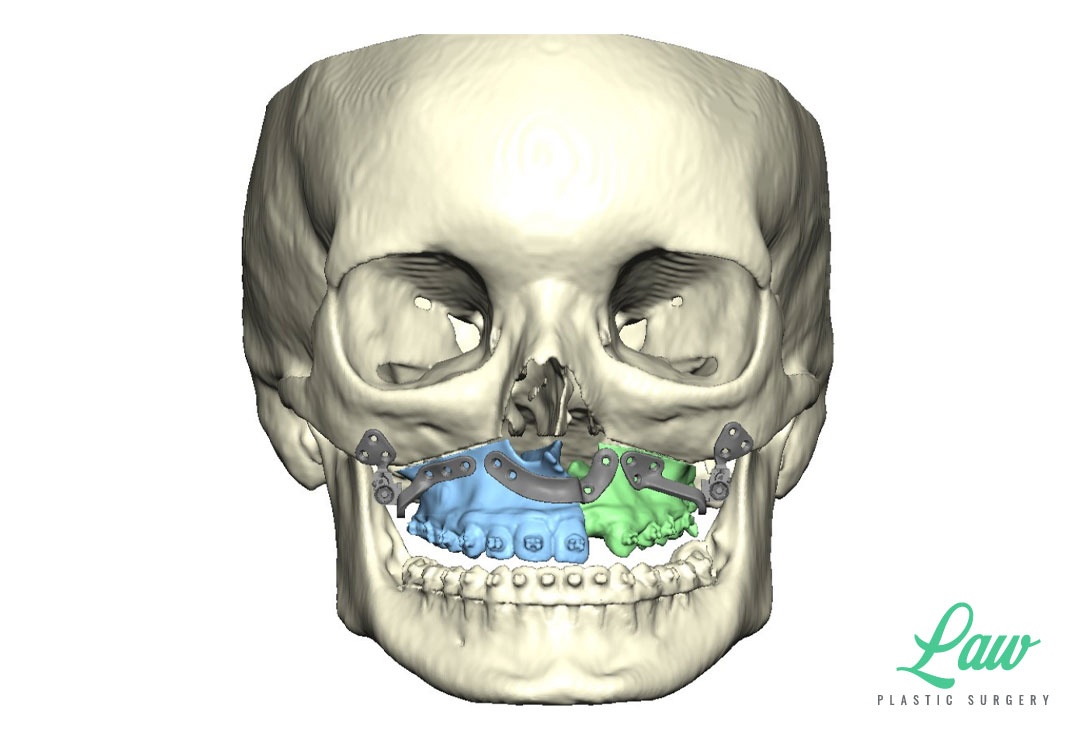
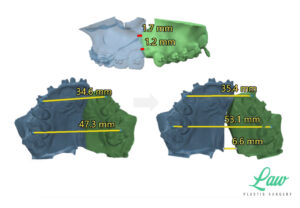
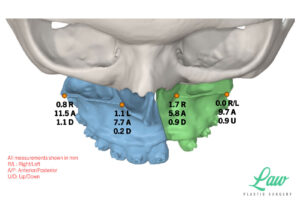
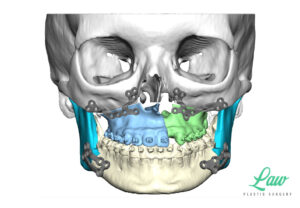
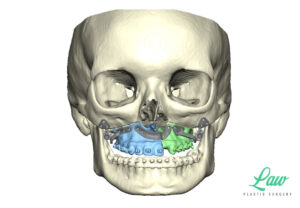
I’ve included a sneak peek behind some of the 3D planning we do to minimize the risks of :
– relapse (leading to more surgery),
– hardware complications (needing removal or revision), and
– damage to tooth roots or nerves (causing permanent numbness or loss of dentition).
