Jaw Distraction Before & After Photos
Jaw Distraction Before & After Case 1

Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
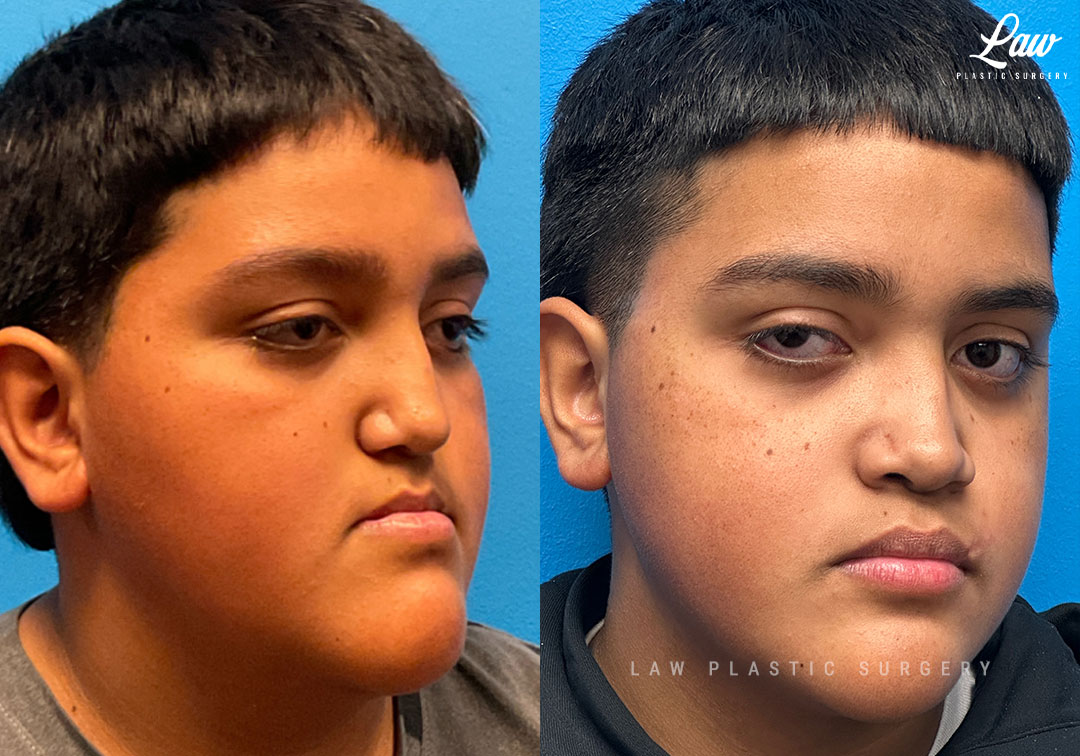
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
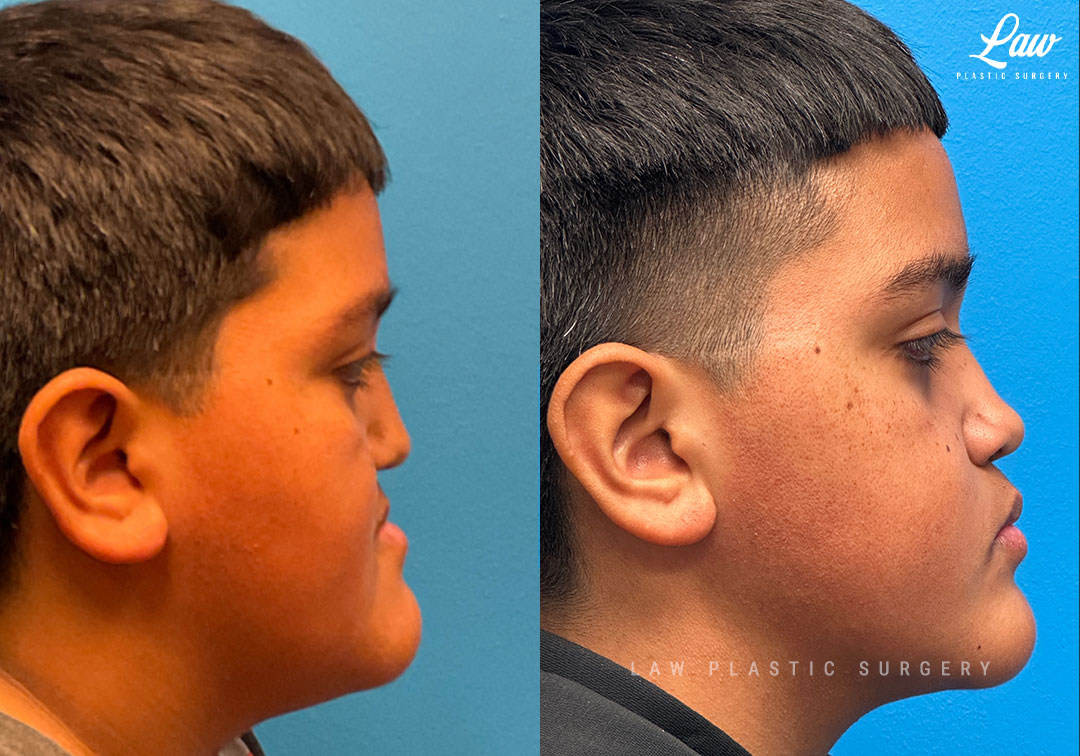
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Lefort 1 distraction is a powerful tool when the upper jaw (maxilla) sits more than about 8-10mm back from its ideal position relative to the lower jaw (mandible).
This is especially true with our patients with clefts due to the scar tissue and abnormal blood flow who are at risk of an incomplete advancement or significant relapse.
We are able to use “internal” distractors in most cases, which leaves the distractor hidden inside the upper lip, rather than requiring an “external” HALO device.
The HALO is useful in some cases, but with the HALO overall we have historically seen a slightly higher rate of minor and major complications with infections, hardware failure, or wound problems.
Working with Dr. Fearon on complex craniofacial cases like Lefort 3 advancement, and some of his lessons learned, we have come back to using more HALO external distraction as well.
