Cleft Lip Repair, Primary Bilateral Repair Before & After Photos
Cleft Lip Repair, Primary Bilateral Before & After 1
The lip from either side of the cleft is repaired in the midline, with attempt made to reconstruct a more normal appearance of the lip.
At the first surgery, some repair is performed on the nose as well to lengthen the columella and improve the appearance and function of the nasal passage.
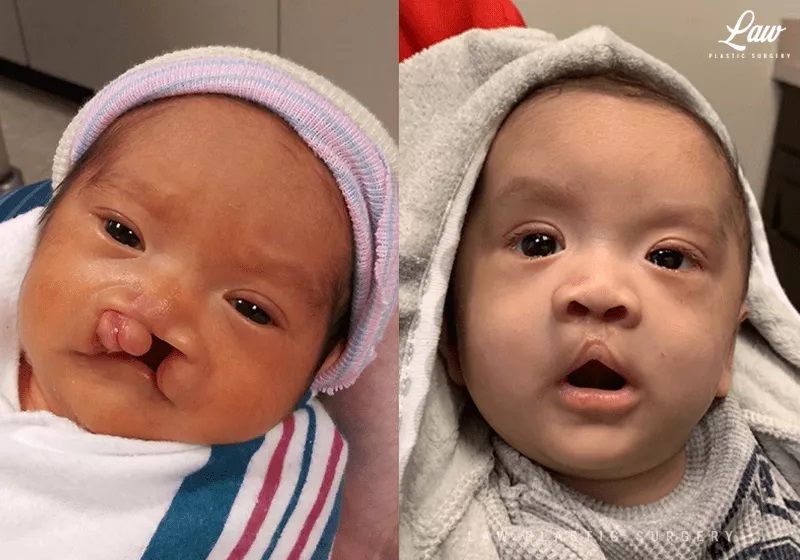
Cleft Lip Repair, Primary Bilateral Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Cleft Lip Repair, Primary Bilateral Before & After 2
The orbicularis oris muscle normally completes a ring around the mouth, allowing one to eat without food spilling out, and drinking through and straw.
In bilateral clefts, there is no muscle in the central portion, so the muscle must be brought all the way across from the sides.
This restores function, and helps to bring the premaxilla back in line with the lateral maxillary arches.
Elongation of the columella was also performed in the initial operation to reduce the flat and wide nasal appearance usually seen with bilateral cleft patients.
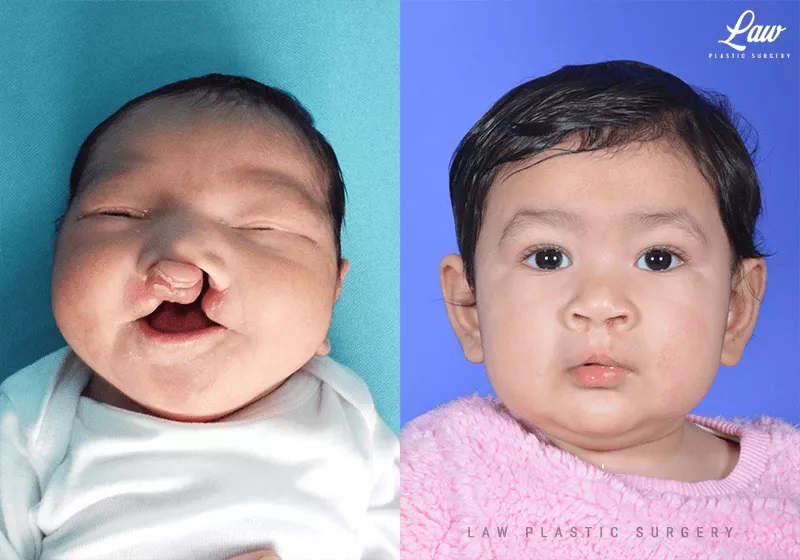
Cleft Lip Repair, Primary Bilateral Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Cleft Lip Repair, Primary Bilateral Before & After 3
The first year of life is often a stressful one for any family.
Our patients born with a cleft of the lip and/or palate – and their families – have additional worries about surgery, recovery, doctors’ visits, bills, time away from work, attention away from other siblings and family, and so much more.
Remembering all of that is part of the joy of our follow-ups.
We get to see the other side: the trips to Disney, starting school, going to prom, getting married, and then coming back to visit with kids of their own!
Witnessing the pure love of parents with their children – kindles the soul (paraphrasing Seneca).

Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
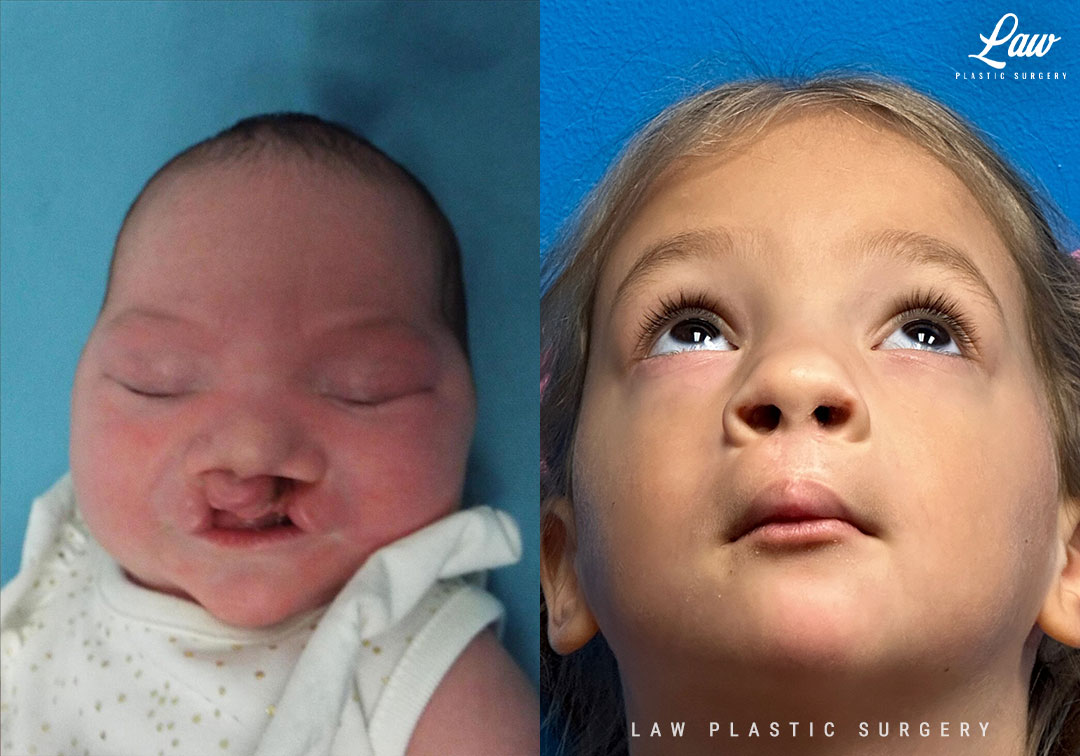
Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Cleft Lip Repair, Primary Bilateral Before & After 4
Repair of the orbicularis oris muscle early on helps to bring the central part of the palate and gums back in line with the rest of the gums over time. He did also have wider, thicker scars early on.
This is common in patients with thicker, darker skin. These scars improved gradually over time with massage and a steroid injection. He’s now happy, thriving, and only returning for annual visits until it is time for bone graft surgery.