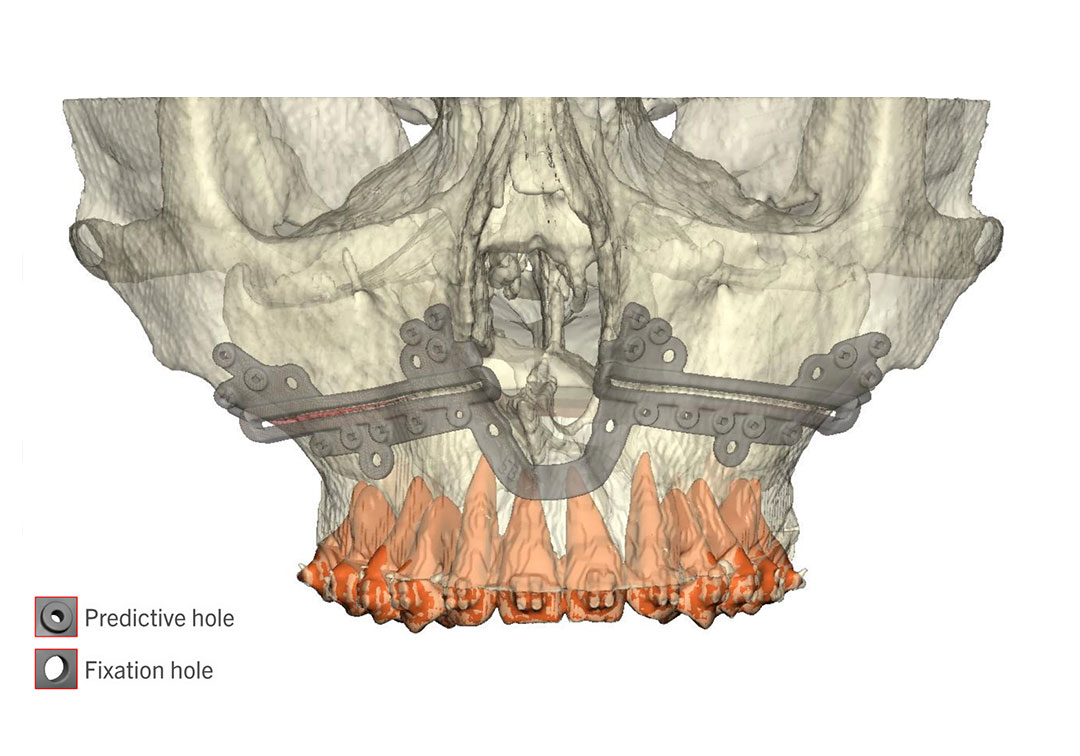
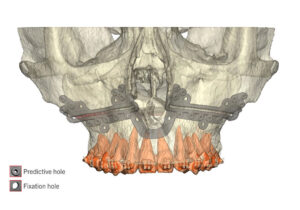
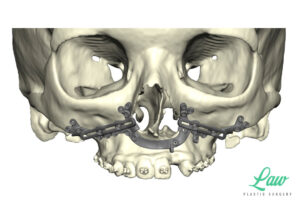
My current preference is a single plate on the right and left sides of the maxilla with single piece LeFort I advancements.
A multi-piece LeFort I is sometimes better off with a single, four-buttress plate, for more stable fixation!
Orthodontics: @GenecovOrthodontics
Surgeon: Huay-Zong Law, MD
Hardware: @KLSMartinGroup
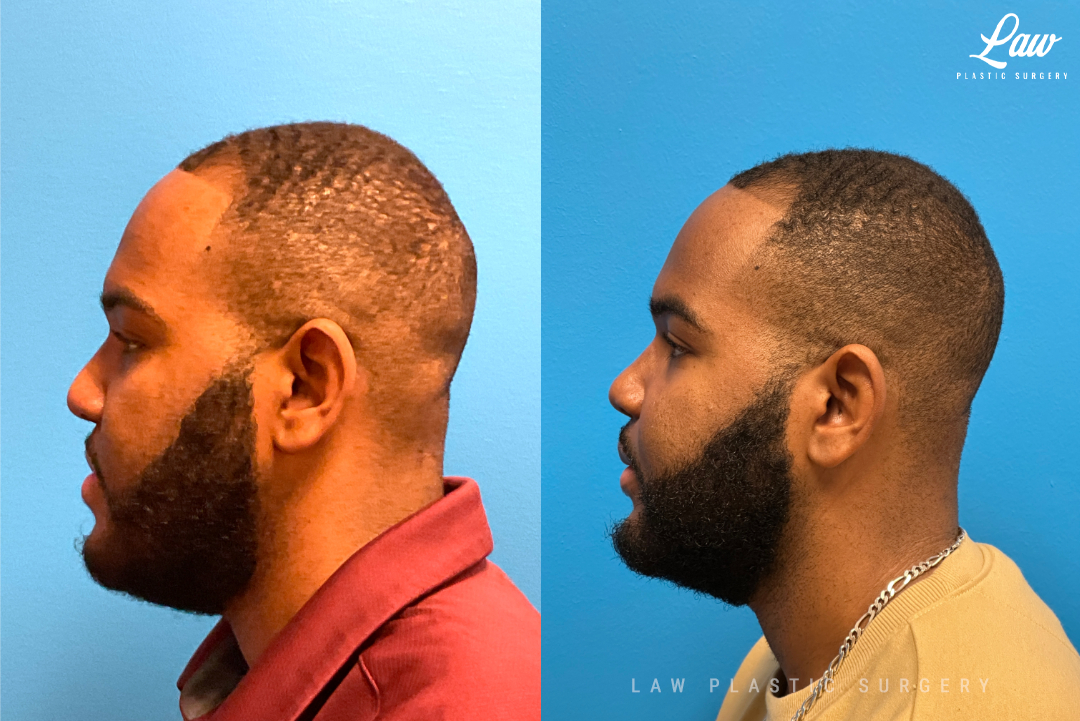
Jaw Surgery Before & After 4
About 1 in 3 patients with cleft lip and palate benefit from jaw surgery. Aligning the upper and lower teeth helps people fully chew their food, and reduces wear and tear on the TMJ’s.