Jaw Distraction Before & After Case 2
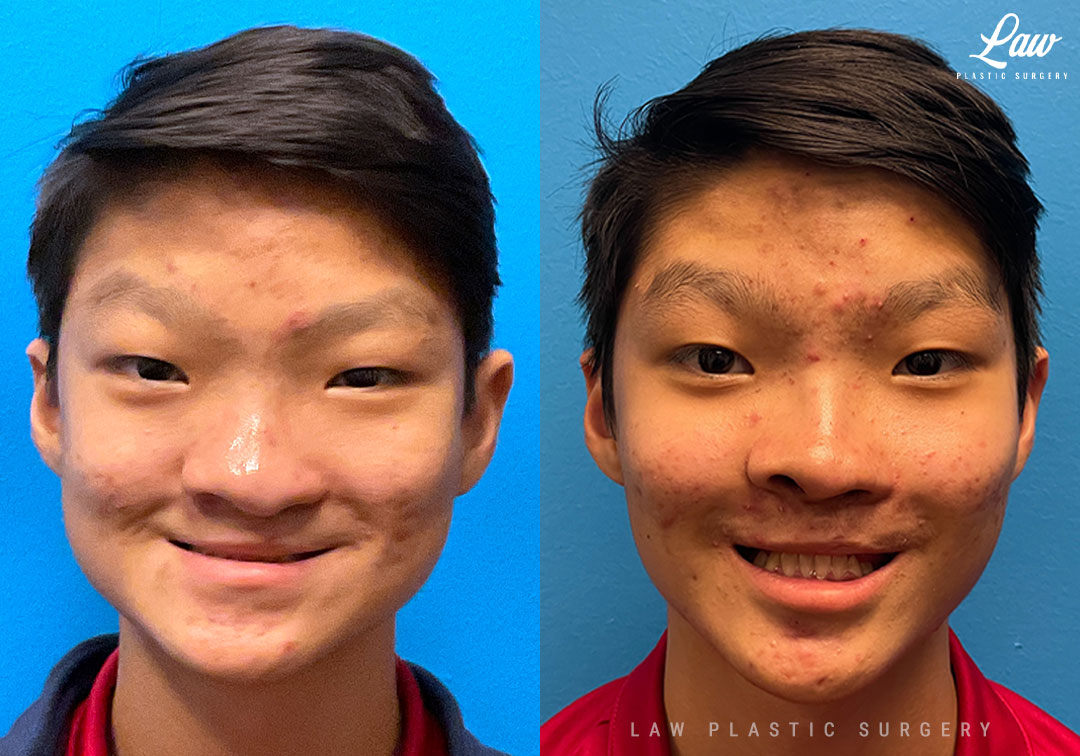
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
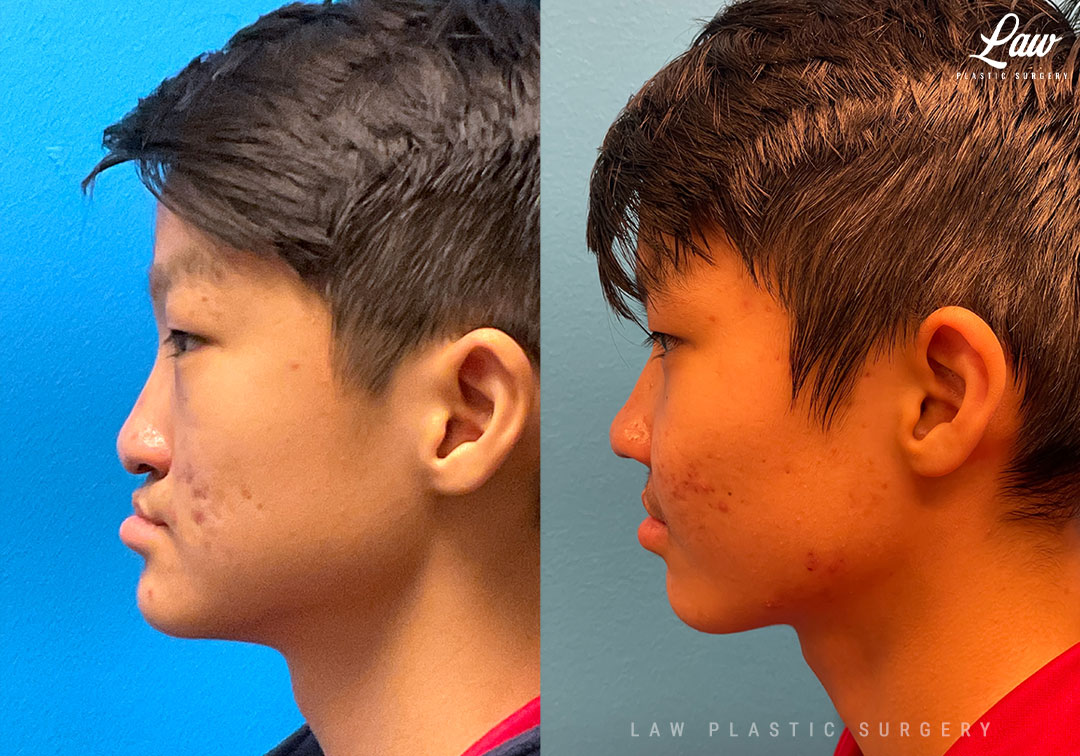
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
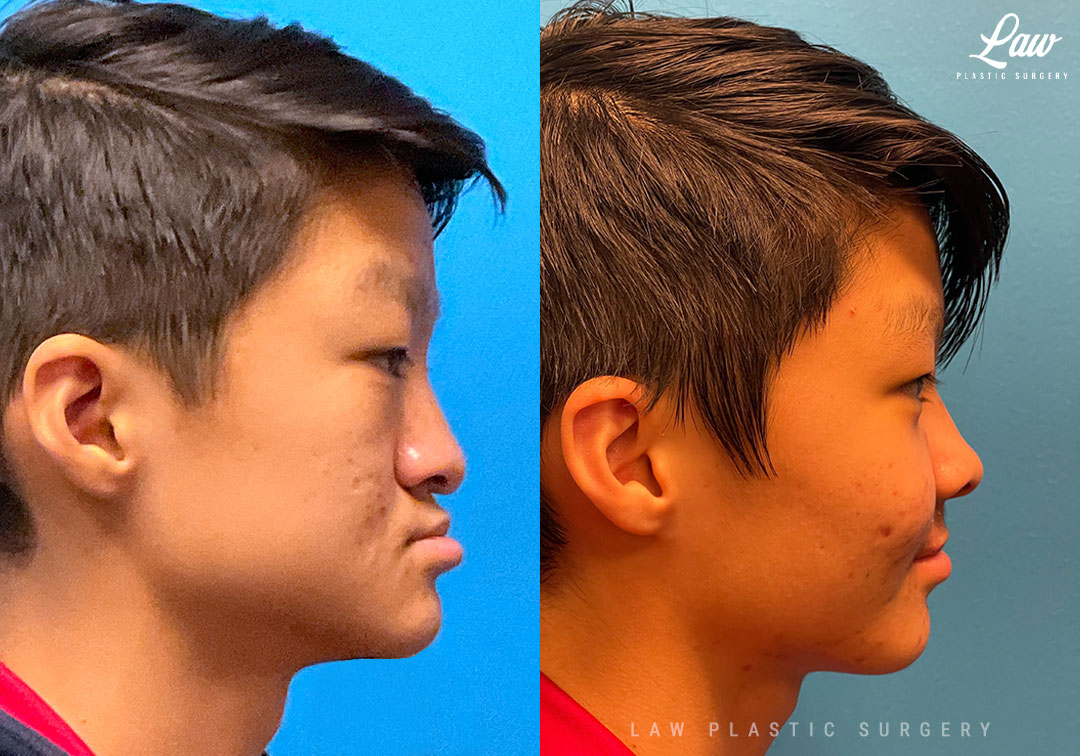
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
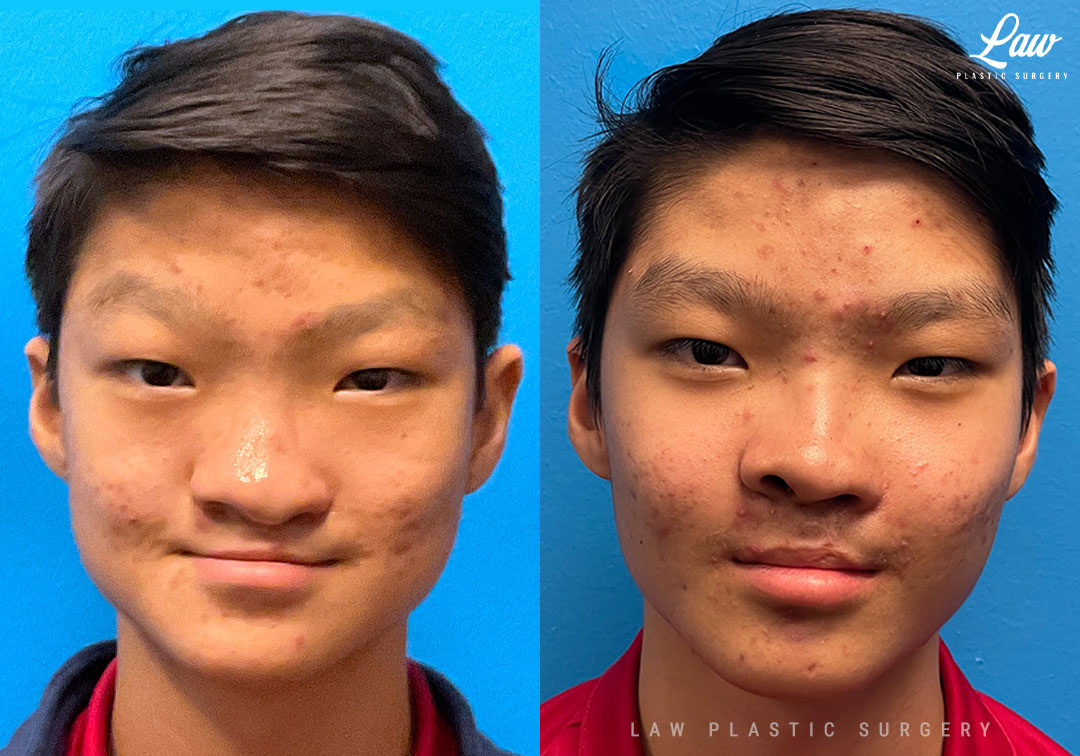
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
The timing and techniques used for our patients with clefts are tailored to each patient.