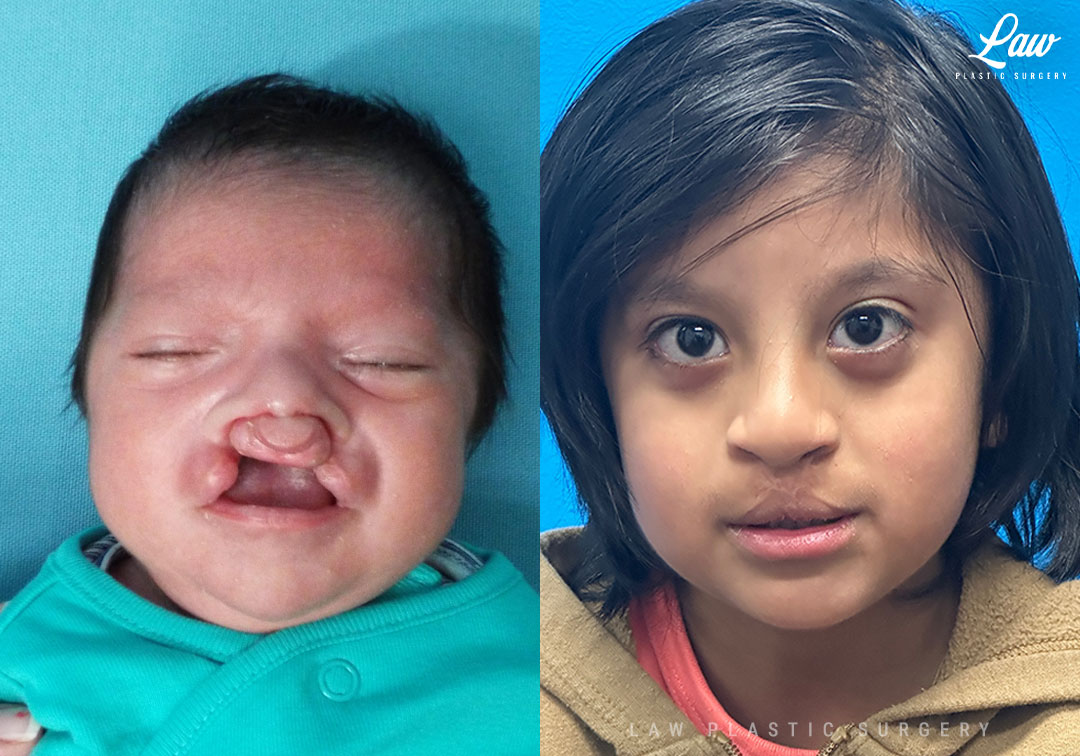
Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
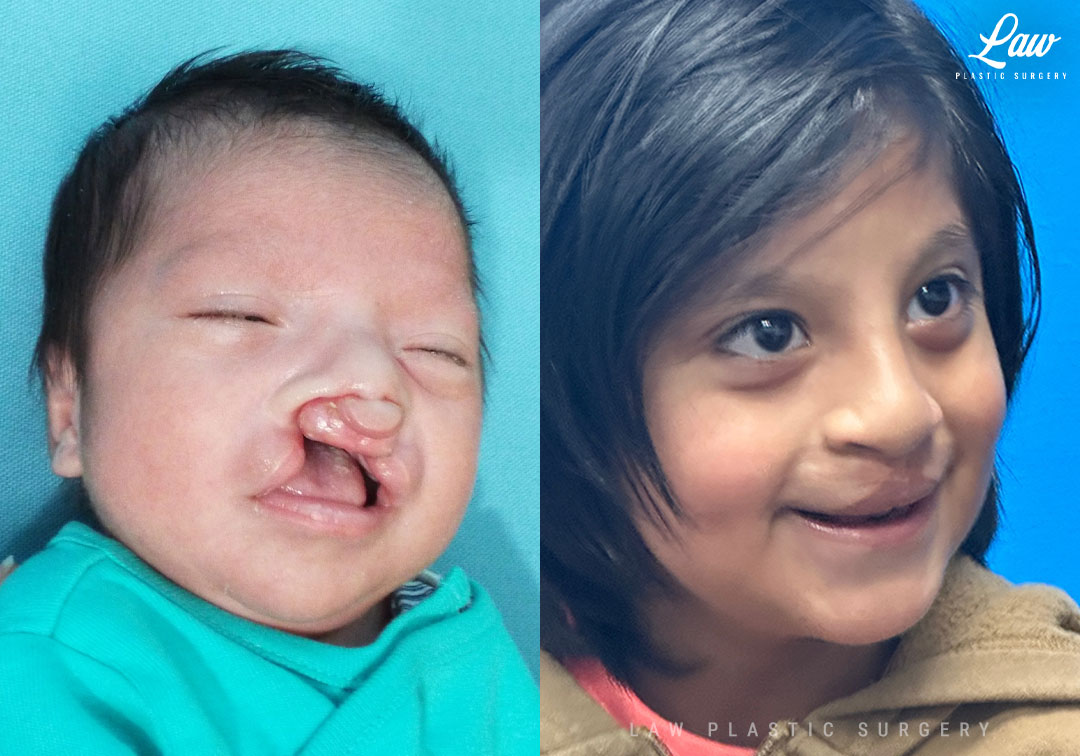
Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.

Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Cleft Lip Repair, Primary Bilateral Before & After 5
Most clefts are due to random chance in the first couple months after conception.
Normally there is nothing that the parents or families could have done any differently to prevent it. (Some things like smoking, alcohol, or other drugs, can slightly increase the odds.)
The premaxilla is the central part of the upper jaw. It extends from the forehead and nose, growing down from the frontonasal prominence.
From the sides, the lateral maxillary prominences come towards the middle to join with the frontonasal prominence.
When the lip doesn’t fuse on one side, a unilateral cleft lip is seen.
When both sides don’t fuse, a bilateral cleft lip occurs.
When the maxillary prominences don’t meet on the inside of the mouth, that is when a cleft palate occurs. (Specifically, of the secondary palate, the part posterior to the premaxilla.)
This sweet child is seen at 1 month after lip repair, eating well and thriving!
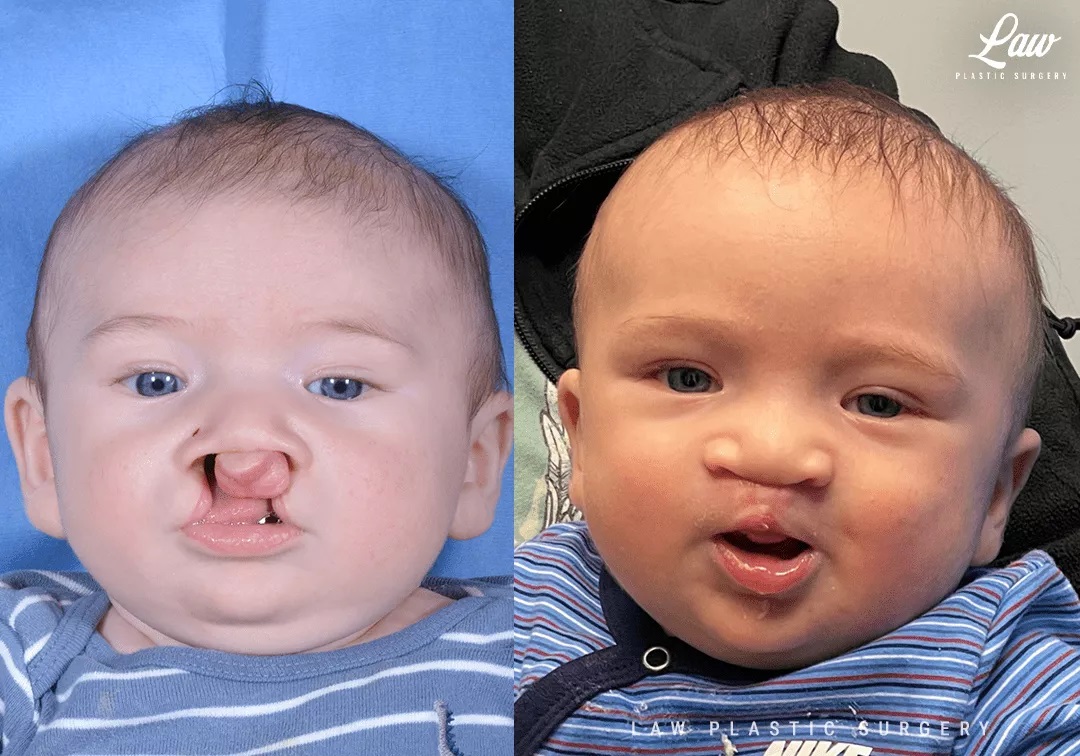
Cleft Lip Repair, Primary Bilateral Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
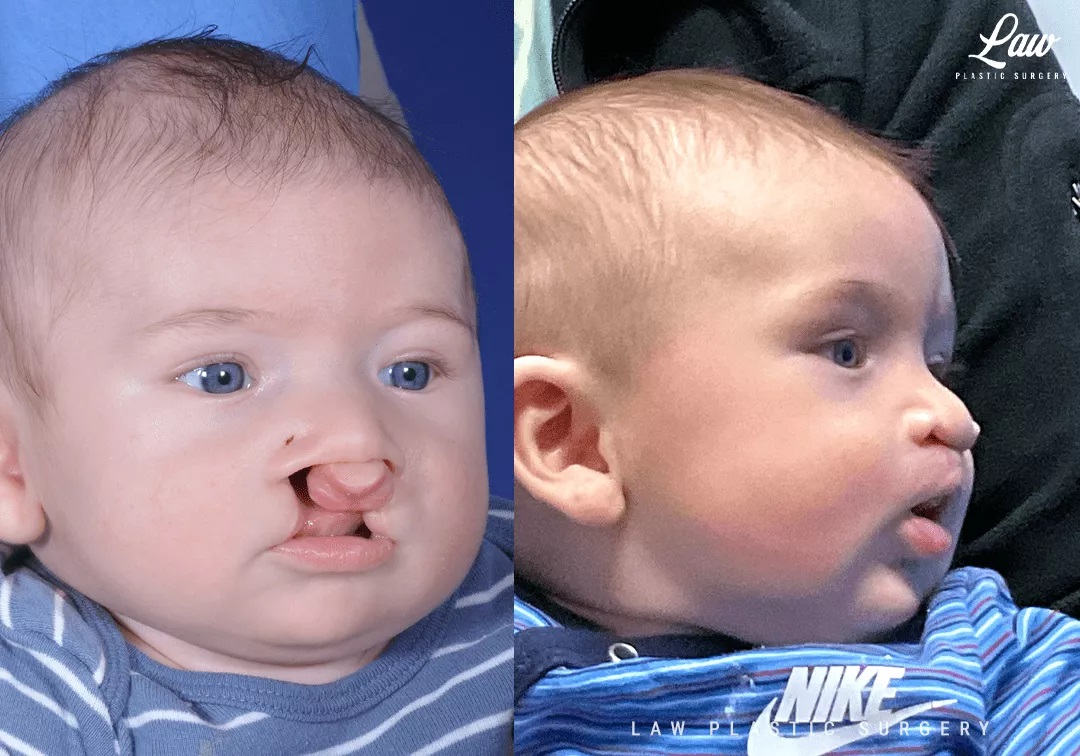
Cleft Lip Repair, Primary Bilateral Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
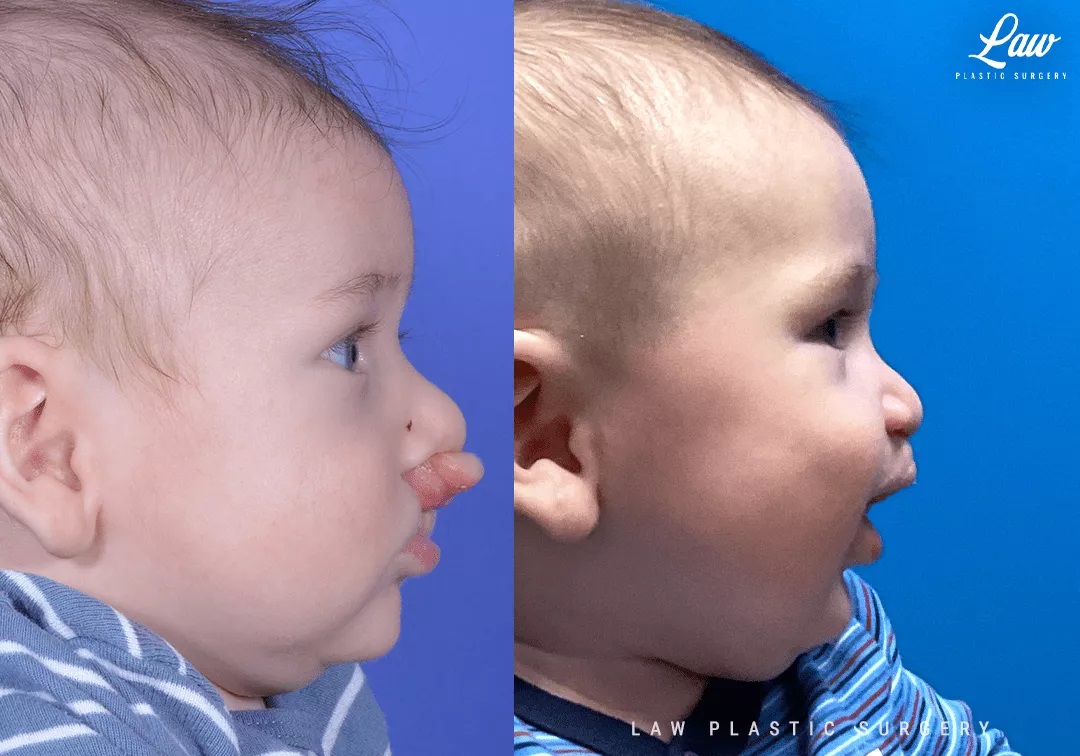
Cleft Lip Repair, Primary Bilateral Before and After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Cleft Lip Repair, Primary Bilateral Before & After 6