We also consider facial balance and harmony when planning the surgery and final outcome.
Jaw surgery can often be done in a single surgery, sometimes involving just the upper jaw, and sometimes with the lower jaw as well.
Here, the amount of advancement was well over 10mm, which is the point at which we usually move towards distraction over a single surgery.
Distraction involves cutting the bone and freeing up scar tissue, but then gradually moving from the starting position by 1mm per day.
New bone is deposited in the space made as the upper jaw moves forward. The surrounding blood vessels, lining, and old scar tissue all expand and accommodate the new bony position.
We usually keep the hardware in place (much more comfortably after finishing advancement!) for 3 months while the new bone hardens.
At that point, minor adjustments can be made as needed with additional movement or augmentation, or just removal of the hardware.
Here, we performed some fat grafting to the upper lip, expecting about half of the fat to reabsorb and half to stay long term.
He is seen here at about a month after that surgery — we look forward to sharing more photos as all the swelling comes down!
Jaw Surgery Before & After 5
Whether because of complexity — or because of insurance purposes — this perpetually-positive patient was frustratingly turned away on the day of surgery with another team.
As anybody gearing up for jaw surgery will tell you, it is a long road to even get to that point.
Traditionally, the textbooks would recommend performing this operation in 2 stages: first, with a distraction, and then second, with a final positioning and mandible surgery.
Here, our engineers were able to plan for both a 1-stage and 2-stage reconstruction.
Using the custom guides and plates, we were able to match custom distractor footplates to the exact same fixation points as for the single-stage, custom plates.
This way, if the maxilla were unable to get to the final position (because the blood flow is under too much tension, or the scar tissue is too tight), then we could set the maxilla back to its starting point and begin the distraction process.