Here, the upper jaw required greater than 10mm of advancement to correct his occlusion.
Thus, we performed a Le Fort 1 internal distraction: the maxilla was mobilized, and hardware placed to gradually bring the bone and teeth forward 0.5mm at a time.
This incremental movement stretches the scar tissue, blood vessels, and nerves, giving them a chance to catch up a little bit every day and adapt. Otherwise, the advancement in a single surgery can be limited, and the maxilla is at risk of collapsing back.
Once the new bone solidifies, we return to retrieve the hardware and double-check stability of the new bone.
Here, he had continued difficulty breathing through his nose, and desired improved symmetry and contour.
Given his ongoing nasal obstruction — a closed septorhinoplasty was performed at the same time as the hardware removal.
MTF rib cartilage was used as a dorsal onlay graft, cantilevered with a septal extension graft. Tip grafts and diced cartilage helped provide some further tip definition and contour.
He is healing wonderfully at one month, with the swelling already much improved.
Jaw Distraction Before & After Case 3

Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
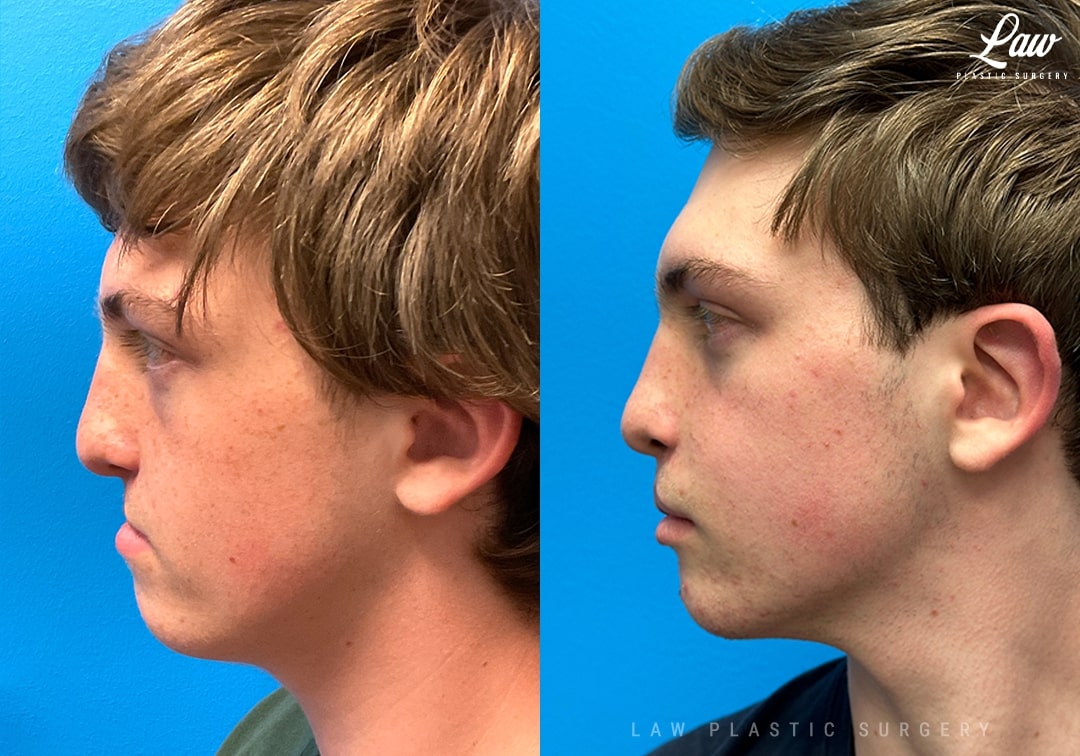
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
The smile says it all!About 1 in 3 patients with cleft lip and palate benefit from jaw surgery. Aligning the upper and lower teeth helps people fully chew their food, and reduces wear and tear on the TMJ’s.
We also consider facial balance and harmony when planning the surgery and final outcome.
Jaw surgery can often be done in a single surgery, sometimes involving just the upper jaw, and sometimes with the lower jaw as well.
Here, the amount of advancement was well over 10mm, which is the point at which we usually move towards distraction over a single surgery.
Distraction involves cutting the bone and freeing up scar tissue, but then gradually moving from the starting position by 1mm per day.
New bone is deposited in the space made as the upper jaw moves forward. The surrounding blood vessels, lining, and old scar tissue all expand and accommodate the new bony position.
We usually keep the hardware in place (much more comfortably after finishing advancement!) for 3 months while the new bone hardens.
At that point, minor adjustments can be made as needed with additional movement or augmentation, or just removal of the hardware.
Here, we performed some fat grafting to the upper lip, expecting about half of the fat to reabsorb and half to stay long term.
He is seen here at about a month after that surgery — we look forward to sharing more photos as all the swelling comes down!