Cleft lip repair normally is offered at 3-6 months of age.
Palate repair then follows at 9-12 months of age as speech development speeds up. This can also be a good time to perform a tip rhinoplasty while under the same anesthetic, to bring the nasal tip closer together, and helping to round out the nostrils to have more height medially.
Ideally we then wait to perform a definitive rhinoplasty at full skeletal maturity and after any orthognathic surgery that may need to be done to align the upper and lower teeth.
Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
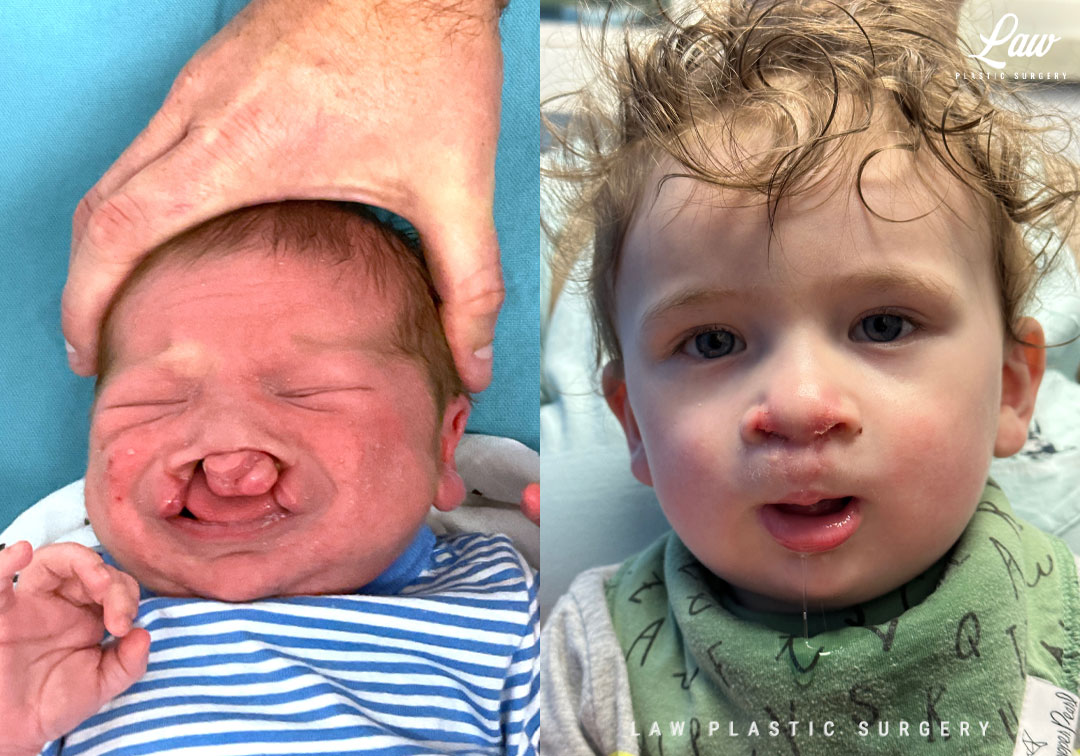
Cleft Lip Repair, Primary Bilateral Before & After 7
While some patients disappear for years at a time, follow-ups every 1-2 years are a good time for a few things:
– Evaluating for and reassuring about expected, common issues (like a small nasolabial fistula until bone grafting), versus treating early any abnormal delays with speech development or bone growth.
– Providing personal support and a sense of home and belonging for patients and families. We have a number of patients and families who we connect families with, and several other foundations and charities that combine to provide a strong network for our patients and families.
– Interacting with the team outside of surgeries to develop trust and comfort.
– Ensuring all the right specialists are being seen at the right time. This includes ENT’s, speech therapists, dentists and orthodontists, genetic counselors, psychiatrists and psychologists, and more.