Once we had the maxilla set in either position, then we could decide on doing the lower jaw at that same time, or in the future if the maxilla required distraction.
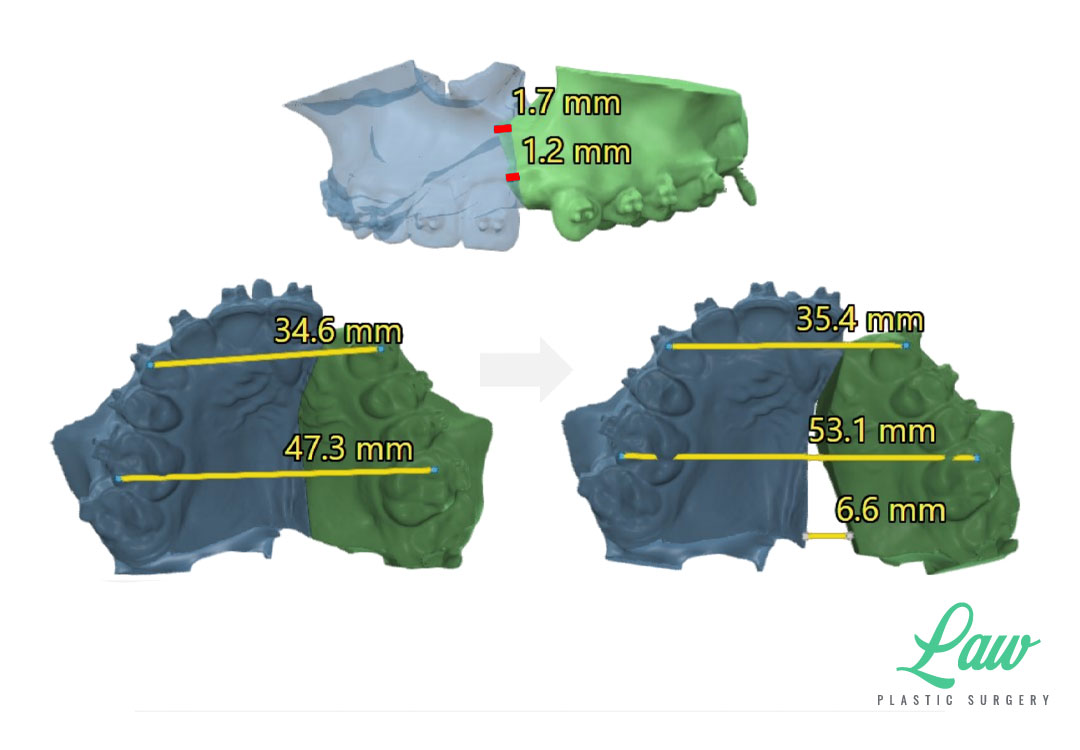
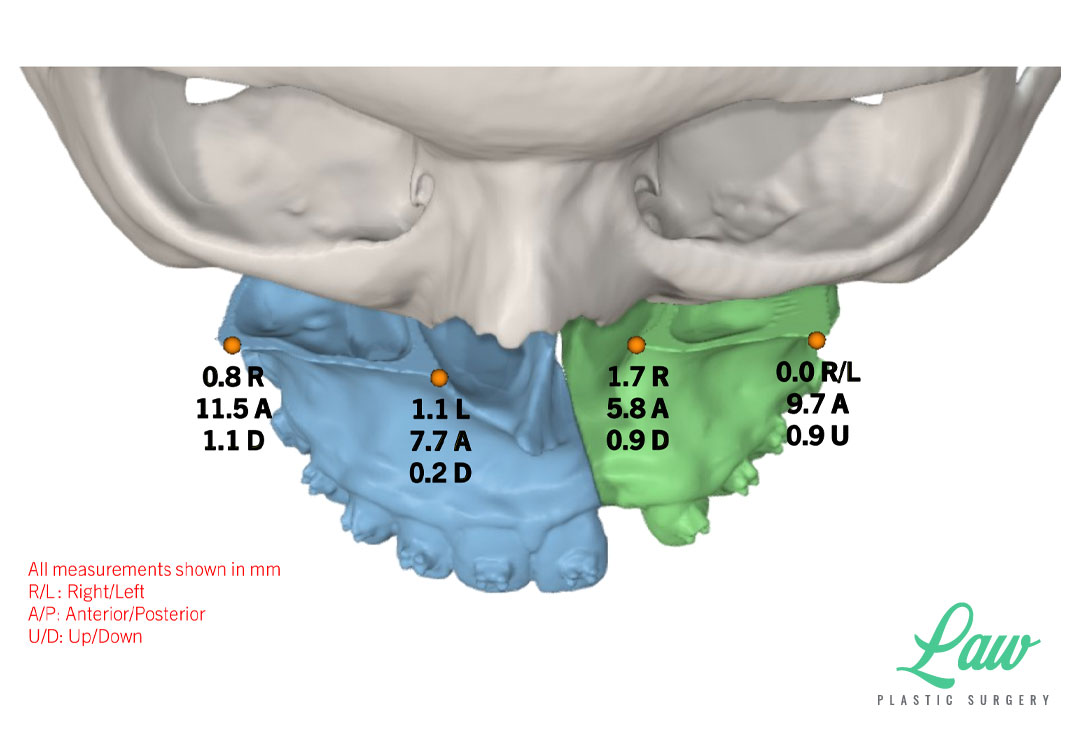
For the surgeons, we widened the maxilla by 6.6mm at the molars, and advanced the canines 12mm, with a 4mm lower jaw setback. The palatal split required an additional h-shaped osteotomy extension along both nasal floors, connected near the incisive foramen, to expand the palate.
She is seen here at 3 months post op, healing up well!
Jaw Surgery Before & After 6
“It’s crazy different…. For the longest time I wasn’t ever able to chomp my teeth because of my open bite, but now I can 😁”
“At first it was really horrible… But once I got back into school, it progressively kept getting better… With anything with surgery, it won’t be easy; it’s all about time.”
“I feel a lot better, I look better, and I am happy. It was worth it.”
Jaw Surgery Before & After 7
While it takes part of a lunchtime and several emails back and forth with our engineers, the end result is worth it.
With virtual surgical planning (VSP) for jaw surgery, we see the advantages of better precision (sub-millimeter compared to stock plates that transitioned by 2-mm with each level), more stability, and more foresight into any potential interferences or problems in the operating room.
This means less time in the operating room, quicker recovery, less relapse and reoperations, and a faster time to finish orthodontic treatment.
He is seen here at 6 months after upper and lower jaw surgery.
Orthodontics: @GenecovOrthodontics
Engineers: @KLSMartinGroup
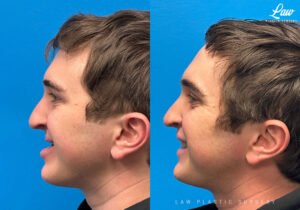
Jaw Surgery Before & After 8
It can be a tough surgery and tougher recovery, but the benefits to breathing, chewing, and facial balance can be tremendous.
This man worked through the worst of it – the months of prep work, swelling, drainage, difficulty sleeping, and more – with superb care and composure.