Jaw Distraction Before & After Case 4
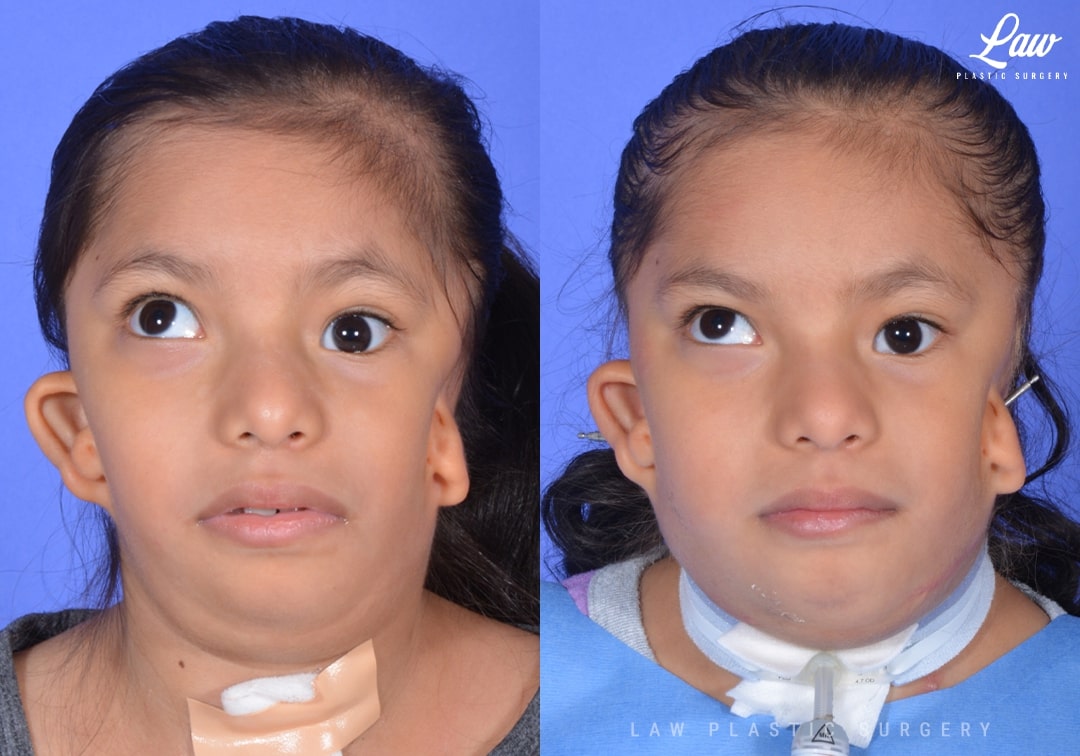
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
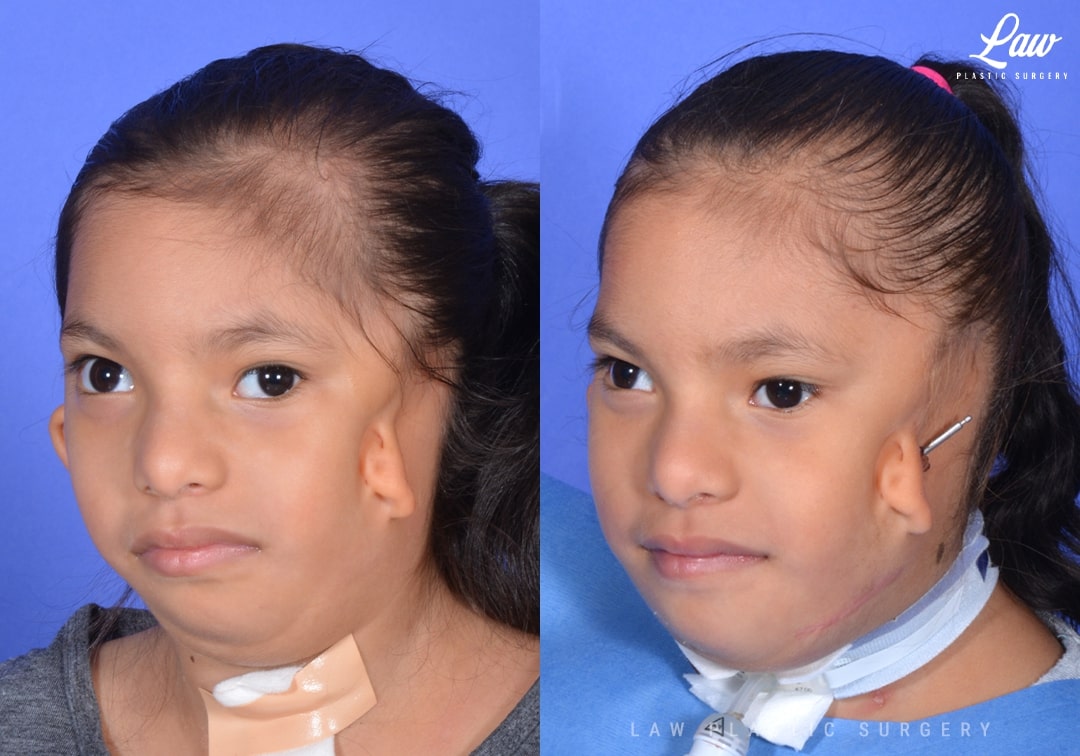
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
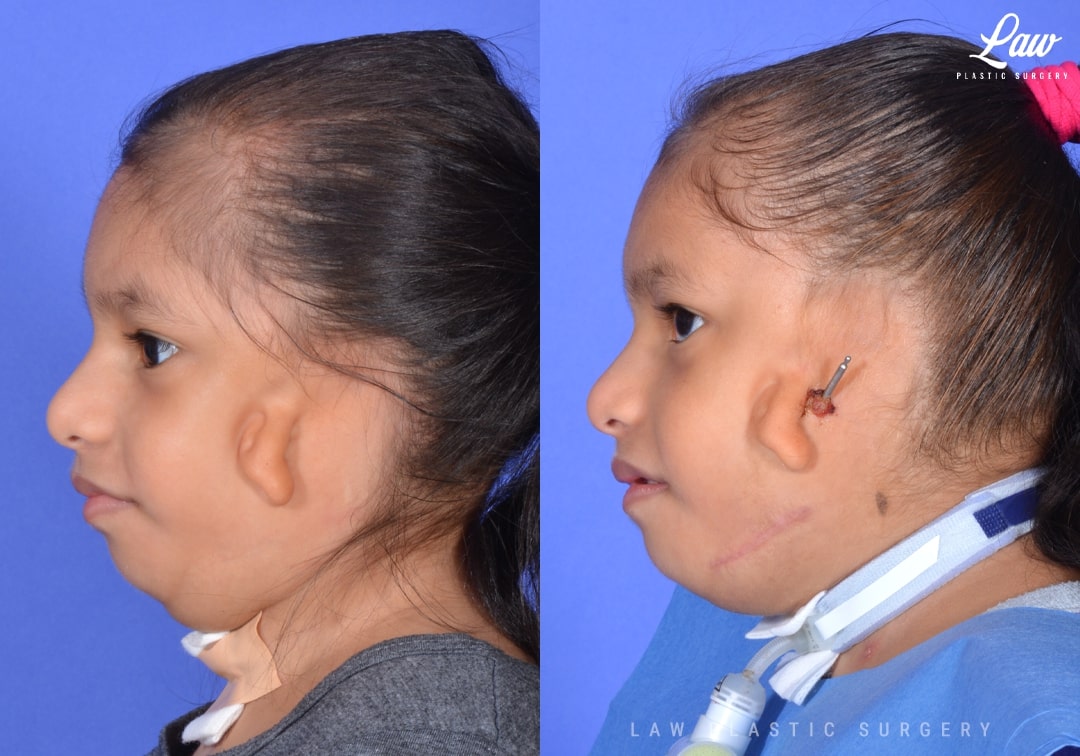
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Treacher-Collins syndrome affects about one in every 50,000 children, and varies widely in severity from one patient to another.
There is underdevelopment of the cheeks and jaws. This affects the shape and size of the orbits, cheeks, and jaws.
For this patient, the small lower jaw made her airway too small for her breathing needs. Her tracheostomy site was unable to heal because of this, despite a previous jaw distraction.
3D modeling and planning was performed to give the best chance at protecting her tooth buds and nerves, while having enough solid fixation to grow new bone, pushing her jaw forward in the process.
Over a couple of weeks, the mandible was moved out a millimeter at a time.
The hardware has since been removed, with good bone healing.
We look forward to having her tracheostomy removed and healed soon!