We do operate a little differently than most team clinics. Rather than seeing every specialist on a certain day in one clinic, we see cleft and craniofacial patients every day, and then help coordinate with other specialists as needed.
There are pros and cons to this, but our families seem to appreciate fewer co-pays if not needed, fewer unproductive visits where the actual dental or other care can’t be provided, and shorter trips that are easier to schedule.
We also pride ourselves in taking care of patients of all ages. This has given us a longer perspective on treatment outcomes, more flexibility in timing surgeries for our teenagers and young adults, and accepting insurance payment for our older patients who may need treatment at adult hospitals.

Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
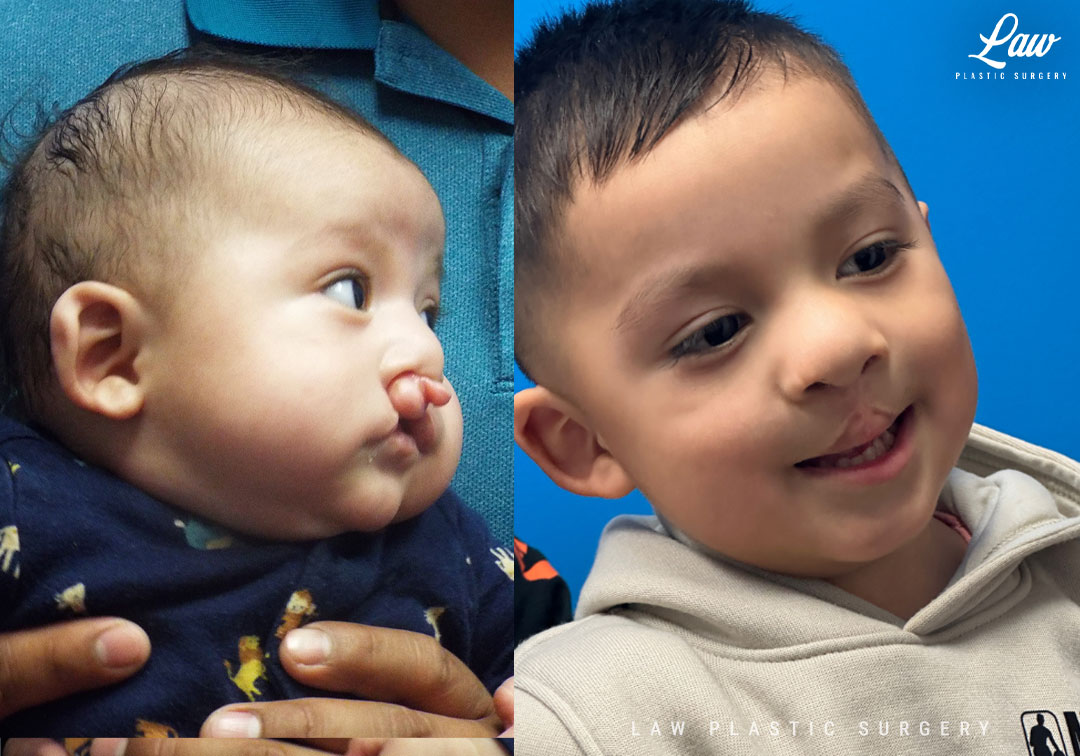
Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
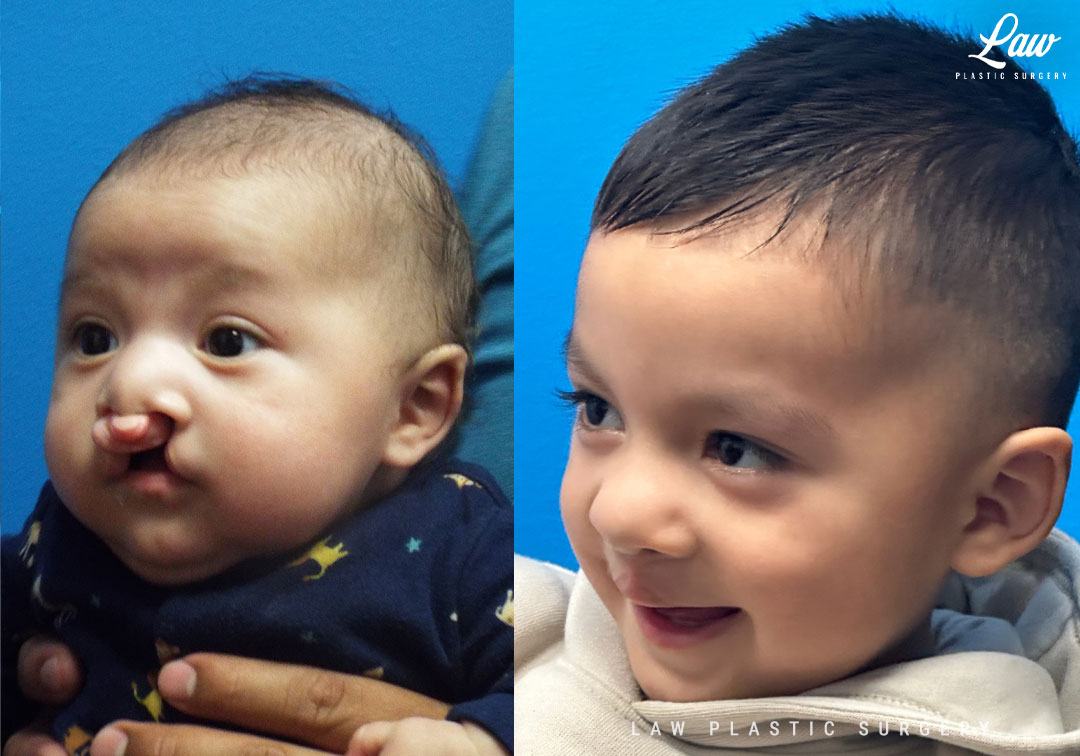
Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
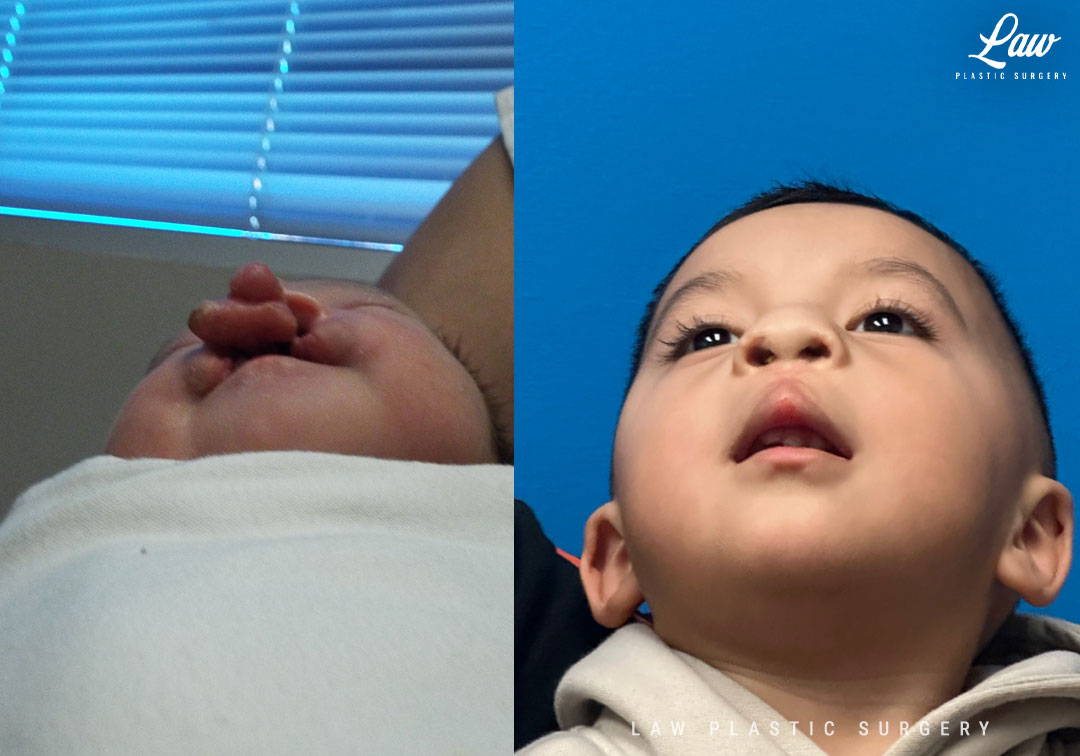
Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Cleft Lip Repair, Primary Bilateral Before & After 8
Some of the initial tightness of the on-table repair relaxes as the premaxilla falls back into place if needed, and as the absorbable sutures give way.