In this case, additional bone grafting to the upper cheeks helped improve lower eyelid support and balance, and augmented the bony healing and stability after the osteotomy.
We look forward to watch him continue on to greater things!
Jaw Surgery Before & After 9
This is especially true with our patients with clefts due to the scar tissue and abnormal blood flow who are at risk of an incomplete advancement or significant relapse.
We are able to use “internal” distractors in most cases, which leaves the distractor hidden inside the upper lip, rather than requiring an “external” HALO device.
The HALO is useful in some cases, but with the HALO overall we have historically seen a slightly higher rate of minor and major complications with infections, hardware failure, or wound problems.
Working with Dr. Fearon on complex craniofacial cases like Lefort 3 advancement, and some of his lessons learned, we have come back to using more HALO external distraction as well.
Jaw Surgery Before & After 10
Not always!
While we usually plan for the rhinoplasty to come second — to set the bony foundation first — sometimes the amount of nasal obstruction is severe enough to warrant doing the nose and nasal airway first.
This timing helps to alleviate the symptoms of nasal obstruction if severe, until the orthodontic set up is ready for jaw surgery.
Doing the nose first also helps the jaw surgery recovery, as most of the breathing is through the nasal passages. If the jaws are rubber banded snugly together, and the nose is blocked off, you can imagine that getting enough oxygen and carbon dioxide exchanged becomes more challenging.
We can do some of this work (like a septal resection, and turbinate work) during the upper jaw surgery, but may cause more swelling, bleeding, and problems healing if extensive work needs to be done.
She is seen 6 weeks after upper and lower jaw surgery, and 1 year after cleft rhinoplasty.
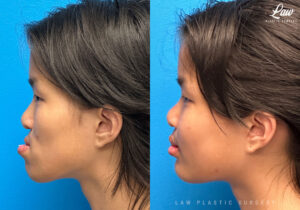
Jaw Surgery Before & After 11
The upper jaw often does not grow as much as the lower jaw, or may grow canted, in our patients born with a cleft.
Not every patient with a cleft will need this surgery, but it is one we perform routinely given the number of cleft and non-cleft craniofacial patients we see.
We usually wait until patients are fully skeletally mature before doing this surgery, to minimize the risk of needing to do any future surgeries.
Occasionally, the difference in the upper and lower jaw is so severe that we do perform distraction surgery prior to full maturity, knowing that we may need another surgery in the future.
He is seen here at 6 weeks after his operation, with his splint out and smile ready to show off!
Jaw Surgery Before & After 12
His upper jaw was leveled, centered, and rotated to be as symmetric as possible, with an advancement of 8-10mm, depending on your landmark.
His lower jaw also came forward to give him a functional and aesthetic occlusion, with a more functional airway as well.
Regarding the airway, we also come across patients with prior pharyngeal flaps who benefit from disconnecting these, with no apparent problems with speech.
The journey can be difficult with some chutes mixed in with the ladders. Especially for patients with previous surgeries or other craniofacial conditions, it is helpful to work with experienced teams like our orthodontist Dr. Jeff Genecov and engineers at Synthes.
Orthodontics: @GenecovOrthodontics
Custom Hardware and Planning: @JJMT_CMF
Jaw Surgery Before & After 13
The planning helps us identify any potential problems or anatomic considerations before the day of surgery, minimizing the risks of nerve or tooth injury. The guides and custom plates also provide 3D verification that the movement and final position agree with the occlusion-based, traditional technique.
The custom hardware is more precise and stronger, avoiding damage to teeth, nerves, and with titanium that can be as strong as traditional plates, but with a lower profile. The genioplasty also has a more precise result with custom planning.
This is particularly helpful for our patients with significant asymmetry, like people with hemifacial microsomia.
Finally, putting time in on the planning side ahead of time, helps reduce the time under anesthesia, so recovery is faster and easier.
Jaw Surgery Before & After 14
This handsome young man has a history of a unilateral cleft lip and palate.
He is seen here 7 months after jaw surgery (maxillary advancement, mandibular setback, and chin advancement), and 1 month after rhinoplasty.
His occlusion (or how his teeth fit together) is now centered and leveled, with the teeth now able to chew optimally. This will help with TMJ and dental health long-term.
The bony work also helped to balance his facial profile, giving his upper lip and chin more support.
The rhinoplasty improved his breathing by straightening the septum and supporting his nasal passages, like having a Breathe-Right strip on the inside of his nose.
His lip scar will also continue to improve after a re-repair and re-orientation of the muscle of his lip.
Jaw Surgery Before & After 15
⠀⠀⠀⠀⠀⠀⠀⠀⠀
Some children are born with a slightly smaller lower jaw or ear. Other children may have severe asymmetry affecting multiple areas including the eye, ear, cheek, upper and lower jaw, and nerve function. Other organ systems may also be affected, including the heart, kidneys, spine, and arms/hands, and need to be evaluated as well.