Jaw Distraction Before & After Case 5
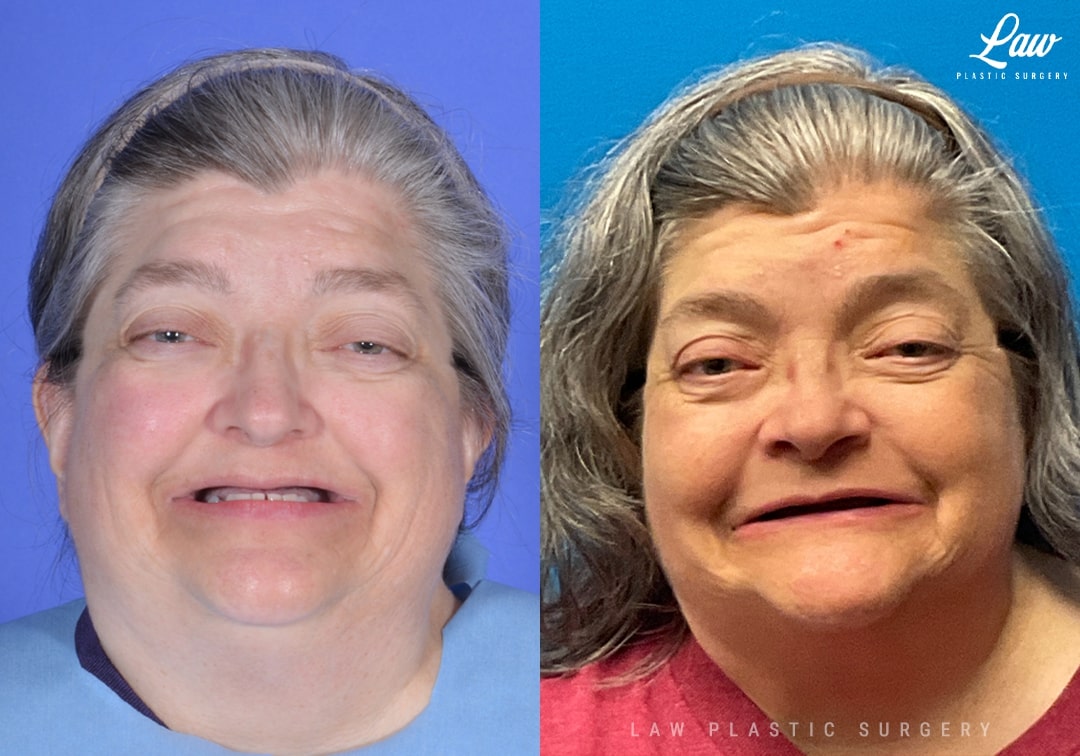
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
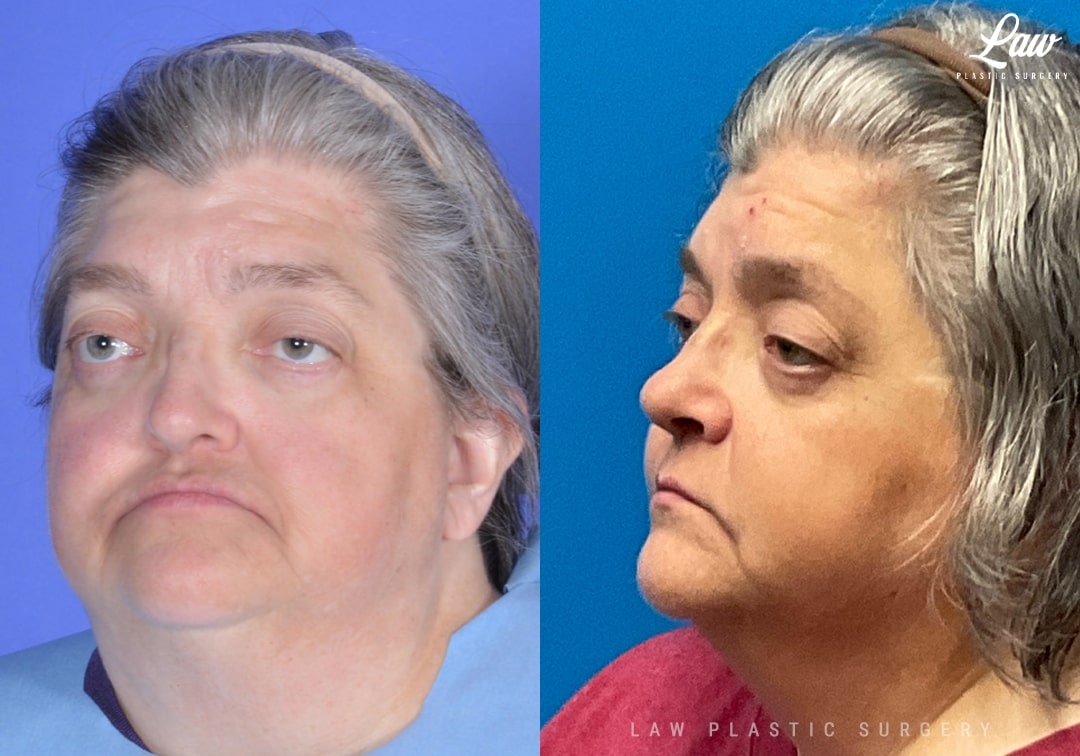
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
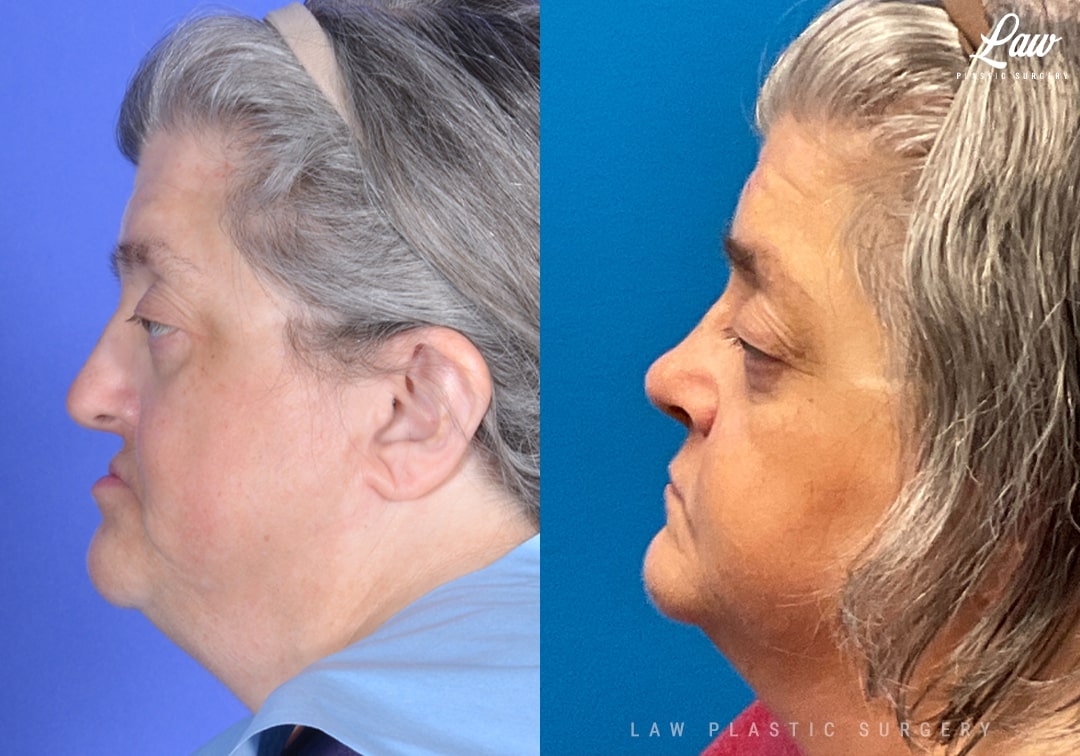
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Jaw distraction surgery is used when the amount of movement is too large for a single surgery.
In this case, a patient with Crouzon syndrome planned for dental restoration. The upper and lower jaws were much more than 10mm offset, which is the usual cutoff to consider distraction surgery.
A 3D-printed model and guides were used for precisely planning the placement of the osteotomies, plate positioning, and the vector of distraction.
The use of internal distractors avoided the use of a large, external halo device. No external scars, wires, or screws were needed.
After placement of the hardware, the upper jaw was advanced a little every day until we reached our goal of lining up the upper and lower jaws.
The patient is seen here after the bone has solidified, and the distractors have been removed.
You can see an improvement of her facial profile and balance, with the upper lip now better supported as well.
The posts for dental implants were able to be placed at the time of distractor removal as well.