I have been happy with the results of
1) minimizing/eliminating incisions at the alar sill and base (especially for patients prone to thick and dark scars!), and also
2) recruiting the medial crurae in the initial cleft lip/nasal repair to help with columellar height and tip projection.
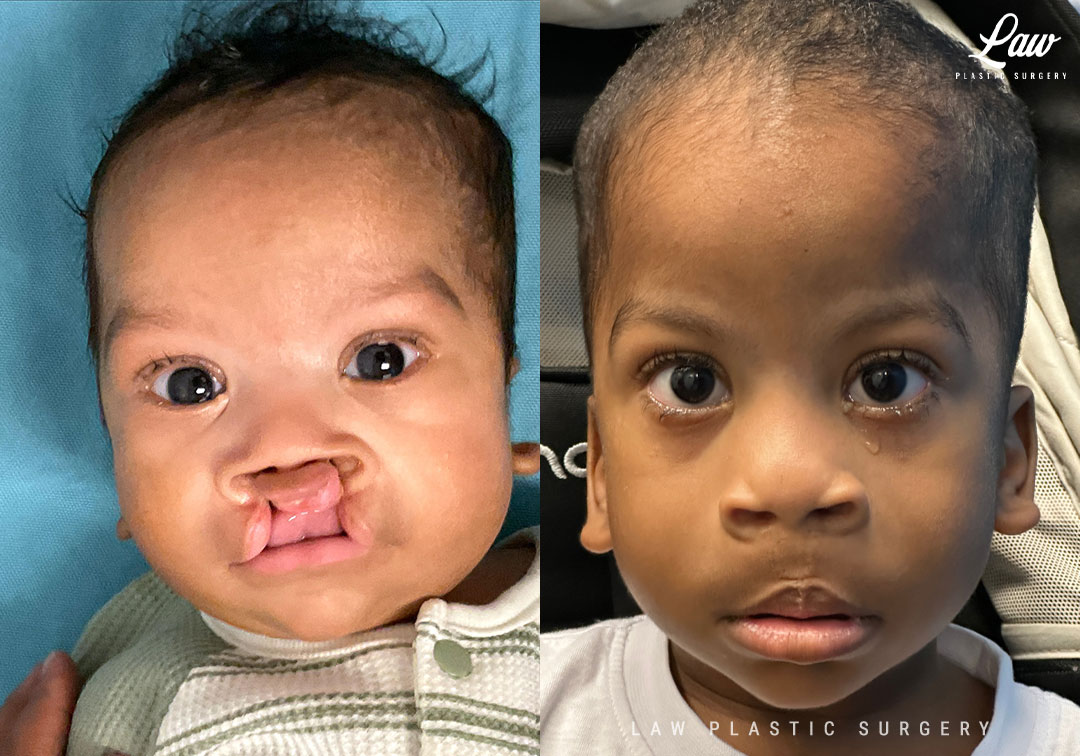
Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
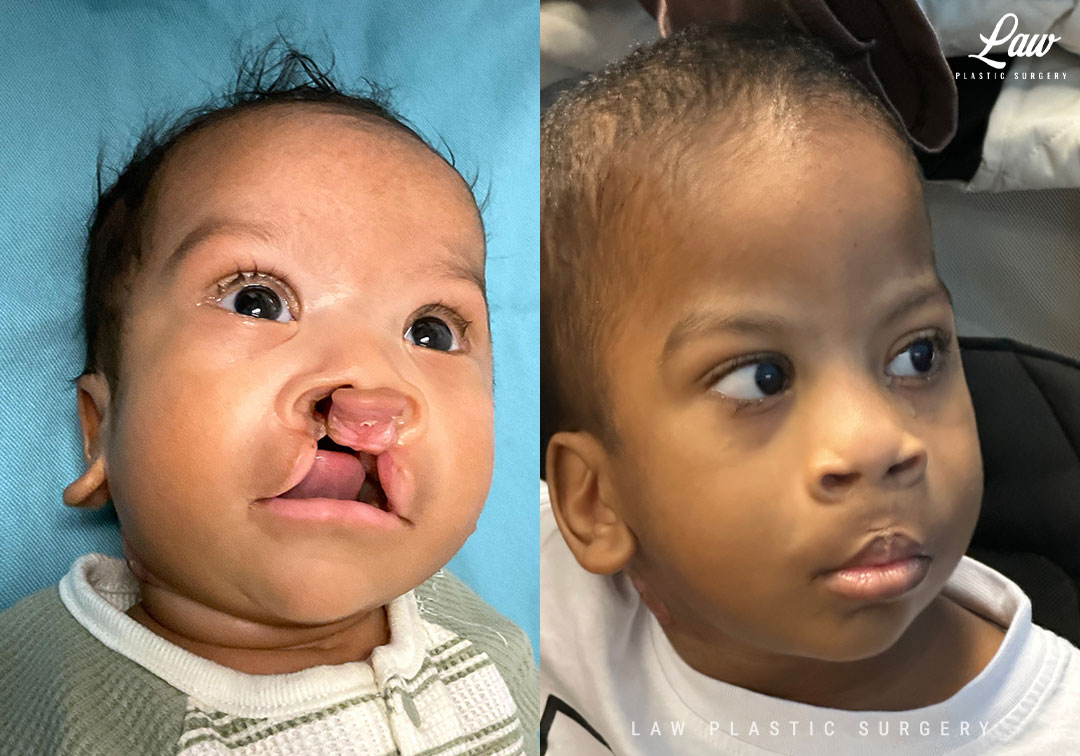
Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Cleft Lip Repair, Primary Bilateral Before & After 9
Some centers have moved this up to 2-4 weeks, once the child is doing well and gaining weight. There may be some benefits to feeding and weight gain doing this on the earlier side.
On the other hand, some other surgeons are pushing the cleft lip repair back towards 9-12 months. This is to mitigate concerns about the effects of general anesthesia on the developing brain.
I get into these details with families in prenatal and initial visits, and work with them to decide on what’s best for them and their child.
For this patient, the lip was repaired at 3 months, and she is seen in her after photos in preparation for her cleft palate repair at 9 months.