⠀⠀⠀⠀⠀⠀⠀⠀⠀
As each and every child is unique, their treatment plan must also be tailored to their needs. The goals are always to offer the best chance at a happy and healthy life, while minimizing the number of surgeries and the risks involved.
⠀⠀⠀⠀⠀⠀⠀⠀⠀
For this gentleman, the occlusion of his teeth was severely slanted, with TMJ pain and popping.
⠀⠀⠀⠀⠀⠀⠀⠀⠀
To correct this, we performed upper and lower jaw surgery with TMJ replacement at the same time. We waited to do this until he reached skeletal maturity and had a long enough break from contact sports to heal.
⠀⠀⠀⠀⠀⠀⠀⠀⠀
After the first few months of recovery, his jaw is free of popping and pain, and his symmetry is improved. Further procedures like fat grafting may be offered to further fine tune any asymmetry if desired.
⠀⠀⠀⠀⠀⠀⠀⠀⠀
As you can see, we love our patients, especially ones we have cared for since they were little!
Jaw Surgery Before & After 16
Braces alone sometimes aren’t enough to get a smile just right.
If the upper and lower dental arches are too far apart, or the facial harmony would be improved, orthognathic surgery may be recommended.
The main goals are often to align the upper and lower teeth, to help with chewing food completely and safely, and to improve facial balance from the upper, middle, and lower face.
Here, mandible-only surgery with a bilateral sagittal split osteotomy was done to correct a class II malocclusion.
Jaw Surgery Before & After 17
The smile says it all! Jaw surgery is used in cases where the upper and lower jaws are too misaligned to correct with braces alone.
Functional issues include difficulty with fully chewing and then choking on food, affected speech, and sleep apnea.
Long term, there may be problems with the TMJ, and supraeruption or loss of teeth and bone thickness. Obstructed breathing can cause a wide range of negative health effects, increasing the risk of obesity, diabetes, stroke, heart attacks, and more.
Thankfully we have worked for decades to get the surgery included under insurance (when meeting insurance criteria), with some of our most reliable partners right now Aetna and United Healthcare.
The recovery is significant, but so are the benefits!
Jaw Surgery Before & After 18
In other cases, the actual roots of the teeth need to be moved with jaw surgery, to reposition the entire foundation. The teeth work more effectively and efficiently after correction. This takes stress off of the TMJ and muscles used for chewing.
In some cases, we do this for sleep apnea, where the airway can be made larger by bringing the jaws and the attached soft tissue forward.
All surgeries carry risks like infection, permanent numbness, or damage to teeth, and the recovery for this surgery is more substantial than most.
A proper consultation and experienced team can help you make a well-informed decision about whether surgery would be right for you.
Jaw Surgery Before & After 19
I love helping someone get to the finish line, matching up their smile with their bright personality.
Upper and lower jaw surgery was done to bring the maxilla forward, and level the mandible, so that all of his teeth can be used while chewing.
This is at 6 weeks post-op, which is when we usually clear everyone for full activities.
In the recovery period, I recommend at least 1 week off from school/work, as the swelling can make it hard to breathe and feel rested.
The body is also working extra hard to heal itself, and calories and protein are harder to come by in liquid format for 99% of people.
That is also the point when our out-of-town patients usually head home if coming from a distance.
Jaw Surgery Before & After 20
This difference in bite causes problems with speech and chewing, and can increase the wear and tear on teeth and the TMJ’s.
Here, a custom-planned Lefort 1 advancement and chin advancement (genioplasty) corrected her malocclusion, while also giving a little bit more chin definition without going through the recovery and risks of a BSSO for the mandible.
Jaw Surgery Before & After 21
Commonly, the choice is made to advance the maxilla as far as the scar and soft tissue allows, usually 8-12mm, and then set the mandible back with a BSSO to get to Class I occlusion.
Setting back the mandible can sometimes cause issues with sleep apnea and with the appearance of premature aging.
Thus sometimes we do a two-stage reconstruction:
1) Lefort 1 distraction to advance the maxilla and let the soft tissue adapt for blood flow and long-term stability. Here, over 14mm advancement was achieved.
2) Removal of the distractors, replacement with a custom titanium plate, and closing/centering the occlusion with a BSSO.
He is seen here at 6 weeks. Swelling continues to recede greatly over the next several weeks, and then further gradually over 9-18 months.
Jaw Surgery Before & After 22
One piece of this syndrome is a history of cleft palate and midface hypoplasia that then leads to Class III malocclusion, aka an underbite.
Custom planning and hardware helped us line up his teeth for him to be able to chew food, to speak normally, and to show off his big smile after all the orthodontic work that often goes on for many years.