We can’t wait to see her final results!
Jaw Distraction Before & After Case 6
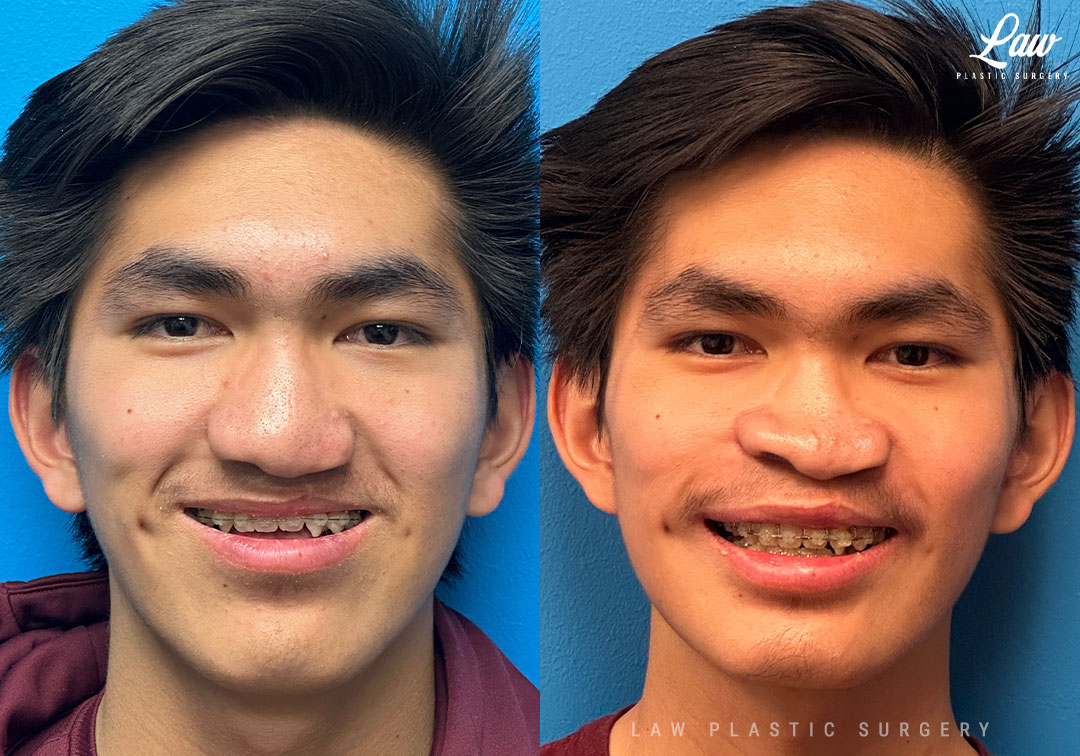
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
For Angle Class III malocclusion of over 10mm, we have a couple of options.
Commonly, the choice is made to advance the maxilla as far as the scar and soft tissue allows, usually 8-12mm, and then set the mandible back with a BSSO to get to Class I occlusion.
Setting back the mandible can sometimes cause issues with sleep apnea and with the appearance of premature aging.
Thus sometimes we do a two-stage reconstruction:
1) Lefort 1 distraction to advance the maxilla and let the soft tissue adapt for blood flow and long-term stability. Here, over 14mm advancement was achieved.
2) Removal of the distractors, replacement with a custom titanium plate, and closing/centering the occlusion with a BSSO.
He is seen here at 6 weeks. Swelling continues to recede greatly over the next several weeks, and then further gradually over 9-18 months.
Jaw Distraction Before & After Case 7

Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
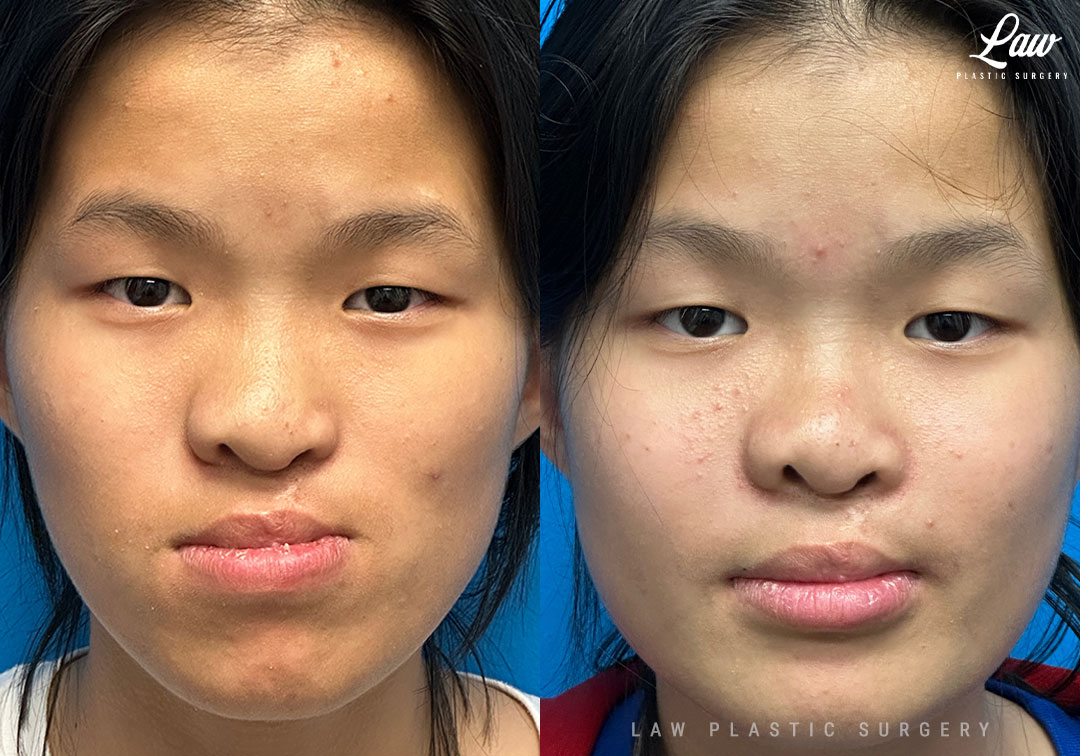
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
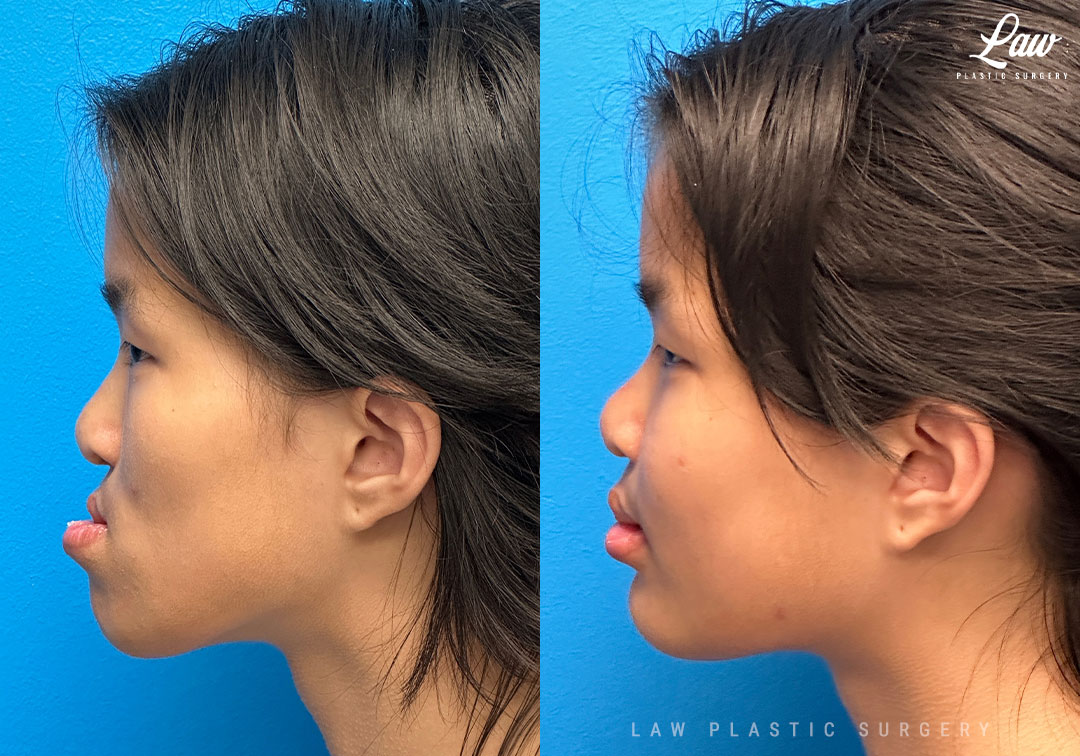
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Why we do jaw surgery, in sum:
“It’s crazy different…. For the longest time I wasn’t ever able to chomp my teeth because of my open bite, but now I can 😁”
“At first it was really horrible… But once I got back into school, it progressively kept getting better… With anything with surgery, it won’t be easy; it’s all about time.”