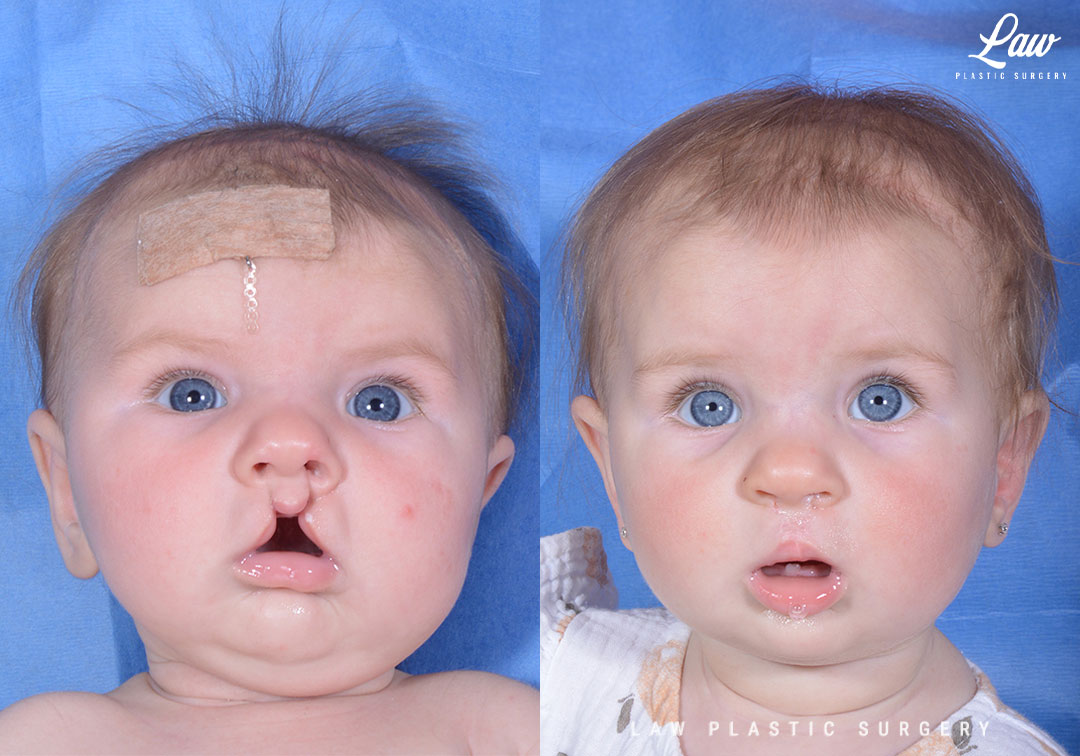
Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
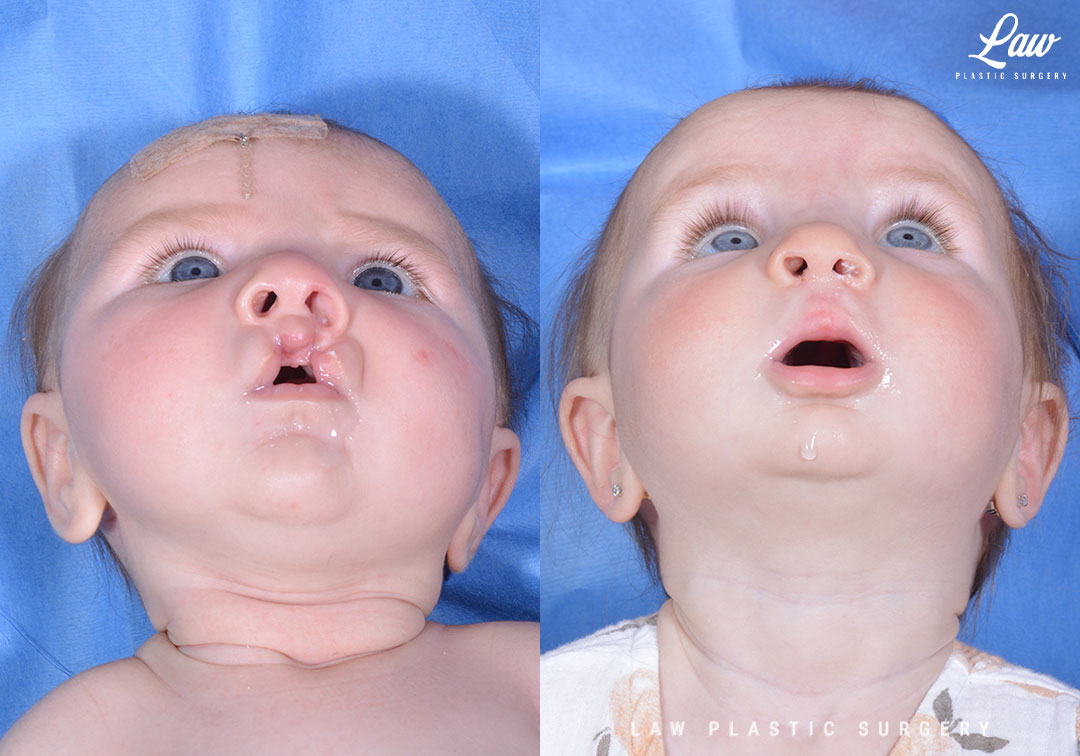
Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Cleft Lip Repair, Primary Bilateral Before & After 10
Annual visits in the 4-6 year range center around speech. Kids are now able to participate more with an evaluation. Parents often also have a few videos of their kids speaking at home to give some more context and information to go off of.
Rarely, patients have come as far as possible with speech therapy, but anatomically need a lengthening of the palate, or closure of the space in the back directly with a pharyngeal flap.
At this visit, we also start talking about teeth, orthodontics, and getting ready for bone grafting to fill the gap in bone. That grafted bone then gives a place in which the teeth around it can live happily and securely.