His swelling will continue to improve over the next 6-12 months. We look forward to those braces coming off and hopefully taking a break from doctors for a long while!
Jaw Surgery Before & After 23
As long as the nasal passages are functional enough to allow for recovery after the jaw surgery, we will do the jaw surgery first, and let the foundation settle before working on the nose.
The goals for the nose are very individualized for each person. Some patients focus mainly on the airway, without any concern for the outward appearance.
That said, giving the nasal framework stronger and more symmetric support can be an essential part of making breathing easier.
Making the lip more symmetric with better balance between the upper and lower lip can help with speech and confidence.
Filler (usually a hyaluronic acid) can be used for a temporary boost without surgery, while fat grafting gives more long-term results, but requires harvesting someone’s fat (usually with a little bit of liposuction).
Surgery may be recommended with – or instead of – filler, depending on each person’s goals and their anatomy, including the amount of scarring, and each component of the lip (skin, muscle, and mucosa).
Swelling and scar maturation can take months to fully return to normal. Like with any surgery, most people are perhaps 85-90% back to baseline at 6-12 weeks. With prior surgeries, and the extent of some of these surgeries, that timeline can run twice as long.
Jaw Surgery Before & After 24
Here, swelling is still present at 6 weeks, but especially in the oblique view, one can see his facial harmony improved with a chin advancement (genioplasty).
The Lefort 1 with bone grafting also helps provide midface support, and additional augmentation at the area of previous cleft bone grafting for long term stability and dental health.
Jaw Surgery Before & After 25
If the upper arch is too constricted/narrow, we can separate the maxilla into multiple, separately mobile sections.
This is useful for cleft patients, but that experience carries over for our noncleft patients as well.
Careful dissection and use of ultrasonic saws preserves the blood flow through the soft tissue between bone cuts.
Here we performed this preparation and planning with Invisalign, in coordination with Dr. @GenecovOrthodontics.
Jaw Surgery Before & After 26
If an oral splint is used, usually speech and swelling feel much better once that comes out.
Post-op diet after jaw surgery is one of the most common questions we field.