“I feel a lot better, I look better, and I am happy. It was worth it.”
Jaw Distraction Before & After Case 8
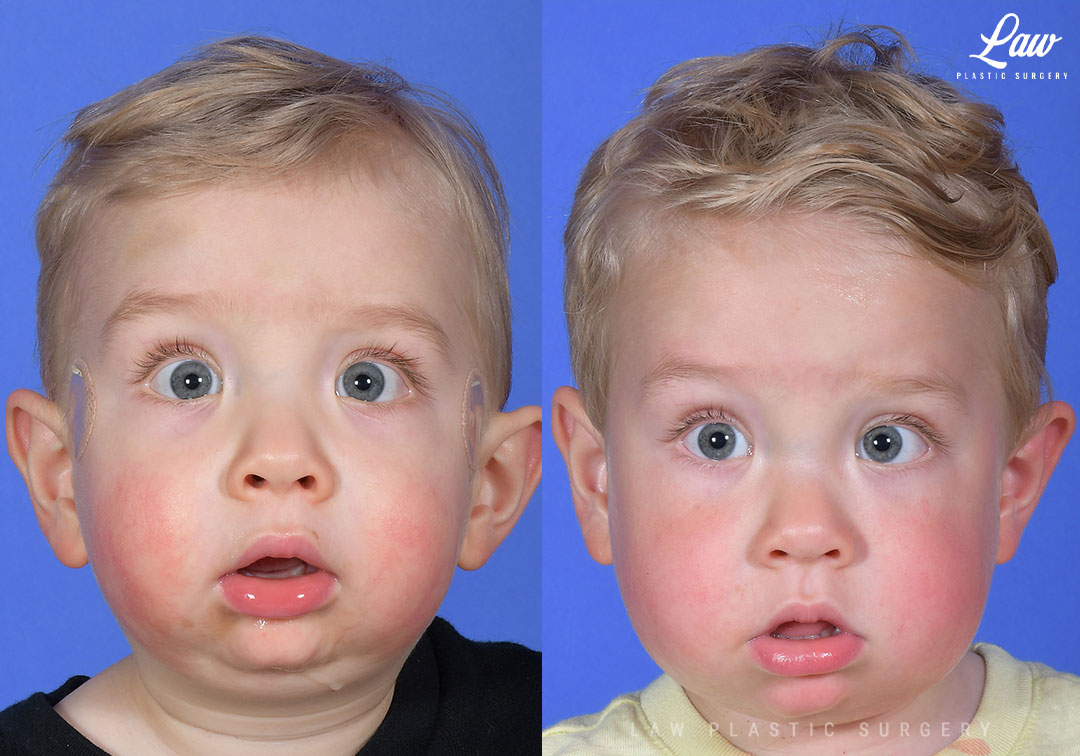
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
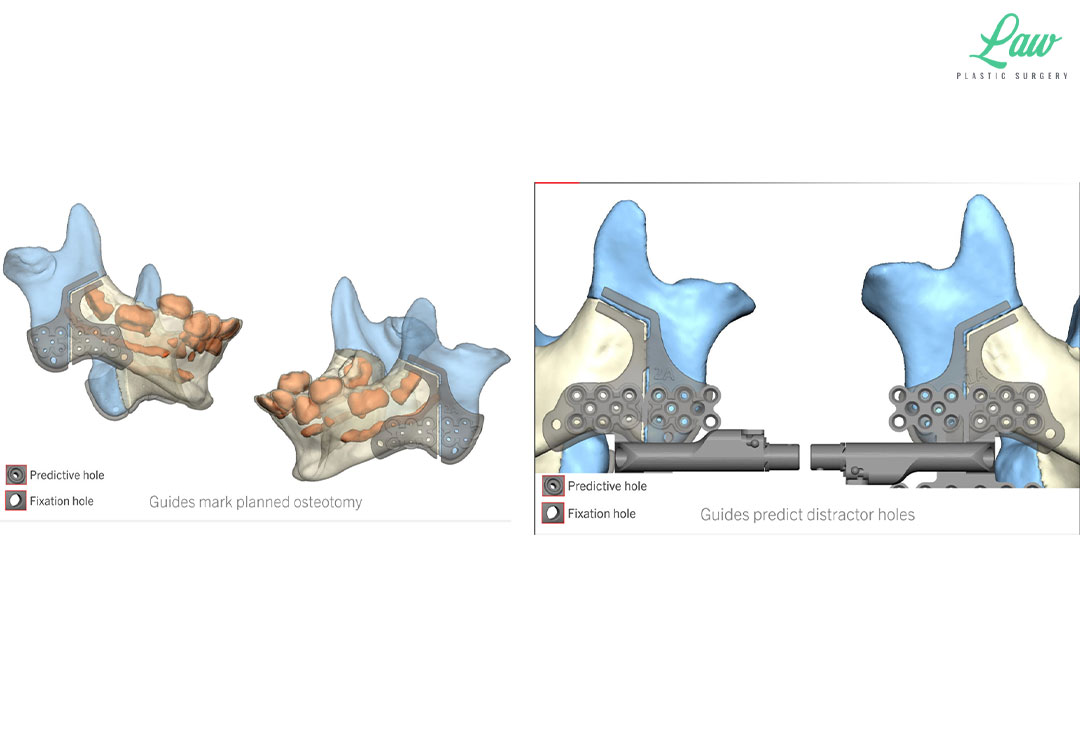
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
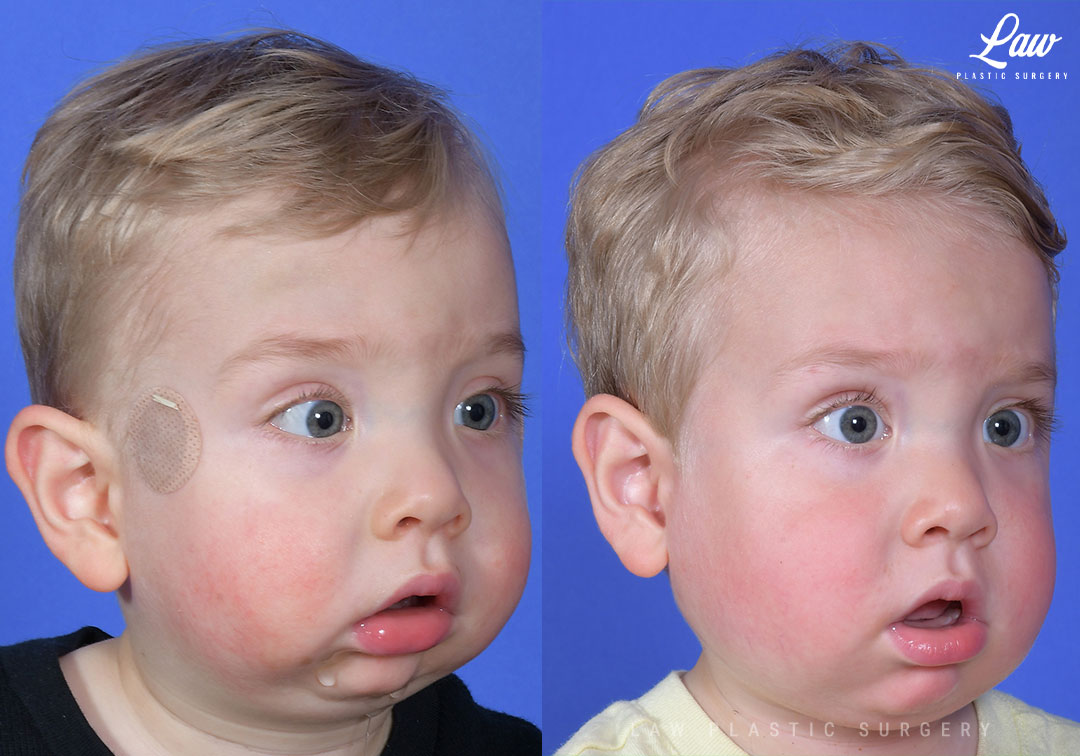
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
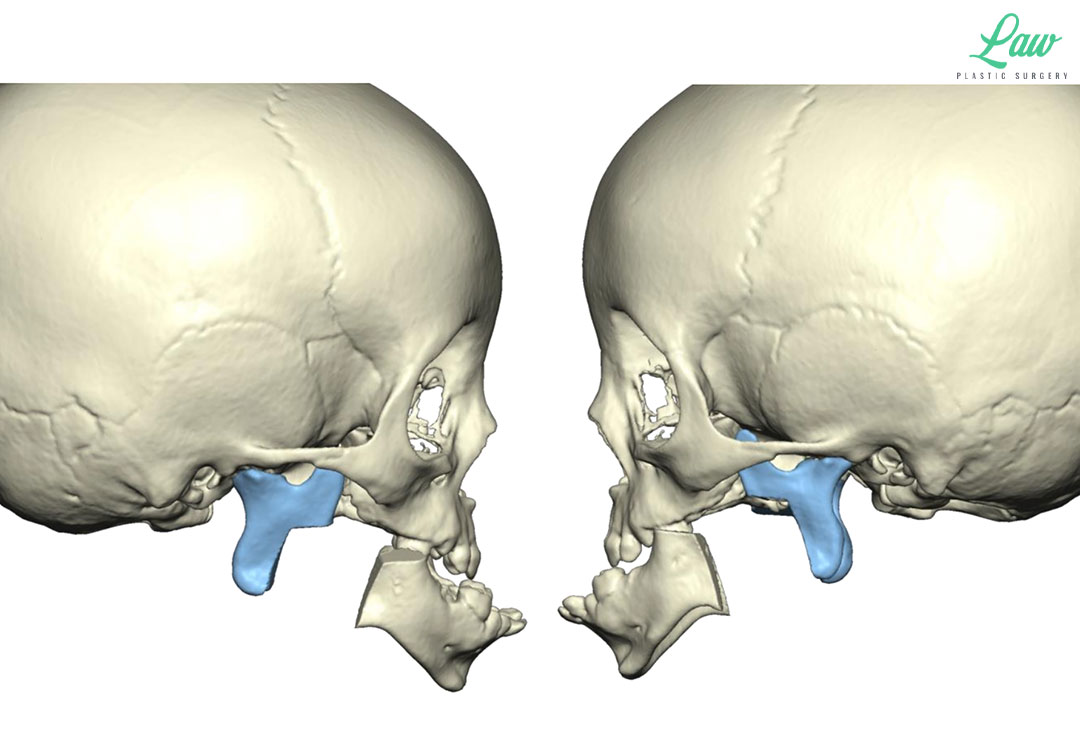
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
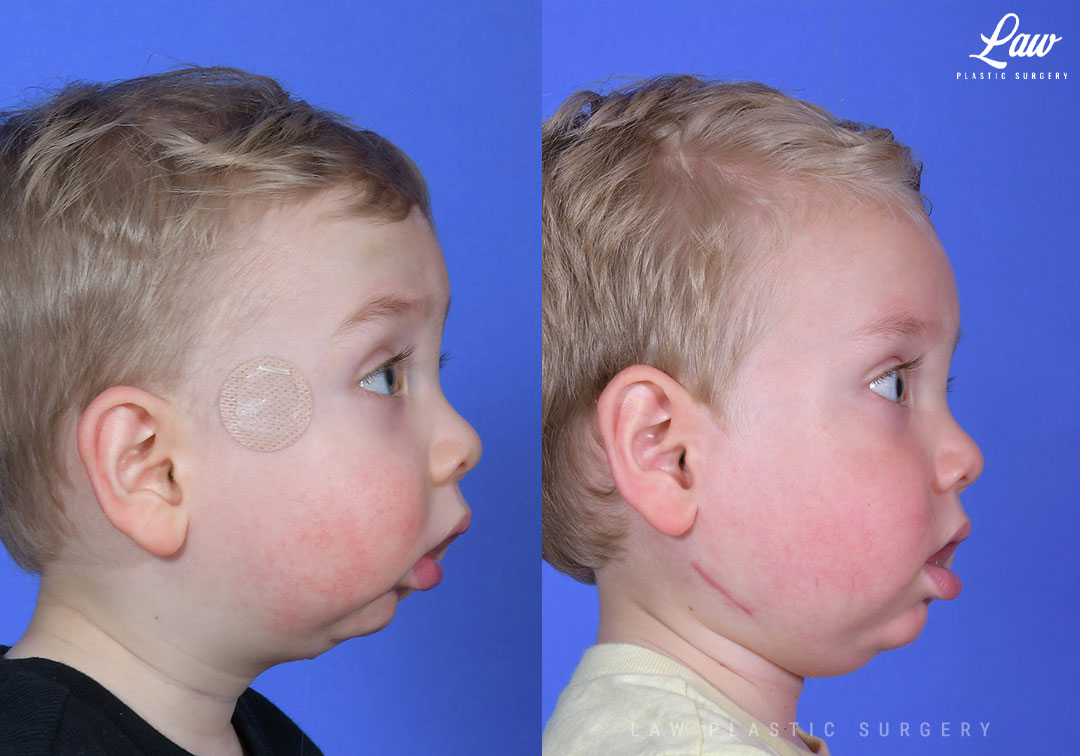
Jaw Distraction Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
What is Pierre Robin Sequence/Syndrome?
When the mandible is small and set too far back (microretrognathic),
–> the tongue falls back into the airway (glossoptosis),
–> and the airway is obstructed by the tongue.
The tongue can sometimes also be in the way of the palate as it closes, so a cleft palate may be present as well.
The treatment options include:
1) positioning on the baby’s stomach to let the tongue fall forward,
2) an oral airway plate to keep the tongue from falling back,
3) tongue-lip adhesion to pull the tongue forward,
4) jaw distraction to carry the tongue forward as the mandible is pushed forward,
5) nasopharyngeal airway or tracheostomy to bypass the obstruction.
Here, distraction was done when other options had not done enough.
3D guides helped us to minimize risks to the tooth buds and inferior alveolar nerve.
After just a few days, he was able to be off of his home CPAP, and he has started catching back up with his growth and milestones.