Also rarely, we also discuss a revision of a cleft lip or nose repair. Sometimes the septum of the nose is causing severe nasal obstruction. Sometimes patients had poor healing from their original surgery due to an infection or a fall.
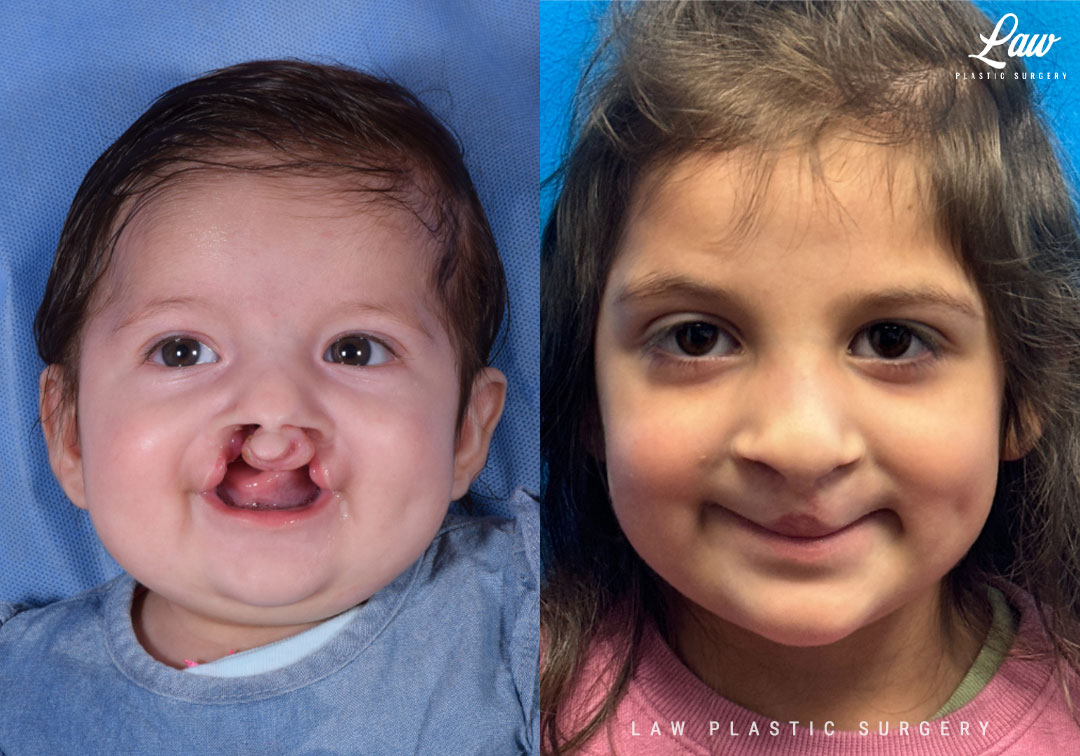
Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
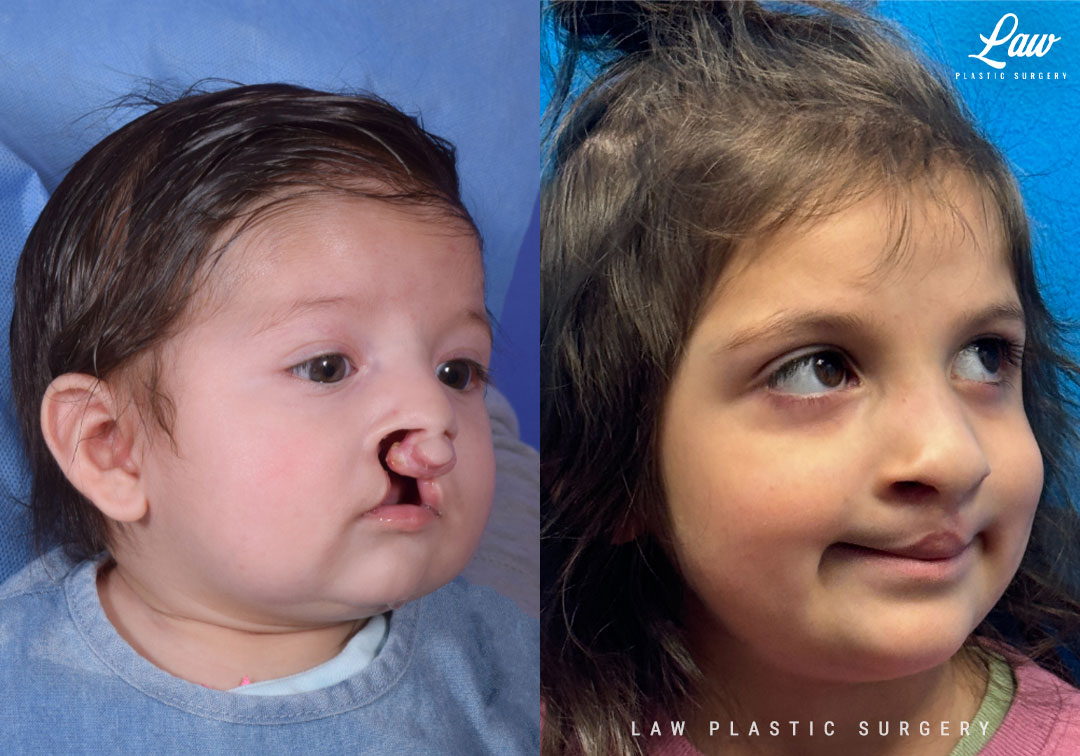
Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
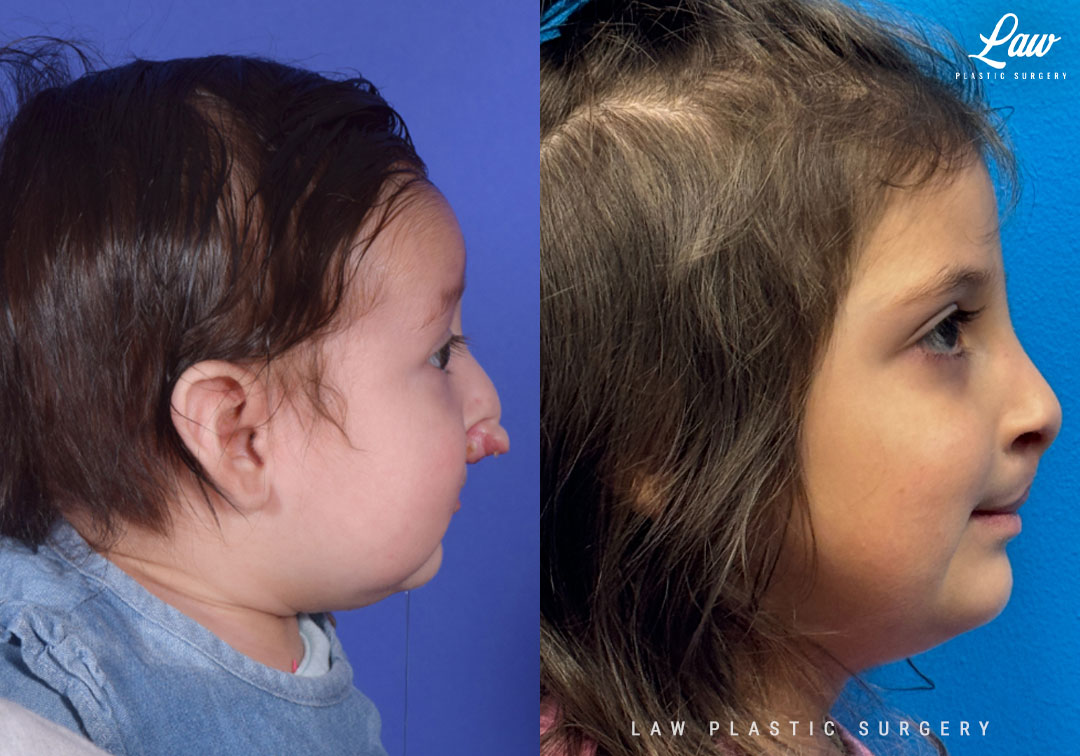
Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
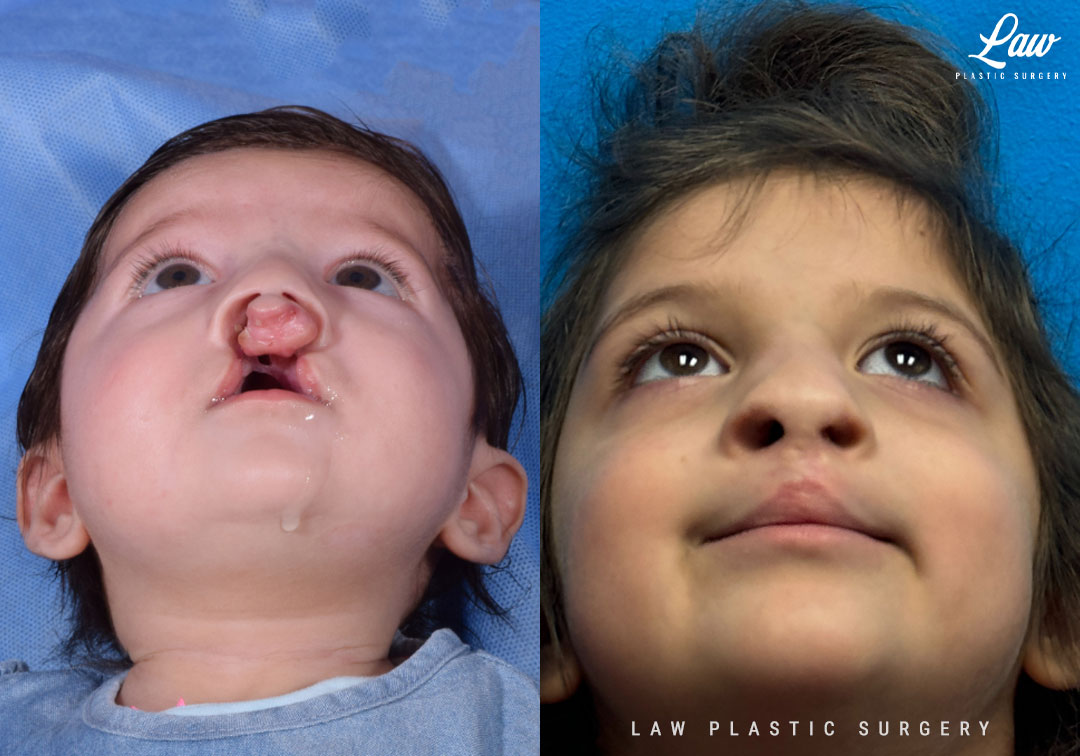
Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
Cleft Lip Repair, Primary Bilateral Before & After 11
NAM can help to ease this into place, but it can be challenging to get just right.
Sometimes we have patients with multiple and less common cleft patterns, like a Tessier #7 macrostomia for this sweet patient.
Stay tuned for more updates, but we treat each area in turn, to minimize the risk of over-challenging the blood flow, to give each area the best chance to heal well.