Normally this is a liquid diet for 2 weeks until incisions are better healed.
Then we switch to a soft, non-chew diet for another 6 weeks.
That includes mashes, smoothies, and milkshakes. We also allow for things like ground beef and steaks, as long as the chewing is completed outside of the mouth. One it goes in, you can savor the flavor, and then wash it down. But no chewing until the bone is further healed!
Jaw Surgery Before & After 27
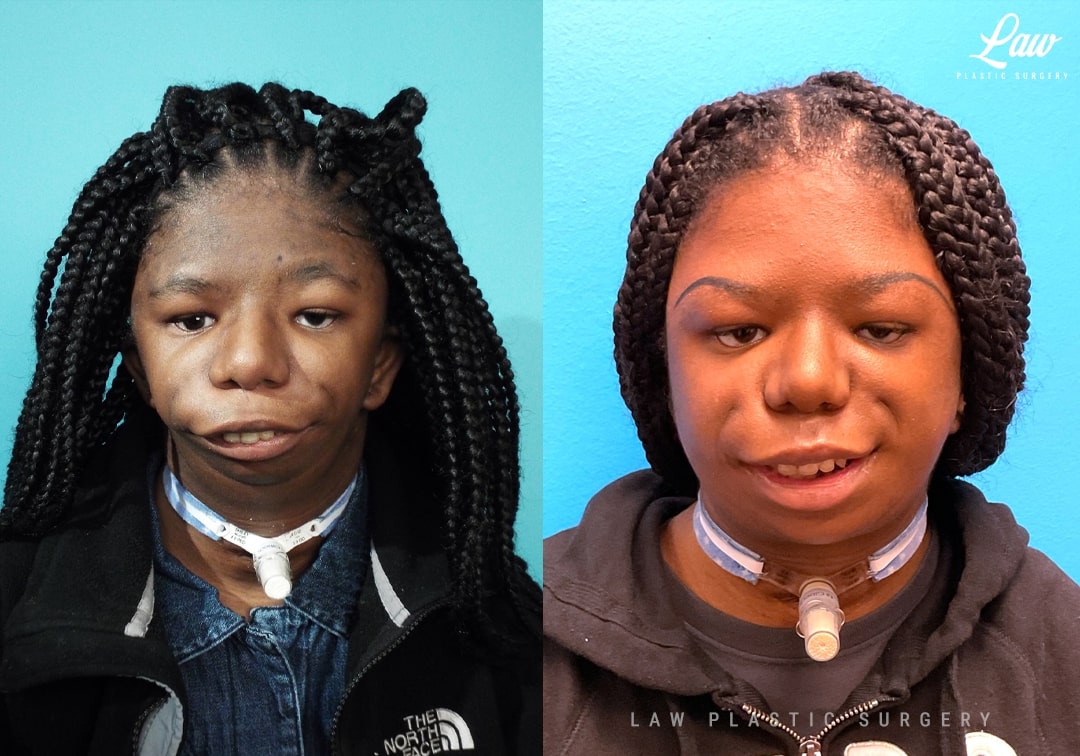
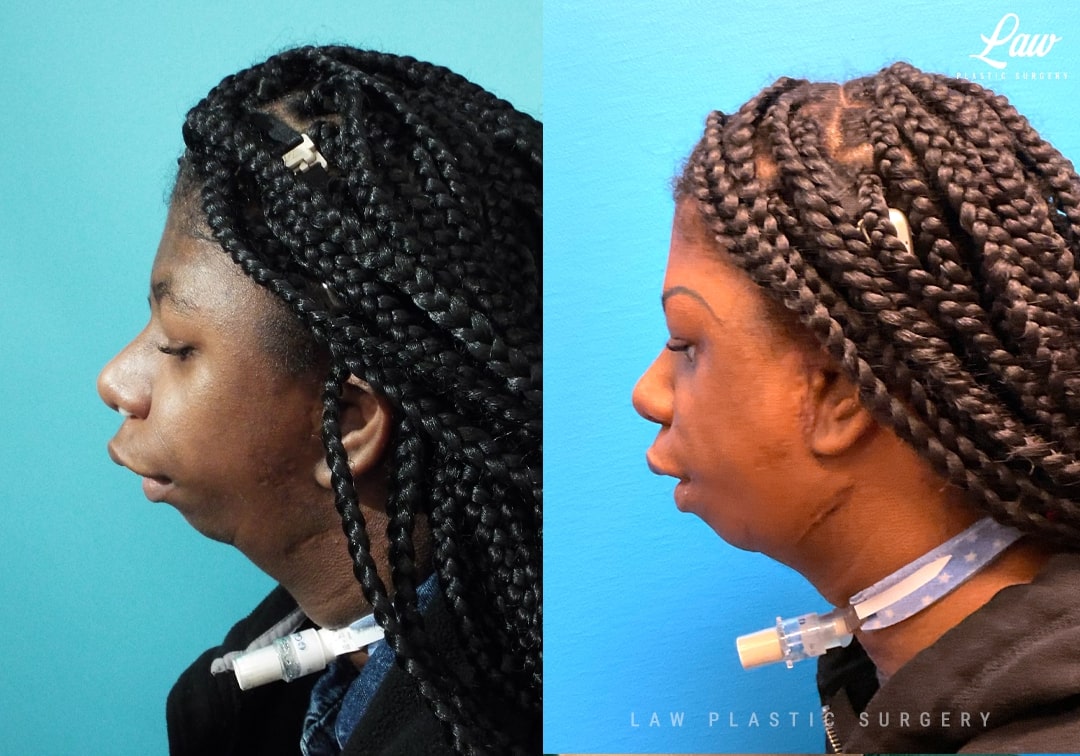
The small size of her mandible has required her to have a tracheostomy her entire life. She has had multiple jaw distractions, where the mandible has been broken and gradually lengthened.
The combination of her condition and her surgeries had left her with ankylosed, or totally frozen and immobile, TMJ’s on both sides.
We performed custom TMJ replacements – similar to a knee or hip replacement – with the condyles replaced with titanium heads, and a titanium and plastic joint fossa custom made to fit at the base of her skull.
She is seen here at 6 weeks after her surgery, with her range of motion the best it has ever been. She continues to improve every week as she progresses with her physical therapy.
She has been able and wanting to talk more, too, and we look forward to repairing her cleft palate (which has never been accessible). One day we may be able to remove her trach as well!
Jaw Surgery Before & After 28
Upper and lower jaw surgery (LeFort I advancement and bilateral sagittal split osteotomy) was performed to close and level his occlusion.
He is happily now back to full activities on his skates!
Jaw Surgery Before & After 29
Commonly we perform this surgery for our patients with a history of a cleft. Growth of the upper jaw may not keep up with the lower jaw. The teeth then do not line up, and normal chewing is affected.
We also perform this surgery for patients with sleep apnea, or other imbalances of the jaws including overbites, underbites, open bites, and cants (like with hemifacial microsomia).
Jaw Surgery Before & After 30
At some point, if the upper and lower roots are just too far apart, no amount of orthodontics will allow the teeth to line up.
That difference leads to problems chewing, breathing, and speaking. Some people also are more self-conscious of their smile.
Here, a four-piece Lefort 1 was performed, to correct a difference in the transverse dimension, in addition to the anterior-posterior direction.
He is seen here at 6 weeks, well on the road to recovery!