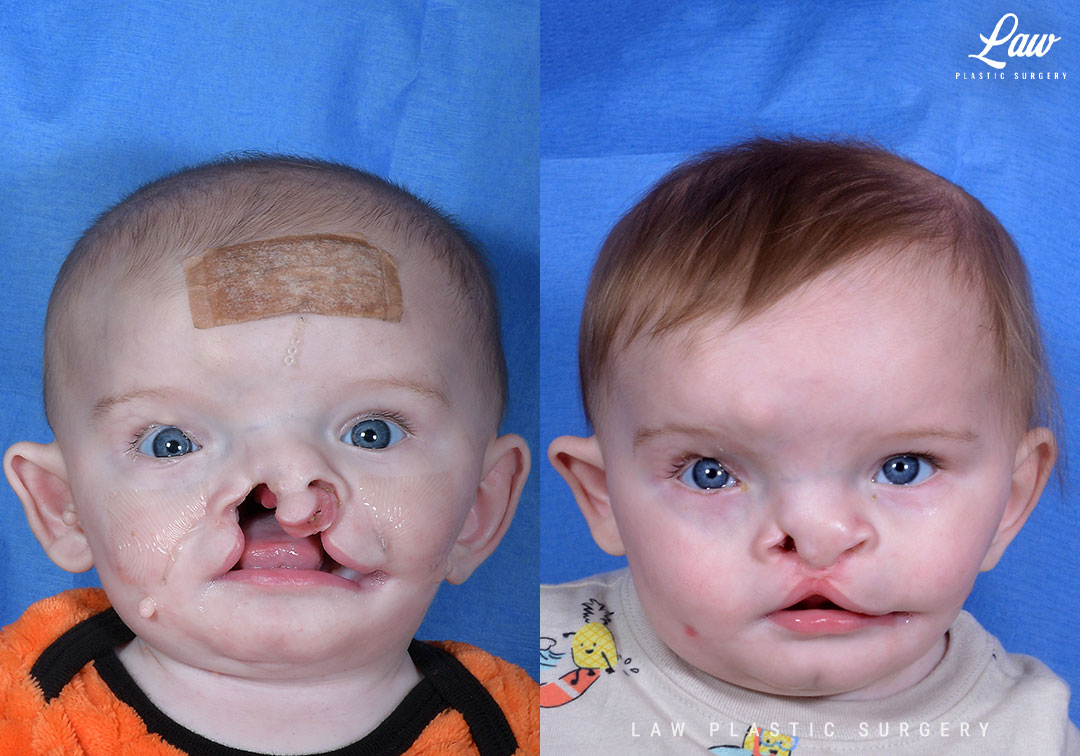
Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
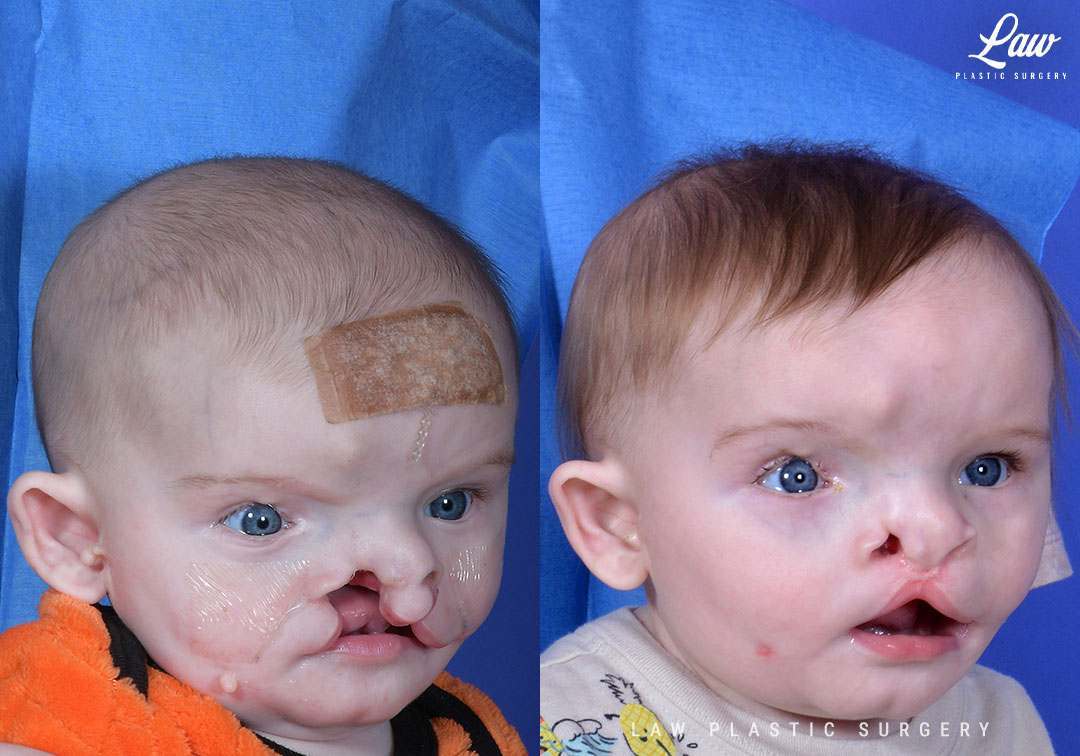
Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
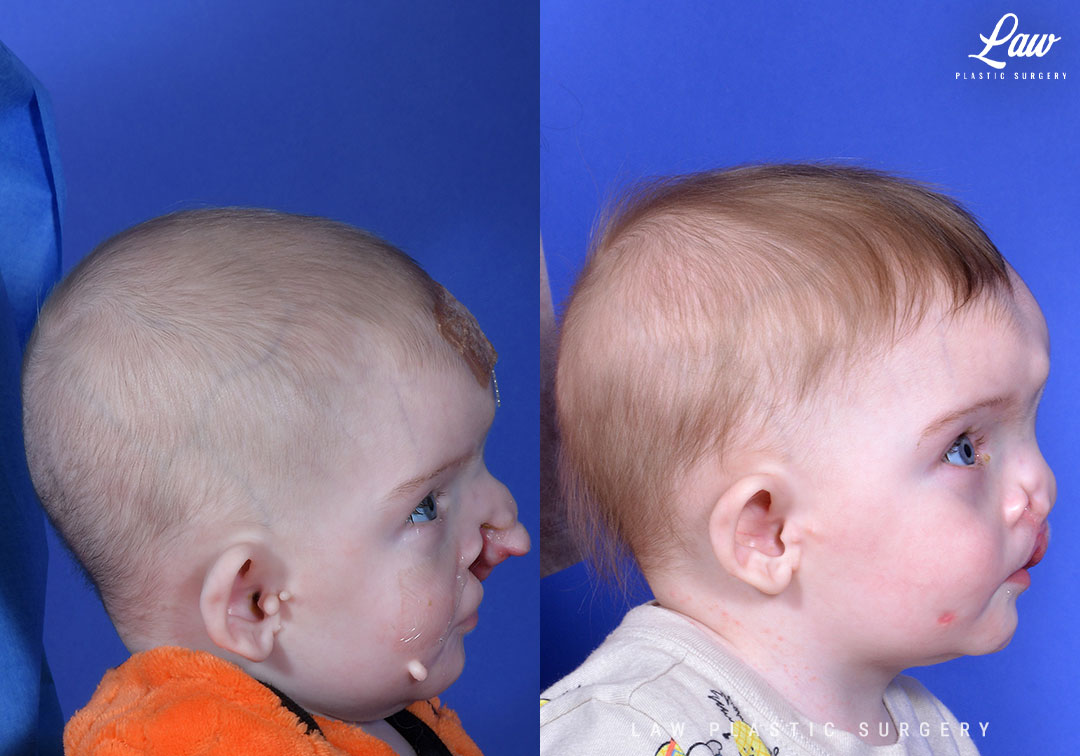
Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
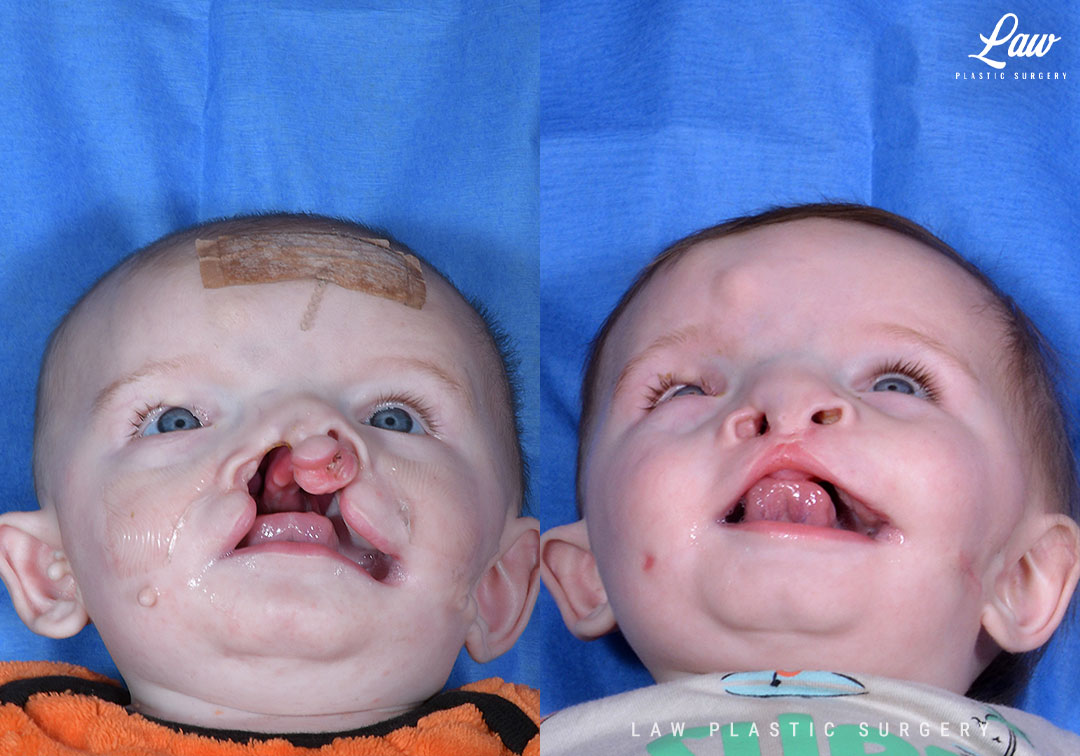
Cleft Lip Repair Before & After Photo. Surgery performed in Dallas, TX at Law Plastic Surgery.
